Facioscapulohumeral muscular dystrophy
| Facioscapulohumeral muscular dystrophy | |
|---|---|
| Other names | Landouzy–Dejerine muscular dystrophy, FSHMD, FSH |
 | |
| A diagram showing the muscles commonly affected by FSHD | |
| Pronunciation | |
| Management | Physical therapy, bracing, reconstructive surgery |
| Medication | Clinical trials ongoing |
| Prognosis | Progressive, unaffected life expectancy |
| Frequency | Up to 1/8,333[2] |
Facioscapulohumeral muscular dystrophy (FSHD) is a type of
FSHD is caused by a
Signs, symptoms, and diagnostic tests can suggest FSHD;
FSHD was first distinguished as a disease in the 1870s and 1880s when French physicians Louis Théophile Joseph Landouzy and Joseph Jules Dejerine followed a family affected by it, thus the initial name Landouzy–Dejerine muscular dystrophy. Their work is predated by descriptions of probable individual FSHD cases.[16][17][18] The significance of D4Z4 contraction on chromosome 4 was established in the 1990s. The DUX4 gene was discovered in 1999, found to be expressed and toxic in 2007, and in 2010 the genetic mechanism causing its expression was elucidated. In 2012, the gene most frequently mutated in FSHD2 was identified. In 2019, the first drug designed to counteract DUX4 expression entered clinical trials.[19]
Signs and symptoms
Classically, weakness develops in the face, then the
Face
Weakness of the muscles of the face is the most distinguishing sign of FSHD.
Weakness of facial muscles contributes to difficulty pronouncing words.[34] Facial expressions can appear diminished, arrogant, grumpy, or fatigued.[4] Muscles used for chewing and moving the eyes are not affected.[24][14] Difficulty swallowing is not typical, although can occur in advanced cases, which is at least in part due to facial muscle weakness.[35][34] FSHD is generally progressive, but it is not established whether facial weakness is progressive or stable throughout life.[36]
Shoulder, chest, and arm

After the facial weakness, weakness usually develops in the muscles of the chest and those that span from scapula to thorax. Symptoms involving the shoulder, such as difficulty working with the arms overhead, are the initial complaint in 80% of cases.
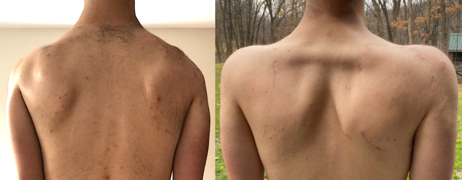
Severe muscle wasting can make bones and spared shoulder muscles very visible, a characteristic example being the "poly-hill" sign elicited by arm elevation.
Also affected is the chest, particularly the parts of the
Lower body and trunk
After the upper body, weakness can next appear in either the pelvis, or it "skips" the pelvis and involves the
Weakness can also occur in the
Non-muscular
The most common non-musculoskeletal manifestation of FSHD is abnormalities in the small arteries (
Scoliosis can occur, thought to result from weakness of abdominal, hip extensor, and spinal muscles.[46][47] Conversely, scoliosis can be viewed as a compensatory mechanism to weakness.[46] Breathing can be affected, associated with kyphoscoliosis and wheelchair use; it is seen in one-third of wheelchair-using patients.[2] However, ventilator support (nocturnal or diurnal) is needed in only 1% of cases.[2][48] Although there are reports of increased risk of cardiac arrhythmias, general consensus is that the heart is not affected.[14]
Genetics

The genetics of FSHD is complex.
DUX4 and the D4Z4 repeat array
DUX4 resides within the D4Z4
The subtelomeric region of chromosome 10q contains a tandem repeat structure highly homologous (99% identical) to 4q35,[8][51] containing "D4Z4-like" repeats with protein-coding regions identical to DUX4 (D10Z10 repeats and DUX4L10, respectively).[8][56] Because 10q usually lacks a polyadenylation sequence, it is usually not implicated in disease. However, chromosomal rearrangements can occur between 4q and 10q repeat arrays, and involvement in disease is possible if a 4q D4Z4 repeat and polyadenylation signal are transferred onto 10q,[57][8][58] or if rearrangement causes FSHD1.
D4Z4 repeat array types are subclassified into 4qA and 4qB alleles, with only 4qA alleles causing disease. 4qA alleles are defined by a specific sequence of DNA immediately downstream to the D4Z4 repeat array: a 260 base pair region named pLAM, followed by a 6,200 base pair beta satellite region.[9][59] 4qA and 4qB alleles, together, are able to be subdivided into at least 17 types,[51] based on the DNA upstream from the D4Z4 repeat array, the presence/absence of restriction enzyme sites within D4Z4, the size of the last D4Z4 repeat element, and the DNA present downstream to the D4Z4 repeat array.[59] For example, the most common 4qA allele, 4A161, has 161 nucleotides in the region upstream from the D4Z4 repeat array,[27] and can in turn be subdivided into 4A161S and 4A161L (short and long), which are characterized by a flanking D4Z4 repeat units of 300 nucleotides and 1,900 nucleotides, respectively.[59]
DUX4 consists of three
| FSHD1 | ↓ | ↑ | ↓ | |
| FSHD2* | ↓ | ↑ | ↓ | ↑ |
| *Chromatin profiles not fully characterized for DNMT3B mutation[55] | ||||
FSHD1
FSHD involving deletion of D4Z4 repeats (termed 'D4Z4 contraction') on 4q is classified as FSHD1, which accounts for 95% of FSHD cases.
It has been proposed that FSHD1 undergoes
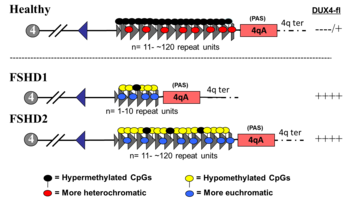
FSHD2
FSHD with a D4Z4 array repeat size of 11 or greater is classified as FSHD2, which constitutes 5% of FSHD cases.
