Campylobacter
| Campylobacter | |
|---|---|
| |
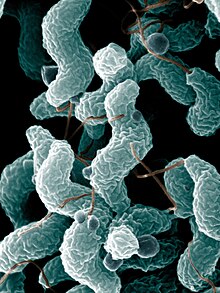
| Campylobacter jejuni | |
| Scientific classification | |
| Domain: | Bacteria |
| Phylum: | Campylobacterota |
| Class: | "Campylobacteria"
|
| Order: | Campylobacterales |
| Family: | Campylobacteraceae
|
| Genus: | Campylobacter Sebald & Véron 1963 |
| Type species | |
| Campylobacter fetus (Smith & Taylor 1919) Sebald & Veron 1963
| |
| Species | |
|
See text | |
Campylobacter is a type of bacteria that can cause a diarrheal disease in people.[1] Its name means "curved bacteria", as the germ typically appears in a comma or "s" shape. According to its scientific classification, it is a genus of gram-negative bacteria that is motile.[a][2]
The germ is common in nature and in domestic animals. It is frequently found in raw food of vegetable and animal origin. Its numbers can be very high in some foods, like raw poultry.[3] Due to their diverse natural reservoir, some Campylobacter can also be detected in the air, although not at an epidemiologically significant level.[4] The disease that some of the species of the bacteria can cause is called campylobacteriosis.[b]
At least a dozen species of Campylobacter have been implicated in human disease, with
Morphology and phenotype
Campylobacter
History
Theodor Escherich was the first to describe in 1886 what are known today as Campylobacters in the stool samples of infants, who perished from a disease he named "cholera infantum".[13] In the following years until the end of the century, a number of publications appeared, describing the occurrence of such "spirilla" in cases of "cholera-like" and "dysenteric" disease. These organisms were mainly found in the colon or associated with mucus in diarrhoeal stool specimens. Vibrio-like bacteria were also described by Sir John McFadyean and Stockman in 1913 in fetal tissues of aborted sheep.[14] For several years Campylobacters were continuously referred to as ‘‘Vibrio-like organisms’’, until 1963 when Sebald and Veron gave the name "Campylobacter" to the genus based on their shape and microaerophilic growth requirement and after showing significant biological differences with Vibrio species.[13]
Genomics
The genomes of several Campylobacter species have been sequenced, beginning with C. jejuni in 2000.[15][16] These genome studies have identified molecular markers specific to members of Campylobacter.[citation needed] Campylobacter ssp. genomes are rather small compared to those of other gastrointestinal pathogens, with sizes ranging between 1.60 and 1.90 Mbp.[16] A characteristic of most Campylobacter genomes is the presence of hypervariable regions, which can differ greatly between different strains.[16]
Studies have investigated the genes responsible for motility in Campylobacter species. Some Campylobacter species contain two
Phylogeny
The currently accepted taxonomy is based on the List of Prokaryotic names with Standing in Nomenclature (LPSN)[19] and National Center for Biotechnology Information (NCBI)[20]
| 16S rRNA based | 120 single copy marker proteins based GTDB 08-RS214[24][25][26] | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
|
Species incertae sedis:
- "C. faecalis" Kachler et al. 2000
- "C. lawrenceae" Foley et al. 2004
- C. magnus Gruntar et al. 2023
Campylobacter-specific bacteriophages
Campylobacter-specific
Pathogenesis
Campylobacter can cause a gastrointestinal infection, campylobacteriosis. The incubation period is 24–72 hours after infection.
