Anemia
| Anemia | |
|---|---|
| Other names | Anaemia, erythrocytopenia |
Blood loss, decreased red blood cell production, increased red blood cell breakdown[1] | |
| Diagnostic method | Blood hemoglobin measurement[1] |
| Frequency | 2.36 billion / 33% (2015)[2] |
Anemia or anaemia (
Anemia can be caused by
Treatment depends on the specific cause. Certain groups of individuals, such as pregnant women, can benefit from the use of
Anemia is the most common blood disorder, affecting about a fifth to a third of the global population.
Signs and symptoms

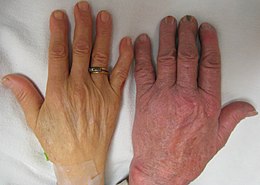
A person with anemia may not have any symptoms, depending on the underlying cause, and no symptoms may be noticed, as the anemia is initially mild, and then the symptoms become worse as the anemia worsens. A patient with anemia may report feeling tired, weak, decreased ability to concentrate, and sometimes shortness of breath on exertion.[19] These symptoms are unspecific and none of the symptoms alone or in combination show a good predictive value for the presence of anemia in non-clinical patients.[20]

Symptoms of anemia can come on quickly or slowly.
In more severe anemia, the body may compensate for the lack of oxygen-carrying capability of the blood by increasing
On examination, the signs exhibited may include
Causes
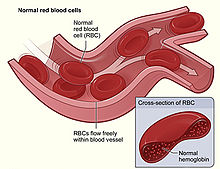
The causes of anemia may be classified as impaired red blood cell (RBC) production, increased RBC destruction (hemolytic anemia), blood loss and fluid overload (hypervolemia). Several of these may interplay to cause anemia. The most common cause of anemia is blood loss, but this usually does not cause any lasting symptoms unless a relatively impaired RBC production develops, in turn, most commonly by iron deficiency.[4]
Impaired production
- Disturbance of proliferation and differentiation of stem cells
- Pure red cell aplasia[28]
- Aplastic anemia[28] affects all kinds of blood cells. Fanconi anemia is a hereditary disorder or defect featuring aplastic anemia and various other abnormalities.
- Anemia of kidney failure[28] due to insufficient production of the hormone erythropoietin
- Anemia of endocrine disease[29]
- Disturbance of proliferation and maturation of erythroblasts
- Pernicious anemia[28] is a form of megaloblastic anemia due to vitamin B12 deficiency dependent on impaired absorption of vitamin B12. Lack of dietary B12 causes non-pernicious megaloblastic anemia.
- Anemia of folate deficiency,[28] as with vitamin B12, causes megaloblastic anemia
- Anemia of prematurity, by diminished erythropoietin response to declining hematocrit levels, combined with blood loss from laboratory testing, generally occurs in premature infants at two to six weeks of age.
- Iron-deficiency anemia, resulting in deficient heme synthesis[28]
- Thalassemias, causing deficient globin synthesis[28]
- Congenital dyserythropoietic anemias, causing ineffective erythropoiesis
- Anemia of kidney failure[28] (also causing stem cell dysfunction)
- Other mechanisms of impaired RBC production
- myelophthisisis a severe type of anemia resulting from the replacement of bone marrow by other materials, such as malignant tumors, fibrosis, or granulomas.
- Myelodysplastic syndrome[28]
- anemia of chronic inflammation[28]
- Leukoerythroblastic anemia is caused by space-occupying lesions in the bone marrow that prevent normal production of blood cells.[30]
Increased destruction
Anemias of increased red blood cell destruction are generally classified as hemolytic anemias. These types generally feature jaundice, and elevated levels of lactate dehydrogenase.[31][32]
- Intrinsic (intracorpuscular) abnormalities[28] cause premature destruction. All of these, except paroxysmal nocturnal hemoglobinuria, are hereditary genetic disorders.[33]
- Hereditary spherocytosis[28] is a hereditary defect that results in defects in the RBC cell membrane, causing the erythrocytes to be sequestered and destroyed by the spleen.
- Hereditary elliptocytosis[28] is another defect in membrane skeleton proteins.