For FSHD2 associated with SMCHD1 or DNMT3B mutation, only one allele needs to be abnormal. These FSHD2-causative genes are not located next to the required D4Z4 array/4qA allele within the genome, and are thus inherited independently, resulting in a biallelic digenic inheritance pattern. For example, one parent without FSHD can pass on an SMCHD1 mutation, and the other parent, also without FSHD, can pass on a borderline-shortened D4Z4/4qA allele, bearing a child with FSHD2.[68][70] For FSHD2 associated with LRIF1 mutation, both LRIF1 alleles need to be mutated, which theoretically yields an even more complex inheritance pattern, termed trialleic digenic.[71][72]
Two ends of a disease spectrum
FSHD1 and FSHD2 have been traditionally viewed as separate entities with distinct genetic causes (albeit, the downstream genetic mechanisms merge).[73] Alternatively, the genetic causes of FSHD1 and FSHD2 can be viewed as risk factors, each contributing to an FSHD disease spectrum.[73] Not rarely, an affected individual seems to have contributions from both.[63] For example, in those with FSHD2, although they have do not have a 4qA allele with D4Z4 repeat number less than 11, they still have one less than 30 (shorter than the upper limit seen in the general population), suggesting that a large number of D4Z4 repeats can prevent the effects of an SMCHD1 mutation.[63][10] Further studies may be needed to determine the upper limit of D4Z4 repeats in FSHD2.[63]
In those with FSHD1 and FSHD2, that is, having 10 or fewer repeats with an adjacent 4qA allele and an SMCHD1 mutation, the disease manifests more severely, illustrating that the effects of each mutation are additive.[74] A combined FSHD1/FSHD2 presentation is most common in those with 9 - 10 repeats. A possible explanation is that a sizable portion of the general population has 9 - 10 repeats with difficult to detect or no disease, yet with the additive effect of an SMCHD1 mutation, symptoms are severe enough for a diagnosis to be made.[63] The 9 - 10 repeat size can be considered as an overlap zone between FSHD1 and FSDH2.[63]
Pathophysiology
Molecular

As of 2020, there seems to be a consensus that aberrant expression of DUX4 in muscle is the cause of FSHD.
It remains an area of active research how DUX4 protein causes muscle damage.
The cellular
Another study found that DUX4 expression in muscle cells led to the recruitment and alteration of
A single study implicated RIPK3 in DUX4-mediated cell death.[80]
Muscle histology
Unlike other muscular dystrophies, early muscle biopsies show only mild degrees of
Muscle involvement pattern
Why certain muscles are preferentially affected in FSHD remains unknown. There are multiple trends of involvement seen in FSHD, possibly hinting at underlying pathophysiology. Individual muscles can weaken while adjacent muscles remain strong.[83] The right shoulder and arm muscles are more often affected than the left upper extremity muscles, a pattern also seen in Poland syndrome and hereditary neuralgic amyotrophy; this could reflect a genetic, developmental/anatomic, or functional-related mechanism.[24][25] The deltoid is often spared, which is not seen in any other condition that affects the muscles around the scapula.[36]

Medical imaging (CT and MRI) have shown muscle involvement not readily apparent otherwise[37]
- A single MRI study shows the teres major muscle to be commonly affected.[38]
- The
- Of the quadriceps muscles, the rectus femoris is preferentially affected[84]
- Of the
- The iliopsoas, a hip flexor muscle, is very often spared.[85][2]
Retinopathy
Tortuosity of the retinal arterioles, and less often microaneurysms and telangiectasia, are commonly found in FSHD.[42] Abnormalities of the capillaries and venules are not observed.[42] One theory for why the arterioles are selectively affected is that they contain smooth muscle.[42] The degree of D4Z4 contraction correlates to the severity of tortuosity of arterioles.[42] It has been hypothesized that retinopathy is due to DUX4-protein-induced modulation of the CXCR4–SDF1 axis, which has a role in endothelial tip cell morphology and vascular branching.[42]
Diagnosis
Genetic testing
Genetic testing is the
Assessing D4Z4 length
Measuring D4Z4 length is technically challenging due to the D4Z4 repeat array consisting of long, repetitive elements.[88] For example, NGS is not useful for assessing D4Z4 length, because it breaks DNA into fragments before reading them, and it is unclear from which D4Z4 repeat each sequenced fragment came.[4] In 2020, optical mapping became available for measuring D4Z4 array length, which is more precise and less labor-intensive than southern blot.[89] Molecular combing is also available for assessing D4Z4 array length.[90] These methods, which physical measure the size of the D4Z4 repeat array, require specially prepared high quality and high molecular weight genomic DNA (gDNA) from serum, increasing cost and reducing accessibility to testing.[91]

- D4Z4 repeats = (EcoRI length - 5) / 3.3
Sometimes 4q or 10q will have a combination of D4Z4 and D4Z4-like repeats due to DNA exchange between 4q and 10q, which can yield erroneous results, requiring more detailed workup.[51] Sometimes D4Z4 repeat array deletions can include the p13E-11 binding site, warranting use of alternate probes.[51][95]
Assessing methylation status
Methylation status of 4q35 is traditionally assessed after FSHD1 testing is negative. Methylation sensitive restriction enzyme (MSRE) digestion showing hypomethylation has long been considered diagnostic of FSHD2.[91] Other methylation assays have been proposed or used in research settings, including methylated DNA immunoprecipitation and bisulfite sequencing, but are not routinely used in clinical practice.[96][91] Bisulfite sequencing, if validated, would be valuable due to it being able to use lower quality DNA sources, such as those found in saliva.[91]
Auxiliary testing

Other tests can support the diagnosis of FSHD, although they are all less sensitive and less specific than genetic testing.[97][4] Nonetheless, they can rule out similar-appearing conditions.[14]
- Creatine kinase (CK) blood level is often ordered when muscle damage is suspected. CK is an enzyme found in muscle, leaking into the blood when muscles become damaged. In FSHD, CK level is normal to mildly elevated,[2] never exceeding five times the upper limit of normal.[4]
- Electromyogram (EMG) measures the electrical activity in the muscle. EMG can show nonspecific signs of muscle damage or irritability.[2]
- neuropathy rather than myopathy.[citation needed]
- biochemical tests are used for examination. Findings in FSHD are nonspecific, such as presence of white blood cells or variation in muscle fiber size. This test is rarely indicated.[2]
- T2-weighted MRI imaging can visualize muscle edema.[citation needed] MRI can help differentiate FSHD from other muscle diseases on the basis of the pattern of muscles involved, directing genetic testing.[37][38]