In humans, the sites of tissue injury include the
Campylobacter has also been associated with
Detection
Campylobacter testing needs to be done to manage the risk of foodborne Campylobacter and reducing the level of foodborne Campoboteriosis, to protect people and to determine if a person is infected with Campylobacter.[citation needed]
In humans
Usually, detection of Campylobacter in humans is done by laboratory culturing a stool sample or swab of the rectum collected by a healthcare provider. Results take about 48–72 hours for preliminary results. Confirmation test and testing to determine the species of Campylobacter or drug sensitivities of the organism require additional time.[36]
In livestock
Usually, detection of Campylobacter in livestock is done by laboratory culturing a faecal sample. Results take about 48–72 hours.[37]
In meat
Usually, detection of Campylobacter in meat is done by laboratory culturing a homogenised sample. Results takes about 48–72 hours.[37]
Treatment
The infection is usually self-limiting and, in most cases, symptomatic treatment by liquid and electrolyte replacement is sufficient to treat human infections. Symptoms typically last 5–7 days.[31] Treatment with antibiotics has only a minor effect on the typical duration of the infection in non-complex cases, and is discouraged except in high-risk patients.[38] Diagnosis of campylobacteriosis is made by testing a fecal specimen. Standard treatment in high-risk cases is
Epidemiology
Canada
FoodNet Canada has reported that Campylobacter was the most common pathogen found on packaged chicken breast, with nearly half of all samples testing positive. Additionally, Campylobacter and Salmonella were the most common causes of gastrointestinal illness in Canada.[43]
Italy
In Italy, the annual prevalence of Campylobacter infections appears to be relatively stable based on findings from a national survey conducted on more than 5000 isolates. The survey revealed that the most common species of Campylobacter were C. jejuni, accounting for 83.7% of isolates, followed by C. coli (13.5%) and C. fetus (0.6%). The mean age of affected patients was 34.61 years, with males constituting 57.1% of cases. Outpatients represented the majority of cases, comprising 54% of the total. Campylobacter infections were predominantly isolated from feces, accounting for 97.3% of cases, while a smaller proportion (2.7%) was isolated from blood. Notably, C. fetus was primarily isolated from blood samples, constituting 88.2% of cases. Regarding antibiotic resistance patterns, the survey found that resistance to ciprofloxacin and tetracyclines was relatively high, with rates of 75.5% and 54.8%, respectively. In contrast, resistance to macrolides, including erythromycin, clarithromycin, and azithromycin, was lower, with rates ranging from 2% to 4.8%. Additionally, approximately 50% of C. jejuni and C. coli isolates exhibited resistance to two or more antibiotics. There was a significant decrease in resistance to ciprofloxacin and tetracyclines over time, while resistance to macrolides remained stable.[44]
New Zealand
In August 2016, an estimated 8,000+ residents of Havelock North, a town with around 13,000 residents, had gastric illness after the water supply was thought to be contaminated by Campylobacter.[45][46][47]
Norway
In June 2019, an estimated 2,000 residents of Askøy municipality got sick due to the presence of C. jejuni in the water supply. Two deaths were connected to the outbreak, and it was the largest outbreak of Campylobacter in Norway.[48] The suspected source of the contamination was thought to be horse faeces, which leaked into a drinking water pool.[49] A C. jejuni water isolate thought to be the cause of the outbreak was examined with human isolates, and showed the highest pathogenic potential in vitro, transcriptomic and genomic investigations. This could suggest why the isolate was able to cause an outbreak.[50]
Sweden
During the period of August 2016 to June 2017 there was a large outbreak of C. jejuni in Sweden. It was the largest outbreak that has been reported so far. 5000 more cases than would be expected during this period were reported to the authorities. The source of the outbreak was contaminated chicken meat that came from the same producer. The reason for the increased incidence and elevated levels of Campylobacter was reported to be an improperly installed washing plant, where dirty water was accidentally used to wash transport cages.[51]
United Kingdom
In January 2013, the
United States
Campylobacter infections increased 14% in the United States in 2012 compared to the rate from 2006 to 2008. This represents the highest reported number of infections since calendar year 2000.[31]
High prevalence of Campylobacter (40% or more) has been reported in raw chicken meat in regional retail stores in the US, which remained steady from 2005 through 2011.
See also
References
- ^ PMID 9396691.
- ^ ISBN 978-0-387-24145-6.
- ^ PMID 17368847.
