Molar pregnancy
| Molar pregnancy | |
|---|---|
| Other names | Hydatid mole, hydatidiform mole |
 | |
| Histopathologic image of hydatidiform mole (complete type). H&E stain. | |
| Specialty | Obstetrics |
A molar pregnancy, also known as a hydatidiform mole, is an abnormal form of
A complete mole is caused by either a single
Complete moles carry a 2–4% risk, in Western countries, of developing into
Molar pregnancies are relatively rare complications of pregnancy, occurring in approximately 1 in 1,000 pregnancies in the United States, while in Asia, the rates are considerably higher, reaching up to 1 in 100 pregnancies in countries like Indonesia.[4]
Signs and symptoms

Molar pregnancies usually present with painless vaginal bleeding in the fourth to fifth months of pregnancy.
Cause
The cause of this condition is not completely understood. Potential risk factors may include defects in the egg, abnormalities within the
Pathophysiology
A hydatidiform mole is a pregnancy/
Based on

In rare cases, a hydatidiform mole co-exists in the uterus with a normal, viable fetus. These cases are due to
Parental origin
In most complete moles, all
Most partial moles are
In rare cases, hydatidiform moles are
A small percentage of hydatidiform moles have biparental diploid genomes, as in normal living persons; they have two sets of chromosomes, one inherited from each biological parent. Some of these moles occur in women who carry mutations in the gene NLRP7, predisposing them towards molar pregnancy. These rare variants of hydatidiform mole may be complete or partial.[11][12][13]
Diagnosis


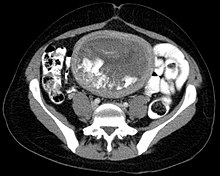
The diagnosis is strongly suggested by
Sometimes symptoms of hyperthyroidism are seen, due to the extremely high levels of hCG, which can mimic the effects of thyroid-stimulating hormone.[15]
| Complete Mole | Partial Mole | |
|---|---|---|
| Karyotype[16] | 46,XX or 46,XY | 69,XXY or 69, XXX |
| hCG | ↑↑↑↑ | ↑ |
| Uterine Size | ↑ | –[clarification needed] |
| Fetal Parts | No | Yes |
| Components[16] | 2 sperm + empty egg
or Empty egg + 1 sperm that duplicates |
2 sperm + 1 egg
or 1 sperm + 1 egg that duplicates |
| Risk of Choriocarcinoma[17] | 15% | 0.5% |
Treatment
Hydatidiform moles should be treated by evacuating the uterus by uterine suction or by surgical
Management is more complicated when the mole occurs together with one or more normal fetuses.
In some women, the growth can develop into gestational trophoblastic neoplasia. For women who have complete hydatidiform mole and are at high risk of this progression, evidence suggests giving prophylactic chemotherapy (known as P-chem) may reduce the risk of this happening.[19] However P-chem may also increase toxic side effects, so more research is needed to explore its effects.[19]
Anesthesia
The uterine curettage is generally done under the effect of anesthesia, preferably spinal anesthesia in hemodynamically stable patients. The advantages of spinal anesthesia over general anesthesia include ease of technique, favorable effects on the pulmonary system, safety in patients with hyperthyroidism and non-tocolytic pharmacological properties. Additionally, by maintaining patient's consciousness one can diagnose the complications like uterine perforation, cardiopulmonary distress and thyroid storm at an earlier stage than when the patient is sedated or is under general anesthesia.[20]
Prognosis
More than 80% of hydatidiform moles are
In 10 to 15% of cases, hydatidiform moles may develop into invasive moles. This condition is named
In 2 to 3% of cases, hydatidiform moles may develop into choriocarcinoma, which is a malignant, rapidly growing, and metastatic (spreading) form of cancer. Despite these factors which normally indicate a poor prognosis, the rate of cure after treatment with chemotherapy is high.
Over 90% of women with malignant, non-spreading cancer are able to survive and retain their ability to conceive and bear children. In those with metastatic (spreading) cancer, remission remains at 75 to 85%, although their childbearing ability is usually lost.
Epidemiology
Hydatidiform moles are a rare complication of pregnancy, occurring once in every 1,000 pregnancies in the US, with much higher rates in Asia (e.g. up to one in 100 pregnancies in Indonesia).[4]
Etymology
The etymology is derived from hydatisia (Greek "a drop of water"), referring to the watery contents of the cysts, and mole (from Latin mola = millstone/false conception).[22] The term, however, comes from the similar appearance of the cyst to a hydatid cyst in an echinococcosis.[23]
References
- ^ "About molar pregnancy | Gestational trophoblastic disease (GTD) | Cancer Research UK". www.cancerresearchuk.org. Retrieved 18 June 2022.
- Merriam Webster. Retrieved May 7, 2012.
- ^ ISBN 978-1-4377-0792-2.
- ^ PMID 9443567.
- ISBN 0-7216-0187-1.
- ISBN 0-07-144159-X.
- ^ MedlinePlus Encyclopedia: Hydatidiform mole
- PMID 17413849.
- S2CID 33752037.
- ISBN 0-340-81662-7.
- PMID 1674641.
- S2CID 1417706.
- S2CID 32421323. Review.
- S2CID 6572375.
- ^ a b "The 6 questions that pregnant women should be ask to the doctor". HealthGuru. 15 March 2019.
- ^ PMID 29083593, retrieved 2024-01-16
- PMID 26566410.
- ISBN 0-7216-0187-1.
- ^ PMID 28892119.
- PMID 22223914.
- ^ PMID 22439034.
- ^ Entries HYDATID n. (a.) and MOLE, n.6 in the Oxford English Dictionary online. (http://dictionary.oed.com/ — subscription required.)
- ^ "Hydatidiform".
External links
- Humpath #3186 Archived 2011-09-30 at the Wayback Machine (Pathology images)
- Clinically reviewed molar pregnancy and choriocarcinoma information for patients from Cancer Research UK
- MyMolarPregnancy.com: Resource for those diagnosed with molar pregnancy. Links, personal stories, and support groups.