- Ultrasound (US) can be used in the evaluation of muscles.[98] US is effective at identifying fatty infiltration or scarring of muscles due to FSHD, manifesting as increased echogenicity (appearing brighter on ultrasound imaging).[98] Advantages of US, compared to MRI or computed tomography, include low cost and no radiation exposure. However, US has poorer evaluation of deeper muscles, and ultrasonic findings tend to be more operator-dependent.[98]
- Computed tomography (CT) imaging is not routinely used for muscle imaging due to significant radiation exposure and inferior characterization of soft tissues (ie, parts of the body other than bone).[98] However, muscle that is incidentally imaged by CT can appear atrophied and lower density, because fat is less dense than muscle.[98] CT has limited ability to detect the inflammatory changes of muscle that MRI can detect.[98]
Differential diagnosis
Included in the
Management
No pharmacologic treatment has proven to significantly slow progression of weakness or meaningfully improve strength.[100][2][10]
Screening and monitoring of complications
The
Physical and occupational therapy
Braces are often used to address muscle weakness. Scapular bracing can improve scapular positioning, which improves shoulder function, although it is often deemed as ineffective or impractical.[106] Ankle-foot orthoses can improve walking, balance, and quality of life.[107]
Pharmacologic management
No pharmaceuticals have definitively proven effective for altering the disease course.[100] Although a few pharmaceuticals have shown improved muscle mass in limited respects, they did not improve quality of life, and the AAN recommends against their use for FSHD.[100]
Reconstructive surgery
Scapular winging is amenable to surgical correction, namely operative scapular fixation. Scapular fixation is restriction and stabilization of the position of the scapula, putting it in closer apposition to the rib cage and reducing winging. Absolute restriction of scapular motion by fixation of the scapula to the ribs is most commonly reported.[108] This procedure often involves inducing bony fusion, called arthrodesis, between the scapula and ribs. Names for this include scapulothoracic fusion, scapular fusion, and scapulodesis. This procedure increases arm active range of motion, improves arm function, decreases pain, and improves cosmetic appearance.[109][110] Active range of motion of the arm increases most in the setting of severe scapular winging with an unaffected deltoid muscle;[11] however, passive range of motion decreases. In other words, the patient gains the ability to slowly raise their arms to 90+ degrees, but they lose the ability to "throw" their arm up to a full 180 degrees.[2] The AAN states that scapular fixation can be offered cautiously to select patients after balancing these benefits against the adverse consequences of surgery and prolonged immobilization.[100][10]
Another form of operative scapular fixation is scapulopexy. "Scapulo-" refers to the scapula bone, and "-pexy" is derived from the Greek root "to bind." Some versions of scapulopexy accomplish essentially the same result as scapulothoracic fusion, but instead of inducing bony fusion, the scapula is secured to the ribs with only wire, tendon grafts, or other material. Some versions of scapulopexy do not completely restrict scapular motion, examples including
Various other surgical reconstructions have been described. Upper eyelid gold implants have been used for those unable to close their eyes.[114] Drooping lower lip has been addressed with plastic surgery.[115] Ablity to smile can theoretically be restored with a tendon transfer, with donors such as a portion of the temporalis muscle, although evidence is lacking in FSHD.[116] Select cases of foot drop can be surgically corrected with tendon transfer, in which the tibialis posterior muscle is repurposed as a tibialis anterior muscle, a version of this being called the Bridle procedure.[117][118][105] Severe scoliosis caused by FSHD can be corrected with spinal fusion; however, since scoliosis might be a compensatory change in response to muscle weakness, correction of spinal alignment can result in further impaired muscle function.
- Scapular winging management
-
Kinesiology tape applied across the scapulas.
-
A cloth brace to hold the scapulas in retraction to reduce shoulder symptoms, such as collarbone pain.
-
Scapula-to-scapula scapulopexy, pre- and post-operation. The scapulas are tethered together into a retracted position with an Achilles tendon graft, which, in this case, rendered the rhomboid major muscles distinguishable.
Prognosis
Genetics partially predicts prognosis.[100] Those with large D4Z4 repeat deletions (with a remaining D4Z4 repeat array size of 10-20 kbp, or 1-4 repeats) are more likely to have severe and early disease, as well as non-muscular symptoms.[100] Those who have the genetic mutations of both FSHD1 and FSHD2 are more likely to have severe disease.[74] It has also been observed that D4Z4 shortening is less and disease manifestation is milder when a prominent family history is present, as opposed to a new mutation.[119] In some large families, 30% of those with the mutation had no noticeable symptoms, and 30% of those with symptoms did not progress beyond facial and shoulder weakness.[24] Women tend to develop symptoms later in life and have less severe disease courses.[113]
Remaining variations in disease course are attributed to unknown environmental factors. A single study found that disease course is not worsened by tobacco smoking or alcohol consumption, common risk factors for other diseases.[120]
Pregnancy
Pregnancy outcomes are overall good in mothers with FSHD; there is no difference in rate of
A single review found that weakness worsens, without recovery, in 12% of mothers with FSHD during pregnancy, although this might be due to weight gain or deconditioning.[121]
Epidemiology
The prevalence of FSHD ranges from 1 in 8,333 to 1 in 15,000.[2] The Netherlands reports a prevalence of 1 in 8,333, after accounting for the undiagnosed.[122] The prevalence in the United States is commonly quoted as 1 in 15,000.[15]
After genetic testing became possible in 1992, average prevalence was found to be around 1 in 20,000, a large increase compared to before 1992.[123][24][122] However, 1 in 20,000 is likely an underestimation, since many with FSHD have mild symptoms and are never diagnosed, or they are siblings of affected individuals and never seek definitive diagnosis.[122]
Race and ethnicity have not been shown to affect FSHD incidence or severity.[15]
Although the inheritance of FSHD shows no predilection for biological sex, the disease manifests less often in women, and even when it manifests in women, they on average are less severely affected than affected males.[15] Estrogen has been suspected to be a protective factor that accounts for this discrepancy. One study found that estrogen reduced DUX4 activity.[124] However, another study found no association between disease severity and lifetime estrogen exposure in females. The same study found that disease progression was not different through periods of hormonal changes, such as menarche, pregnancy, and menopause.[125]
