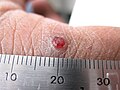
Pyogenic granuloma
| Pyogenic granuloma | |
|---|---|
| Other names | Eruptive hemangioma, granulation tissue-type hemangioma, granuloma gravidarum, lobular capillary hemangioma, pyogenic fibroma, pregnancy tumor, and tumor of pregnancy[1][2] |
 | |
| Specialty | Dermatology |
A pyogenic granuloma or lobular capillary hemangioma
Pyogenic granulomas may be seen at any age, and are more common in
Signs and symptoms
The appearance of pyogenic granuloma is usually a color ranging from red/pink to purple, grows rapidly, and can be smooth or mushroom-shaped. Younger lesions are more likely to be red because of their high number of blood vessels. Older lesions begin to change into a pink color. Size commonly ranges from a few millimeters to centimeters, though smaller or larger lesions may occur.[medical citation needed] A pyogenic granuloma can be painful, especially if located in an area of the body where it is constantly disturbed. Pyogenic granulomas can grow rapidly and often bleed profusely with little or no trauma. They may exude an oil-like substance, causing the surface to be damp. This is especially true if the granuloma is located on the scalp.[medical citation needed]
One study has suggested a correlation between pyogenic granulomas and
Associated conditions
Due to its overwhelming incidence on the gingiva, the condition is often associated with two other diseases, though not because they occur together. Instead, the three are associated with each other because they appear frequently on gingiva—
Cause
Pyogenic granulomas are caused by proliferation of
Diagnosis

A doctor likely can diagnose a pyogenic granuloma based on its appearance, and might perform a biopsy to make a more accurate diagnosis. A biopsy also helps rule out malignant (cancerous) medical conditions that can cause a similar kind of growth. These conditions include squamous-cell carcinoma, basal-cell carcinoma, and melanoma.[citation needed]
Histopathological examination shows multiple capillaries (due to the vascular nature of the tumor), neutrophils (pyogenic), and necrotic tissue.[citation needed]
Management
Although pyogenic granulomas are not infectious or cancerous, treatment may be considered because of bleeding or ulceration. Frequently, they are treated with
Several reports have demonstrated the efficacy of topical application of the
Usually, no treatment is used if the pyogenic granuloma occurs during pregnancy, since the lesion may heal spontaneously. Recurrent bleeding in either oral or nasal lesions may necessitate excision and cauterization sooner, however. If aesthetics are a concern, then treatment may be prioritized. Usually, only minor surgery may be needed, along with a dental cleaning for oral lesions to remove any calculus or other source of irritation.
History
Pyogenic granulomas were first described in 1897 by two French surgeons, Antonin Poncet and Dor, who named these lesions botryomycosis hominis.[14]
Terminology
The name "pyogenic granuloma" is misleading, as it is neither pyogenic or a true
See also
- List of cutaneous conditions
- Trumpeter's wart
References
- ISBN 978-0-7216-2921-6.
- ISBN 978-1-4160-2999-1.
- ^ Nat Pernick. "Oral cavity & oropharynx - Other nonneoplastic - Pyogenic granuloma". PathologyOutlines. Topic Completed: 1 November 2013. Minor changes: 12 October 2020
- ISBN 0-07-138076-0.
- ^ PMID 17220613.
- PMID 18377654.
- PMID 26798522.
- S2CID 7408146.
- PMID 16310070.
- PMID 18496485.
- S2CID 8958995.
- PMID 9041290.
- S2CID 38987169.
- ISSN 0003-9950.