- Abetalipoproteinemia,[28] causing defects in membrane lipids
- Enzyme deficiencies
- Pyruvate kinase and hexokinase deficiencies,[28] causing defect glycolysis
- Glucose-6-phosphate dehydrogenase deficiency and glutathione synthetase deficiency,[28] causing increased oxidative stress
- Hemoglobinopathies
- Paroxysmal nocturnal hemoglobinuria[28]
- Extrinsic (extracorpuscular) abnormalities
- Antibody-mediated
- systemic lupus erythematosus, or a malignancy, such as chronic lymphocytic leukemia.[35]
- Cold agglutinin hemolytic anemia is primarily mediated by IgM. It can be idiopathic[36]or result from an underlying condition.
- Rh disease,[28] one of the causes of hemolytic disease of the newborn
- Transfusion reaction to blood transfusions[28]
- Mechanical trauma to red blood cells
- Microangiopathic hemolytic anemias, including thrombotic thrombocytopenic purpura and disseminated intravascular coagulation[28]
- Infections, including malaria[28]
- Heart surgery[medical citation needed]
- Haemodialysis[medical citation needed]
- Parasitic
- Trypanosoma congolense alters the surfaces of RBCs of its host and this may explain T. c. induced anemia[37]
- Antibody-mediated
Blood loss
- Anemia of prematurity, from frequent blood sampling for laboratory testing, combined with insufficient RBC production
- , causing acute blood loss
- Gastrointestinal tract lesions,)
- Gynecologic disturbances,[28] also generally causing chronic blood loss
- From menstruation, mostly among young women or older women who have fibroids
- Many type of cancers, including colorectal urinary bladder, may cause acute or chronic blood loss, especially at advanced stages
- Infection by intestinal
- Iatrogenic anemia, blood loss from repeated blood draws and medical procedures.[41][42]
The roots of the words anemia and ischemia both refer to the basic idea of "lack of blood", but anemia and
Fluid overload
Fluid overload (hypervolemia) causes decreased hemoglobin concentration and apparent anemia:[44]
- General causes of hypervolemia include excessive sodium or fluid intake, sodium or water retention and fluid shift into the intravascular space.[45]
- From the 6th week of pregnancy, hormonal changes cause an increase in the mother's blood volume due to an increase in plasma.[46]
Intestinal inflammation
Certain gastrointestinal disorders can cause anemia. The mechanisms involved are multifactorial and not limited to malabsorption but mainly related to chronic intestinal inflammation, which causes dysregulation of hepcidin that leads to decreased access of iron to the circulation.[47][48][49]
- Helicobacter pylori infection.[50]
- Gluten-related disorders: untreated celiac disease[49][50] and non-celiac gluten sensitivity.[51] Anemia can be the only manifestation of celiac disease, in absence of gastrointestinal or any other symptoms.[52]
- Inflammatory bowel disease.[53][54]
Diagnosis


Definitions
There are a number of definitions of anemia; reviews provide comparison and contrast of them.[55] A strict but broad definition is an absolute decrease in red blood cell mass,[56] however, a broader definition is a lowered ability of the blood to carry oxygen.[57] An operational definition is a decrease in whole-blood hemoglobin concentration of more than 2 standard deviations below the mean of an age- and sex-matched reference range.[58]
It is difficult to directly measure RBC mass,[59] so the hematocrit (amount of RBCs) or the hemoglobin (Hb) in the blood are often used instead to indirectly estimate the value.[60] Hematocrit; however, is concentration dependent and is therefore not completely accurate. For example, during pregnancy a woman's RBC mass is normal but because of an increase in blood volume the hemoglobin and hematocrit are diluted and thus decreased. Another example would be bleeding where the RBC mass would decrease but the concentrations of hemoglobin and hematocrit initially remains normal until fluids shift from other areas of the body to the intravascular space.[citation needed]
The anemia is also classified by severity into mild (110 g/L to normal), moderate (80 g/L to 110 g/L), and severe anemia (less than 80 g/L) in adults.[61] Different values are used in pregnancy and children.[61]
Testing
Anemia is typically diagnosed on a complete blood count. Apart from reporting the number of red blood cells and the hemoglobin level, the automatic counters also measure the size of the red blood cells by flow cytometry, which is an important tool in distinguishing between the causes of anemia. Examination of a stained blood smear using a microscope can also be helpful, and it is sometimes a necessity in regions of the world where automated analysis is less accessible.[citation needed]