History
The first description of a person with FSHD in medical literature appears in an autopsy report by
Since the publication of the unifying theory in 2010, researchers continued to refine their understanding of DUX4. With increasing confidence in this work, researchers proposed the first a consensus view in 2014 of the pathophysiology of the disease and potential approaches to therapeutic intervention based on that model.[27]
Alternate and historical names for FSHD include the following:
- facioscapulohumeral disease[23]
- faciohumeroscapular [citation needed]
- Landouzy-Dejerine disease[23] (or 'syndrome'[127] or 'type of muscular dystrophy'[23])
- Erb-Landouzy-Dejerine syndrome[citation needed]
| 1861 | Person with muscular dystrophy depicted by Duchenne. Based on the muscles involved, this person could have had FSHD. |
| 1884 | Landouzy and Dejerine describe a form of childhood progressive muscle atrophy with a characteristic involvement of facial muscles and distinct from pseudohypertrophic (Duchenne's MD) and spinal muscle atrophy in adults.[128] |
| 1886 | Landouzy and Dejerine describe progressive muscular atrophy of the scapulo-humeral type.[129] |
| 1950 | Tyler and Stephens study 1249 individuals from a single kindred with FSHD traced to a single ancestor and describe a typical Mendelian inheritance pattern with complete penetrance and highly variable expression. The term facioscapulohumeral dystrophy is introduced.[130] |
| 1982 | Padberg provides the first linkage studies to determine the genetic locus for FSHD in his seminal thesis "Facioscapulohumeral disease."[23] |
| 1987 | The complete sequence of the Dystrophin gene (Duchenne's MD) is determined.[131] |
| 1991 | The genetic defect in FSHD is linked to a region (4q35) near the tip of the long arm of chromosome 4.[132]
|
| 1992 | FSHD, in both familial and R1 fragment to < 28 kb (50–300 kb normally).[93]
|
| 1993 | 4q EcoR1 fragments are found to contain tandem arrangement of multiple 3.3-kb units (D4Z4), and FSHD is associated with the presence of < 11 D4Z4 units.[92]
A study of seven families with FSHD reveals evidence of genetic heterogeneity in FSHD.[133] |
| 1994 | The heterochromatic structure of 4q35 is recognized as a factor that may affect the expression of FSHD, possibly via position-effect variegation.[134]
DNA sequencing within D4Z4 units shows they contain an open reading frame corresponding to two homeobox domains, but investigators conclude that D4Z4 is unlikely to code for a functional transcript.[134][135] |
| 1995 | The terms FSHD1A and FSHD1B are introduced to describe 4q-linked and non-4q-linked forms of the disease.[136] |
| 1996 | FSHD Region Gene1 (FRG1) is discovered 100 kb proximal to D4Z4.[137] |
| 1998 | Monozygotic twins with vastly different clinical expression of FSHD are described.[20] |
| 1999 | Complete sequencing of 4q35 D4Z4 units reveals a promoter region located 149 bp 5' from the open reading frame for the two homeobox domains, indicating a gene that encodes a protein of 391 amino acid protein (later corrected to 424 aa[138]), given the name DUX4.[139] |
| 2001 | Investigators assessed the |
| 2002 | A polymorphic segment of 10 kb directly distal to D4Z4 is found to exist in two allelic forms, designated 4qA and 4qB. FSHD1 is associated solely with the 4qA allele.[141]
Three genes (FRG1, FRG2, ANT1) located in the region just centromeric to D4Z4 on chromosome 4 are found in isolated muscle cells from individuals with FSHD at levels 10 to 60 times greater than normal, showing a linkage between D4Z4 contractions and altered expression of 4q35 genes.[142] |
| 2003 | A further examination of DNA methylation in different 4q35 D4Z4 restriction fragments (BsaAI and FseI) showed significant hypomethylation at both sites for individuals with FSHD1, non-FSHD-expressing gene carriers, and individuals with phenotypic FSHD relative to unaffected controls.[143] |
| 2004 | Contraction of the D4Z4 region on the 4qB allele to < 38 kb does not cause FSHD.[144] |
| 2006 | Transgenic mice overexpressing FRG1 are shown to develop severe myopathy.[145] |
| 2007 | The DUX4 open reading frame is found to have been conserved in the genome of primates for over 100 million years, supporting the likelihood that it encodes a required protein.[146]
Researchers identify DUX4 mRNA in primary FSHD myoblasts and identify in D4Z4-transfected cells a DUX4 protein, the overexpression of which induces cell death.[138]
DUX4 mRNA and protein expression are reported to increase in myoblasts from FSHD patients, compared to unaffected controls. Stable DUX4 mRNA is transcribed only from the most distal D4Z4 unit, which uses an intron and a polyadenylation signal provided by the flanking pLAM region. DUX4 protein is identified as a transcription factor, and evidence suggests overexpression of DUX4 is linked to an increase in the target paired-like homeodomain transcription factor 1 (PITX1).[147] |
| 2009 | The terms FSHD1 and FSHD2 are introduced to describe D4Z4-deletion-linked and non-D4Z4-deletion-linked genetic forms, respectively. In FSHD1, hypomethylation is restricted to the short 4q allele, whereas FSHD2 is characterized by hypomethylation of both 4q and both 10q alleles.[148]
Splicing and cleavage of the terminal (most noncoding RNAs, antisense RNAs and capped mRNAs as new candidates for the pathophysiology of FSHD.[149]
Mechanism proposed of DBE-T (D4Z4 Regulatory Element transcript) leading to de-repression of 4q35 genes.[62] |
| 2010 | A unifying genetic model of FSHD is established: D4Z4 contractions only cause FSHD when in the context of a 4qA allele due to stabilization of DUX4 RNA transcript, allowing DUX4 expression.[8] Several organizations including The New York Times highlighted this research[150][151]
Human Genome with the National Institutes of Health stated:[150]
Daniel Perez, co-founder of the FSHD Society, hailed the new findings saying:[151]
The MDA stated that:[citation needed]
One of the report's co-authors, Silvère van der Maarel of the University of Leiden, stated that[citation needed]
DUX4 is found actively transcribed in skeletal muscle biopsies and primary myoblasts. FSHD-affected cells produce a full-length transcript, DUX4-fl, whereas alternative splicing in unaffected individuals results in the production of a shorter, 3'-truncated transcript (DUX4-s). The low overall expression of both transcripts in muscle is attributed to relatively high expression in a small number of nuclei (~ 1 in 1000). Higher levels of DUX4 expression in human testis (~100 fold higher than skeletal muscle) suggest a developmental role for DUX4 in human development. Higher levels of DUX4-s (vs DUX4-fl) are shown to correlate with a greater degree of DUX-4 H3K9me3-methylation.[7] |