- PMID 19201953.
- PMID 26686808.
- ^ ISBN 978-0-8385-8529-0.
- PMID 15845230.
- ^ "Campylobacter". European Food Safety Authority. Retrieved 2020-11-02.
- ^ a b Campylobacter Infections at eMedicine
- S2CID 28539930.
- ^ "Information for Health Professionals | Campylobacter". Centers for Disease Control and Prevention. 2019-12-23. Retrieved 2020-11-02.
- ^ PMID 14605259.
- ^ PMID 17145081.
- PMID 10081669.
- PMID 15660156.
- ^ ISSN 1476-4687.
- PMID 8478066.
- PMID 36314601.
- ^ A.C. Parte; et al. "Campylobacter". List of Prokaryotic names with Standing in Nomenclature (LPSN). Retrieved 2023-09-09.
- ^ Sayers; et al. "Campylobacter". National Center for Biotechnology Information (NCBI) taxonomy database. Retrieved 2023-09-09.
- ^ "The LTP". Retrieved 20 November 2023.
- ^ "LTP_all tree in newick format". Retrieved 20 November 2023.
- ^ "LTP_08_2023 Release Notes" (PDF). Retrieved 20 November 2023.
- ^ "GTDB release 08-RS214". Genome Taxonomy Database. Retrieved 10 May 2023.
- ^ "bac120_r214.sp_label". Genome Taxonomy Database. Retrieved 10 May 2023.
- ^ "Taxon History". Genome Taxonomy Database. Retrieved 10 May 2023.
- ^ S2CID 46270047.
- PMID 5693467.
- ^ Fletcher, RD (1965). "Activity and morphology of Vibrio coli phage". American Journal of Veterinary Research. 26 (111): 361–4.
- PMID 18023831.
- ^ a b c d "Infections from some foodborne germs increased, while others remained unchanged in 2012" (Press release). CDC. April 18, 2013. Retrieved October 22, 2015.
- PMID 25416162.
- S2CID 44823836.
- PMID 36430700.
- .
- PMID 30783889.
- ^ PMID 12788755.
- PMID 17278062.
- S2CID 22460970.
- PMID 19000862.
- PMID 20038624.
- PMID 33755697.
- ^ "FoodNet Canada 2014 Short Report". Public Health Agency of Canada, FoodNet Canada. 2016-01-12. Retrieved 3 October 2016.
- ISSN 0934-9723.
- ^ Sharpe, Marty (19 August 2016). "Woman died in Havelock North gastro outbreak". Stuff.
- ^ "Govt rejects call for Hawke's Bay water emergency declaration". Radio New Zealand. 19 August 2016.
- S2CID 220306856.
- ^ Olsen, Adrian Nyhammer; Baisotti, Valentina (11 June 2019). "Fant samme bakterie i drikkevannet som hos sykehuspasienter fra Askøy" (in Norwegian Bokmål). NRK.
- PMID 31748129.
- PMID 33194843.
- ^ "Utbrott av anmälningspliktiga sjukdomar i Sverige 2017" [Outbreaks of notifiable diseases in Sweden in 2017] (in Swedish). Folkhälsomyndigheten. 2018-05-09. Retrieved 27 May 2020.
- ^ Ward, Victoria (January 23, 2013). "FSA warns that chicken bacteria could be next meat scandal". The Telegraph.
- ^ "Food Safety Week 2014: 'Don't wash raw chicken'". Food Standards Agency. Archived from the original on November 8, 2014.
- ^ "Campylobacter survey: cumulative results from the full 12 months (Q1 – Q4)" (Press release). Food Standards Agency. May 28, 2015. Retrieved October 23, 2015.
- PMID 22920043.
- ^ "Quarterly Progress Report on Salmonella and Campylobacter". Testing of Selected Raw Meat and Poultry Products: Preliminary Results, July 2014 to September 2014. Food Safety and Inspection Service. United States Department of Agriculture. 2015-04-24.