| Age or gender group | Hb threshold (g/dL) | Hb threshold (mmol/L) |
|---|---|---|
| Children (0.5–5.0 yrs) | 11.0 | 6.8 |
| Children (5–12 yrs) | 11.5 | 7.1 |
| Teens (12–15 yrs) | 12.0 | 7.4 |
| Women, non-pregnant (>15yrs) | 12.0 | 7.4 |
| Women, pregnant | 11.0 | 6.8 |
| Men (>15yrs) | 13.0 | 8.1 |
A blood test will provide counts of white blood cells, red blood cells and platelets. If anemia appears, further tests may determine what type it is, and whether it has a serious cause. although of that, it is possible to refer to the genetic history and physical diagnosis.[63] These tests may also include serum ferritin, iron studies, vitamin B12, genetic testing, and a bome morrow sample, if needed.[64][65]
Reticulocyte counts, and the "kinetic" approach to anemia, have become more common than in the past in the large medical centers of the United States and some other wealthy nations, in part because some automatic counters now have the capacity to include reticulocyte counts. A reticulocyte count is a quantitative measure of the bone marrow's production of new red blood cells. The reticulocyte production index is a calculation of the ratio between the level of anemia and the extent to which the reticulocyte count has risen in response. If the degree of anemia is significant, even a "normal" reticulocyte count actually may reflect an inadequate response. If an automated count is not available, a reticulocyte count can be done manually following special staining of the blood film. In manual examination, activity of the bone marrow can also be gauged qualitatively by subtle changes in the numbers and the morphology of young RBCs by examination under a microscope. Newly formed RBCs are usually slightly larger than older RBCs and show polychromasia. Even where the source of blood loss is obvious, evaluation of erythropoiesis can help assess whether the bone marrow will be able to compensate for the loss and at what rate. When the cause is not obvious, clinicians use other tests, such as:
Red blood cell size
In the morphological approach, anemia is classified by the size of red blood cells; this is either done automatically or on microscopic examination of a peripheral blood smear. The size is reflected in the
Production vs. destruction or loss
The "kinetic" approach to anemia yields arguably the most clinically relevant classification of anemia. This classification depends on evaluation of several hematological parameters, particularly the blood
| Anemia | |||||||||||||||||||||||||||||||||
| Reticulocyte production index shows inadequate production response to anemia. | Reticulocyte production index shows appropriate response to anemia = ongoing hemolysis or blood loss without RBC production problem. | ||||||||||||||||||||||||||||||||
| No clinical findings consistent with hemolysis or blood loss: pure disorder of production. | Clinical findings and abnormal MCV: hemolysis or loss and chronic disorder of production*. | Clinical findings and normal MCV= acute hemolysis or loss without adequate time for bone marrow production to compensate**. | |||||||||||||||||||||||||||||||
| Macrocytic anemia (MCV>100) | Normocytic anemia (80<MCV<100) | Microcytic anemia (MCV<80) | |||||||||||||||||||||||||||||||
* For instance, sickle cell anemia with superimposed iron deficiency; chronic gastric bleeding with B12 and folate deficiency; and other instances of anemia with more than one cause.
** Confirm by repeating reticulocyte count: ongoing combination of low reticulocyte production index, normal MCV and hemolysis or loss may be seen in bone marrow failure or anemia of chronic disease, with superimposed or related hemolysis or blood loss.
Here is a schematic representation of how to consider anemia with MCV as the starting point:
| Anemia | |||||||||||||||||||||||||||||||||||||||||||
| Macrocytic anemia (MCV>100) | Normocytic anemia (MCV 80–100) | Microcytic anemia (MCV<80) | |||||||||||||||||||||||||||||||||||||||||
| High reticulocyte count | Low reticulocyte count | ||||||||||||||||||||||||||||||||||||||||||
Other characteristics visible on the peripheral smear may provide valuable clues about a more specific diagnosis; for example, abnormal white blood cells may point to a cause in the bone marrow.