| 2012 | Some instances of FSHD2 are linked to mutations in the SMCHD1 gene on chromosome 18, and a genetic/mechanistic intersection of FSHD1 and FSHD2 is established.[68]
The prevalence of FSHD-like D4Z4 deletions on permissive alleles is significantly higher than the prevalence of FSHD in the general population, challenging the criteria for molecular diagnosis of FSHD.[152] When expressed in primary myoblasts, DUX4-fl acted as a transcriptional activator, producing a > 3-fold change in the expression of 710 genes.[153] A subsequent study using a larger number of samples identified DUX4-fl expression in myogenic cells and muscle tissue from unaffected relatives of FSHD patients, per se, is not sufficient to cause pathology, and that additional modifiers are determinants of disease progression.[154] |
| 2013 | Mutations in SMCHD1 are shown to increase the severity of FSHD1.[74]
epigenetic features of FSHD.[155]
|
| 2014 | DUX4-fl and downstream target genes are expressed in skeletal muscle biopsies and biopsy-derived cells of fetuses with FSHD-like D4Z4 arrays, indicating that molecular markers of FSHD are already expressed during fetal development.[156]
Researchers "review how the contributions from many labs over many years led to an understanding of a fundamentally new mechanism of human disease" and articulate how the unifying genetic model and subsequent research represent a "pivot-point in FSHD research, transitioning the field from discovery-oriented studies to translational studies aimed at developing therapies based on a sound model of disease pathophysiology." They describe the consensus mechanism of pathophysiology for FSHD as an "inefficient repeat-mediated epigenetic repression of the D4Z4 macrosatellite repeat array on chromosome 4, resulting in the variegated expression of the DUX4 retrogene, encoding a double-homeobox transcription factor, in skeletal muscle."[27] |
| 2020 | Voice of the Patient Report released documenting FSHD's impacts on daily life as conveyed by about 400 patients during an FDA externally led Patient-Focused Drug Development meeting, which was held on June 29, 2020.[32][30][31][33] |
Past pharmaceutical development
Early drug trials, before the pathogenesis involving DUX4 was discovered, were untargeted and largely unsuccessful.[19] Compounds were trialed with goals of increasing muscle mass, decreasing inflammation, or addressing provisional theories of disease mechanism.[19] The following drugs failed to show efficacy:
- Prednisone, a steroid, based on its antiinflammatory properties and therapeutic effect in Duchenne muscular dystrophy.[157]
- Oral albuterol, a β2 agonist, on the basis of its anabolic properties. Although it improved muscle mass and certain measures of strength in those with FSHD, it did not improve global strength or function.[158][159][160] Interestingly, β2 agonists were later shown to reduce DUX4 expression.[161]
- Diltiazem, a calcium channel blocker, on the bases of anecdotal reports of benefit and the theory that calcium dysregulation played a part in muscle cell death.[162]
- MYO-029 (Stamulumab), an antibody that inhibits myostatin, was developed to promote muscle growth. Myostatin is a protein that inhibits the growth of muscle tissue.[163]
- ACE-083, a TGF-β inhibitor, was developed to promote muscle growth.[164]
Society and culture
Media
- In the Amazon Video series The Man in the High Castle, Obergruppenführer John Smith's son, Thomas, is diagnosed with Landouzy-Dejerine syndrome.[165]
- In the biography Stuart: A Life Backwards, the protagonist was affected by muscular dystrophy,[166] presumably FSHD.[citation needed]
- Good Bad Things, an independent film about an entrepreneur afflicted with FSHD and his journey of transformation, self-acceptance and discovery. The movie premiered at the 2024 Slamdance Film Festival[167][168]
- International Day of Persons with Disabilities in 2023.[169]
Patient and research organizations
- The FSHD Society (named "FSH Society" until 2019)MD-CARE Act of 2001, which provided federal funding for all muscular dystrophies.[171][172] The FSHD Society has grown into the world's largest grassroots organization advocating for patient education and scientific and medical research for FSHD.[173][174] One notable spokesperson for FSHD Society has been Max Adler, an actor on the TV series Glee.[175]
- Friends of FSH Research is a research-oriented nonprofit organization founded in 2004 by Terry and Rick Colella from Kirkland, Washington after their son was diagnosed with FSHD.[176][177][178][179]
- The FSHD Global Research Foundation was founded in 2007 by Bill Moss in Australia, a former
- FSHD EUROPE was founded in 2010.[183] Spanning multiple countries in Europe, it has launched the European Trial Network.[183]
Notable cases
- Lululemon. He has pledged 100 million Canadian dollars to research through the venture 'Solve FSHD'.[184]
- Chris Carrino is the radio voice of the Brooklyn Nets. He founded the 'Chris Carrino Foundation for FSHD', oriented towards research funding.[185]
- Madison Ferris is an American actress with FSHD who was the first wheelchair user to play a lead on Broadway.[186][187]
- Morgan Hoffmann is an American professional golfer. He started the Morgan Hoffmann Foundation, oriented towards research funding.[188]
- Arnold Gold (1925-2024) was a pediatric neurologist, founder of the Arnold P. Gold Foundation, and creator of white coat ceremonies. Gold focused on patient-centered care and humanism.[189]
Research directions
Pharmaceutical development
After achieving consensus on FSHD pathophysiology in 2014, researchers proposed four approaches for therapeutic intervention:[27]
- enhance the epigenetic repression of the D4Z4
- target the DUX4 mRNA, including altering splicing or polyadenylation;
- block the activity of the DUX4 protein
- inhibit the DUX4-induced process, or processes, that leads to pathology.
Small molecule drugs
Most drugs used in medicine are "small molecule drugs," as opposed to biologic medical products that include proteins, vaccines, and nucleic acids. Small molecule drugs can typically be taken by ingestion, rather than injection.
- Losmapimod, a selective inhibitor of p38α/β mitogen-activated protein kinases, was identified by Fulcrum Therapeutics as a potent suppressor of DUX4 in vitro.[191] Results of a phase IIb clinical trial, revealed in June 2021, showed statistically significant slowing of muscle function deterioration. Further trials are pending.[192][193]
- Casein kinase 1 (CK1) inhibition has been identified by Facio Therapies, a Dutch pharmaceutical company, to repress DUX4 expression and is in preclinical development. Facio Therapies claims that CK1 inhibition leaves myotube fusion intact, unlike BET inhibitors, p38 MAPK inhibitors, and β2 agonists.[194][195]
Gene therapy
Gene therapy is the administration of nucleotides to treat disease. Multiple types of gene therapy are in the preclinical stage of development for the treatment of FSHD.