Microcytic
Microcytic anemia is primarily a result of hemoglobin synthesis failure/insufficiency, which could be caused by several etiologies:
- Heme synthesis defect
- Iron-deficiency anemia (microcytosis is not always present)
- Anemia of chronic disease (more commonly presenting as normocytic anemia)
- Globin synthesis defect
- Alpha-, and beta-thalassemia
- HbE syndrome
- HbC syndrome
- Various other unstable hemoglobin diseases
- Sideroblasticdefect
- Hereditary sideroblastic anemia
- Acquired sideroblastic anemia, including lead toxicity[66]
- Reversible sideroblastic anemia
Iron-deficiency anemia is the most common type of anemia overall and it has many causes. RBCs often appear hypochromic (paler than usual) and microcytic (smaller than usual) when viewed with a microscope.
- Iron-deficiency anemia is due to insufficient dietary intake or absorption of angular stomatitis).
- In the United States, the most common cause of iron deficiency is bleeding or blood loss, usually from the gastrointestinal tract. Fecal occult blood testing, upper endoscopy and lower endoscopy should be performed to identify bleeding lesions. In older men and women, the chances are higher that bleeding from the gastrointestinal tract could be due to colon polyps or colorectal cancer.
- Worldwide, the most common cause of iron-deficiency anemia is parasitic infestation (
The Mentzer index (mean cell volume divided by the RBC count) predicts whether microcytic anemia may be due to iron deficiency or thalassemia, although it requires confirmation.[73][citation needed]
Macrocytic
- folic acid, or both.[74] Deficiency in folate or vitamin B12 can be due either to inadequate intake or insufficient absorption. Folate deficiency normally does not produce neurological symptoms, while B12 deficiency does.
- autoimmune condition targeting the parietal cells(atrophic gastritis) that produce intrinsic factor or against intrinsic factor itself. These lead to poor absorption of vitamin B12.
- Macrocytic anemia can also be caused by the removal of the functional portion of the stomach, such as during gastric bypasssurgery, leading to reduced vitamin B12/folate absorption. Therefore, one must always be aware of anemia following this procedure.
- Hypothyroidism
- Alcoholism commonly causes a macrocytosis, although not specifically anemia. Other types of liver disease can also cause macrocytosis.
- Drugs such as methotrexate, zidovudine, and other substances may inhibit DNA replication such as heavy metals
Macrocytic anemia can be further divided into "megaloblastic anemia" or "nonmegaloblastic macrocytic anemia". The cause of megaloblastic anemia is primarily a failure of DNA synthesis with preserved RNA synthesis, which results in restricted cell division of the progenitor cells. The megaloblastic anemias often present with neutrophil hypersegmentation (six to 10 lobes). The nonmegaloblastic macrocytic anemias have different etiologies (i.e. unimpaired DNA globin synthesis,) which occur, for example, in alcoholism. In addition to the nonspecific symptoms of anemia, specific features of vitamin B12 deficiency include
Normocytic
Normocytic anemia occurs when the overall hemoglobin levels are decreased, but the red blood cell size (mean corpuscular volume) remains normal. Causes include:
- Acute blood loss
- Anemia of chronic disease
- Aplastic anemia (bone marrow failure)
- Hemolytic anemia
Dimorphic
A dimorphic appearance on a peripheral blood smear occurs when there are two simultaneous populations of red blood cells, typically of different size and hemoglobin content (this last feature affecting the color of the red blood cell on a stained peripheral blood smear). For example, a person recently transfused for iron deficiency would have small, pale, iron deficient red blood cells (RBCs) and the donor RBCs of normal size and color. Similarly, a person transfused for severe folate or vitamin B12 deficiency would have two cell populations, but, in this case, the patient's RBCs would be larger and paler than the donor's RBCs. A person with sideroblastic anemia (a defect in heme synthesis, commonly caused by alcoholism, but also drugs/toxins, nutritional deficiencies, a few acquired and rare congenital diseases) can have a dimorphic smear from the sideroblastic anemia alone. Evidence for multiple causes appears with an elevated RBC distribution width (RDW), indicating a wider-than-normal range of red cell sizes, also seen in common nutritional anemia.[citation needed]
Heinz body anemia