- Antisense therapy utilizes antisense oligonucleotides that bind to DUX4 messenger RNA, inducing its degradation and preventing DUX4 protein production. Phosphorodiamidate morpholinos, an oligonucleotide modified to increase its stability, have been shown to selectively reduce DUX4 and its effects; however, these antisense nucleotides have poor ability to penetrate muscle.[2]
- viral vectors, have shown to reduce DUX4, protect against muscle pathology, and prevent loss of grip strength in mouse FSHD models.[2] Arrowhead pharmaceuticals is developing an RNA interference therapeutic against DUX4, named ARO-DUX4, and intends to file for regulatory clearance in third quarter of 2021 to begin clinical trials.[196][197][198]
- Genome editing, the permanent alteration of genetic code, is being researched. One study tried to use CRISPR-Cas9 to knockout the polyadenylation signal in lab dish models, but was unable to show therapeutic results.[199]
Potential drug targets
- Inhibition of the hyaluronic acid (HA) pathway is a potential therapy. One study found that many DUX4-induced molecular pathologies are mediated by HA signaling, and inhibition of HA biosynthesis with 4-methylumbelliferone prevented these molecular pathologies.[200]
- P300 inhibition has shown to inhibit the deleterious effects of DUX4[201]
- BET inhibitors have been shown to reduce DUX4 expression.[161]
- Antioxidants could potentially reduce the effects of FSHD. One study found that vitamin C, vitamin E, zinc gluconate, and selenomethionine supplementation increased endurance and strength of the quadriceps, but had no significant benefit on walking performance.[202] Further study is warranted.[2]
Outcome measures
Ways of measuring the disease are important for studying disease progression and assessing the efficacy of drugs in clinical trials.
- Reachable workspace uses the Kinect motion sensing system to compare range of reach before and after a therapeutic clinical trial.[203]
- Quality of life can be measured with questionnaires, such as the FSHD Health Index.[204][2]
- How the disease affects daily activities can measured with questionnaires, such as the FSHD‐Rasch‐built overall disability scale (FSHD-RODS)[205] or FSHD composite outcome measure (FSHD-COM).[206]
- Electrical impedance myography is being studied as a way to measure muscle damage.[2]
- Muscle MRI is useful for assessment of all the muscles in the body. Muscles can be scored based on the degree of fat infiltration.[2]
References
- ^
The sources listed below differ on pronunciation of the 'u' in 'scapulo'. A 'long u' sound in an unstressed nonfinal syllable is often reduced to a schwa and varies by speaker.
- "Facioscapulohumeral". Merriam-Webster.com Dictionary.
- "Facioscapulohumeral". Medical Dictionary, Farlex and Partners, 2009.
- ^ S2CID 208531681.
- ISBN 0-13-948142-7.
- ^ S2CID 4481678.
- ^ ISBN 978-0-323-35317-5.
- PMID 28459456.
- ^ PMID 21060811.
- ^ PMID 20724583. Archived from the original(PDF) on 2014-06-05.
- ^ PMID 17924332.
- ^ S2CID 254883066.
- ^ PMID 32430271.
- S2CID 2426923.
- S2CID 24936950.
- ^ S2CID 43304086.
- ^ PMID 27922500.
- ^ a b Cruveilhiers J (1852–1853). "Mémoire sur la paralysie musculaire atrophique". Bulletins de l'Académie de Médecine. 18: 490–502, 546–583.
- ^ ISBN 1-85996-244-0.
- ^ a b Landouzy L, Dejerine J (1885). Landouzy L, Lépine R (eds.). "De la myopathie atrophique progressive (myopathie sans neuropathie débutant d'ordinaire dans l'enfance par la face)". Revue de Médecine (in French). 5. Felix Alcan: 253–366. Retrieved 19 May 2020.
- ^ PMID 33092966.
- ^ PMID 9733041.
- S2CID 44422140.
- ^ Pandya S, Eichinger K. "Physical Therapy for Facioscapulohumeral Muscular Dystrophy" (PDF). FSHD Society. Archived from the original (PDF) on 14 April 2020. Retrieved 14 April 2020.
- ^ a b c d e Padberg GW (1982-10-13). Facioscapulohumeral disease (Thesis). Leiden University.
- ^ ISBN 1-85996-244-0.
- ^ S2CID 101093.
- S2CID 4237308.
- ^ PMID 24940479.
- S2CID 238246093.
- ^ ISBN 0-203-48367-7.
- ^ a b The FDA held an externally-led Patient-Focused Drug Development meeting with about 400 FSHD patients on June 29, 2020, resulting in a seminal document called the "Voice of the Patient Report." The report captures the impact of FSHD on the daily lives of those with the disease as conveyed by the patients themselves. While FSHD is often perceived to be "mild," the report shows that over 80% of patients report being "moderately" or "severely" limited in daily activities.
- Society F. "FSHD Society releases Voice of the Patient Report on FSH muscular dystrophy". www.prweb.com. Retrieved 2024-01-31.
- ^ a b Society F. "Facioscapulohumeral muscular dystrophy community speaks to the FDA". www.prweb.com. Retrieved 2024-01-31.
- ^ a b Voice of the Patient Forum - Patient-Focused Drug Development Meeting, retrieved 2024-01-31
- ^ a b Overman D (2020-11-13). "People Living with FSHD Tell Their Stories in New Report". Rehab Management. Retrieved 2024-01-31.
- ^ PMID 30804066.
- S2CID 7695047.
- ^ a b "A giant of FSHD research shares his "regrets"". FSHD Society. Way Back Machine. 30 September 2020. Archived from the original on 24 October 2020. Retrieved 11 March 2021.
Another striking aspect of FSHD is that muscles weakness seems to vary so much from patient to patient. Nonetheless, "there is a highly characteristic pattern of muscle weakness, otherwise we would never have been able to recognize FSHD as a specific disease," Padberg said. "Strong deltoid muscle does not occur in any other condition that involves weakness of scapular stabilizers. No other muscle disease with shoulder girdle involvement has this pattern." Unfortunately, "an explanation is beyond our grasp as we don't know how muscle are laid down" during the early stages of human gestation.
- ^ PMID 24932477.
- ^ S2CID 24650482.
- PMID 34977539.
- PMID 17986494.
- ISBN 978-0-12-417044-5.
- ^ PMID 32954265.
- S2CID 27523889.
- S2CID 204996841.
- S2CID 26276887.
- ^ PMID 32080072.
- ISBN 978-3-319-17361-0.
- S2CID 31335126.
- S2CID 235822532.
- ^ PMID 35158020.
- ^ S2CID 39898514.
- ^
The name "D4Z4" is derived from an obsolete nomenclature system used for DNA segments of unknown significance during the human genome project: D for DNA, 4 for chromosome 4, Z indicates it is a repetitive sequence, and 4 is a serial number assigned based on the order of submission.
- White J, McAlpine P, Antonarakis S, Cann H, Eppig J, Frazer K, Frezal J, Lancet D, Nahmias J, Pearson P, Peters J, Scott A, Scott H, Spurr N, Talbot C, Povey S (October 1997). "NOMENCLATURE". Genomics. 45 (2): 468–471. PMID 9344684.
- Fasman KH, Letovsky SI, Cottingham RW, Kingsbury DT (1 January 1996). "Improvements to the GDB Human Genome Data Base". Nucleic Acids Research. 24 (1): 57–63. PMID 8594601.
- White J, McAlpine P, Antonarakis S, Cann H, Eppig J, Frazer K, Frezal J, Lancet D, Nahmias J, Pearson P, Peters J, Scott A, Scott H, Spurr N, Talbot C, Povey S (October 1997). "NOMENCLATURE". Genomics. 45 (2): 468–471.
- ^ a b c d Impossible Things: Through the looking glass with FSH Dystrophy Researchers, Margaret Wahl, MDA, Quest magazine, Vol 14, No 2, March–April 2007
- PMID 17984056.
- ^ PMID 37380887.
- ISBN 1-85996-244-0.
- PMID 17335567.
- S2CID 231589589.
- ^ PMID 29162933.
- PMID 32731450.
- S2CID 131775712.
- ^ PMID 22541069.
- ^ PMID 30979860.
- PMID 8733044.
- S2CID 84518968.
- PMID 30871534.
- PMID 24882751.
- ^ PMID 23143600.
- PMID 27153398.
- ^ S2CID 111390628.
- ^ S2CID 218982743.
- PMID 23785127.
- ^ PMID 36078093.
- ^ PMID 24075187.
- ^ PMID 31979100.
- ^ PMID 32250341.
- PMID 34943834.
- ^ S2CID 232202360.
- PMID 32213627.
- S2CID 239471655.
- PMID 30312408.
- ISBN 978-0-19-067501-1.
- PMID 22892954.
- ^ S2CID 25005883.
- ^ S2CID 19421344.
- S2CID 25693278.
- PMID 31600781.
- S2CID 85495566.
- ^ Kinoshita J (11 March 2020). "Genetic testing for FSHD—a new frontier". FSHD Society. Archived from the original on 8 April 2020. Retrieved 8 April 2020.
- S2CID 6871094.
- ^ PMID 34441403.
- ^ PMID 8111371.
- ^ S2CID 21940164.
- ISBN 1-85996-244-0.
- PMID 34559225.
- S2CID 10002229.
- ^ FSHD Fact Sheet Archived 2006-03-06 at the Wayback Machine, MDA, 11/1/2001
- ^ PMID 20422195.
- ^ )
- ^ PMID 26215877.
- ^ S2CID 18448196.
- ^ S2CID 25382403.
- ^ S2CID 11617226.
- PMID 31808555.
- ^ PMID 27185458.
- ^ "Information for Patients and Families - The Richard Fields Center for FSH Dystrophy (FSHD) & Neuromuscular Research - University of Rochester Medical Center". www.urmc.rochester.edu. Archived from the original on 14 November 2019. Retrieved 14 April 2020.
- PMID 23138679.
- ^ PMID 20091543.
- PMID 19333668.
- S2CID 27456684.
- S2CID 20162712.
- ISBN 978-1-9751-2347-5.
- ^ ISBN 1-85996-244-0.
- S2CID 16251273.
- S2CID 16343571.
- .
- PMID 31456618.
- ISBN 978-1-4557-0924-3. Retrieved 1 January 2020.
- ^ Lunt P, Upadhyaya M, Koch MC (2004). "Genotype-phenotype relationships in FSHD". In Upadhyaya M, Cooper DN (eds.). FSHD Facioscapulohumeral Muscular Dystrophy: Clinical Medidne and Molecular Cell Biology. BIOS Scientific Publishers Limited. p. 157.
- PMID 34407911.
- ^ S2CID 246651681.
- ^ PMID 25122204.
- PMID 28198707.
- PMID 28263188.
- PMID 29655530.
- ^ Duchenne GB (1868). "De la paralysie musculaire pseudo-hypertrophique, ou paralysie myo-sclérosique". Arch. Gen. Med. (in French). 11. Bibliothèque nationale de France: 5–25, 179–209, 305–321, 421–443, 552–588. Retrieved 18 May 2020.
- ^ a b Landouzy-Dejerine syndrome, whonamedit.com, date accessed March 11, 2007
- ^ Landouzy, Dejerine (1884). "De la myopathie atrophique progressive (myopathie héréditaire, débutant dans l'enfance par la face, sans altération du système nerveux)". Comptes Rendus de l'Académie des Sciences. 98: 53–55.
- ^ Landouzy, Dejerine (1886). "Contribution à l'étude de la myopathie atrophique progressive (myopathie atrophique progressive, à type scapulo-huméral)". Comptes Rendus des Séances de la Société de Biologie. 38: 478–481.
- PMID 15411118.
- S2CID 35668717.
- PMID 2037288.
- PMID 8328457.
- ^ S2CID 6933736.
- PMID 7987304.
- PMID 8558552.
- PMID 8733123.
- ^ S2CID 25926418.
- PMID 10433963.
- PMID 11708861.
- S2CID 28107557.
- S2CID 16396883.
- S2CID 28696708.
- PMID 15467981.
- S2CID 4427465.
- PMID 17668377.
- PMID 17984056.
- S2CID 14517505.
- PMID 19359275.
- ^ a b Kolata G (19 August 2010). "Reanimated 'Junk' DNA Is Found to Cause Disease". The New York Times. Retrieved 29 August 2010.
- ^ a b "Research Milestones Achieved by FSH Society Research". FSH Society. Archived from the original on 2010-08-23. Retrieved 2024-02-21.
- PMID 22482803.
- PMID 22209328.
- PMID 22798623.
- PMID 23593020.
- PMID 23966205.
- S2CID 729275.
- S2CID 24848310.
- S2CID 28093111.
- S2CID 22778327.
- ^ PMID 28870238.
- S2CID 361422.
- ^ Wyeth Initiates Clinical Trial with Investigational Muscular Dystrophy Therapy MYO-029
- ^ Malcolm E (18 June 2019). "ACE-083". Muscular Dystrophy News. Retrieved 19 December 2019.
- ^ Vultaggio M (5 October 2018). "Why Rufus Sewell wanted to play 'Man in the High Castle' villain John Smith". Newsweek. Archived from the original on 6 November 2018. Retrieved 12 April 2022.
- ^ Kakutani M (9 June 2006). "'Stuart: A Life Backwards,' by Alexander Masters, a Portrait of a Homeless Man". The New York Times. Archived from the original on 16 January 2018.
- ^ White A (2023-12-19). "'Ramy' Star Steve Way Boards Indie Drama 'Good Bad Things' as Executive Producer (Exclusive)". The Hollywood Reporter. Retrieved 2024-01-31.
- ^ jkinoshita (2022-08-25). "New movie will feature man with FSHD". FSHD Society. Retrieved 2024-01-31.
- ^ "A disability advocate preserves his voice with iPhone". Apple Newsroom. Retrieved 2024-02-21.
- ^ a b Kinoshita J (16 August 2019). "What's in a name? – FSHD Society". FSHD Society. Archived from the original on 12 April 2022. Retrieved 18 August 2019.
- ^ a b "Our History". FSHD Society. Archived from the original on 27 February 2022.
- ^ a b Bartlett J (19 August 2014). Boston Business Journal https://web.archive.org/web/20220412220102/https://www.bizjournals.com/boston/blog/health-care/2014/08/dan-perez-living-with-and-fighting-against-a.html. Archived from the original on 12 April 2022. Retrieved 12 April 2022.
{{cite news}}: Missing or empty|title=(help) - ^ "FSHD Society". NORD (National Organization for Rare Disorders). Archived from the original on 2022-05-13. Retrieved 2022-04-12.
- ^ "FSHD Society Achieves Accreditation from BBB Wise Giving Alliance". Prweb. 26 April 2022. Archived from the original on 29 April 2022. Retrieved 29 April 2022.
- ^ "This Is FSHD". HuffPost. 16 July 2014. Archived from the original on 2 August 2019. Retrieved 12 April 2022.
- ^ Krummey C (30 March 2017). "Kirkland couple raises $3.2 million for FSH muscular dystrophy research". Kirkland Reporter. Archived from the original on 16 June 2017. Retrieved 9 April 2022.
- ^ "About Us: Friends of FSH Research". Friends of FSH Research. Archived from the original on 17 February 2020. Retrieved 9 April 2022.
- ^ AMRA Medical (13 Oct 2021). "AMRA Medical's Whole-body MRI Analysis Used in FSHD Clinical Trial Research Network Study for Biomarker Development". Cision PR Newswire. Archived from the original on 1 November 2021. Retrieved 9 April 2022.
- ^ Avidity Biosciences, Inc. (16 August 2021). "Avidity Biosciences Enters Into Collaboration with FSHD Clinical Trial Network to Support Development of Biomarkers for Future Clinical Trial Use". Cision PR Newswire. Archived from the original on 16 August 2021.
- ^ Overington C (24 September 2016). "He's physically wasting but his brain is sharp. Former Macquarie banker Bill Moss is back in business". The Australian.
- ^ a b c Chancellor J (7 September 2020). "Buyer swoops on Brett Whiteley's corella". The Australian. Retrieved 9 April 2022.
- ^ a b Tasker SJ (26 May 2018). "Bill Moss, the single-minded biotech and a search for a cure". The Australian. Retrieved 9 April 2022.
- ^ from the original on Mar 19, 2024.
- ^ Judd A (8 March 2022). "Lululemon founder Chip Wilson donates $100M to find cure for his illness, 30 years after diagnosis". Global News. Retrieved 9 April 2022.
- ^ Isola F (23 April 2019). "'You're not going to quit': One step at a time, Nets radio voice Chris Carrino continues to walk tall". The Athletic. Archived from the original on 14 Feb 2023. Retrieved 9 April 2022.
- ^ "Actress Breaking Barriers as Broadway's First Lead Actor in Wheelchair". NBC News. March 19, 2024. Retrieved 2024-02-21.
- ^ "Community Profiles: Actress Madison Ferris". FSHD Straight Talk with Tim Hollenback. Audioboom. Sep 13, 2022. Archived from the original on 2024-02-21. Retrieved 2024-02-21.
- ^ Shedloski D (24 February 2020). "There's no stopping Morgan Hoffmann in his fight against muscular dystrophy". Golf Digest. Archived from the original on 5 March 2022. Retrieved 12 April 2022.
- ISSN 0362-4331. Retrieved 2024-02-21.
- PMID 26246499.
- ^ "Fulcrum Therapeutics Acquires Global Rights to Losmapimod, a Potential Disease-Modifying Therapy for Facioscapulohumeral Muscular Dystrophy". BioSpace. Retrieved 12 August 2019.
- ^ "ReDUX4 trial result exceeds expectations". FSHD Society. Wayback Machine. 2021-06-24. Archived from the original on 26 June 2021. Retrieved 26 June 2021.
- ^ "Efficacy and Safety of Losmapimod in Subjects With Facioscapulohumeral Muscular Dystrophy (FSHD)". ClinicalTrials.gov. United States National Library of Medicine. Retrieved 12 August 2019.
- ^ "Facio to present at the World Muscle Society Congress". Facio Therapies. 30 September 2019. Retrieved 9 November 2019.
- ^ "Facio reveals novel mechanism targeting the cause of FSHD". Facio Therapies. 24 June 2019. Retrieved 9 November 2019.
- ^ "Arrowhead Pharmaceuticals announces FSHD drug candidate". FSHD Society. 15 April 2021. Retrieved 15 April 2021.
- ^ "Arrowhead Announces ARO-DUX4 as First Muscle Targeted RNAi Candidate Using TRiMTM Platform". Businesswire. 15 April 2021. Retrieved 15 April 2021.
- PMID 34880230.
- PMID 33374516.
- PMID 31844661.
- PMID 31535023.
- S2CID 10971952.
- PMID 24828906.
- S2CID 25834947.
- PMID 33838063.
- PMID 29381807.
External links
- World FSHD Alliance: FSHD patient advocacy organizations across the world
- list of clinical trials for FSHD, Clinicaltrials.gov.
- fsh at NIH/UW GeneTests