- In cats and dogs after eating either raw or cooked plants from the genus Allium, for example, onions or garlic.[78]
- In dogs after ingestion of zinc, for example, after eating U.S. pennies minted after 1982.[77]
- In horses which eat dry or wilted red maple leaves.[79]
Hyperanemia
Hyperanemia is a severe form of anemia, in which the hematocrit is below 10%.[80]
Refractory anemia
Refractory anemia, an anemia which does not respond to
Transfusion dependent
Transfusion dependent anemia is a form of anemia where ongoing blood transfusion are required.[84] Most people with myelodysplastic syndrome develop this state at some point in time.[85] Beta thalassemia may also result in transfusion dependence.[86][87] Concerns from repeated blood transfusions include iron overload.[85] This iron overload may require chelation therapy.[88]
Treatment
The global market for anemia treatments is estimated at more than USD 23 billion per year and is fast growing because of the rising prevalence and awareness of anemia. The types of anemia treated with drugs are
Oral iron
Nutritional iron deficiency is common in developing nations. An estimated two-thirds of children and of women of childbearing age in most developing nations are estimated to have iron deficiency without anemia; one-third of them have iron deficiency with anemia.[89] Iron deficiency due to inadequate dietary iron intake is rare in men and postmenopausal women. The diagnosis of iron deficiency mandates a search for potential sources of blood loss, such as gastrointestinal bleeding from ulcers or colon cancer.[citation needed]
Mild to moderate iron-deficiency anemia is treated by oral iron supplementation with
In the anemia of chronic kidney disease,
Injectable iron
In cases where oral iron has either proven ineffective, would be too slow (for example, pre-operatively), or where absorption is impeded (for example in cases of inflammation),
Blood transfusions
Blood transfusions in those without symptoms is not recommended until the hemoglobin is below 60 to 80 g/L (6 to 8 g/dL).[1] In those with coronary artery disease who are not actively bleeding transfusions are only recommended when the hemoglobin is below 70 to 80g/L (7 to 8 g/dL).[10] Transfusing earlier does not improve survival.[95] Transfusions otherwise should only be undertaken in cases of cardiovascular instability.[96]
A 2012 review concluded that when considering blood transfusions for anaemia in people with advanced cancer who have fatigue and breathlessness (not related to cancer treatment or haemorrhage), consideration should be given to whether there are alternative strategies can be tried before a blood transfusion.[97]
Vitamin B12 intramuscular injections
In many cases, vitamin B12 is used by intramuscular injection in severe cases or cases of malabsorption of dietary-B12. Pernicious anemia caused by loss of intrinsic factor cannot be prevented.[98] If there are other, reversible causes of low vitamin B12 levels, the cause must be treated.[99]
Vitamin B12 deficiency anemia is usually easily treated by providing the necessary level of vitamin B12 supplementation.[100] The injections are quick-acting, and symptoms usually go away within one to two weeks.[100] As the condition improves, doses are reduced to weeks and then can be given monthly. Intramuscular therapy leads to more rapid improvement and should be considered in patients with severe deficiency or severe neurologic symptoms.[100] Treatment should begin rapidly for severe neurological symptoms, as some changes can become permanent.[101] In some individuals lifelong treatment may be needed.[101]
Erythropoiesis-stimulating agents
The objective for the administration of an
Hyperbaric oxygen
Treatment of exceptional blood loss (anemia) is recognized as an indication for
Preoperative anemia
An estimated 30% of adults who require non-cardiac surgery have anemia.[108] In order to determine an appropriate preoperative treatment, it is suggested that the cause of anemia be first determined.[109] There is moderate level medical evidence that supports a combination of iron supplementation and erythropoietin treatment to help reduce the requirement for red blood cell transfusions after surgery in those who have preoperative anemia.[108]
Epidemiology
Anemia affects 27% of the world's population with iron-deficiency anemia accounting for more than 60% of it.[110] A moderate degree of iron-deficiency anemia affected approximately 610 million people worldwide or 8.8% of the population.[13] It is somewhat more common in females (9.9%) than males (7.8%).[13] Mild iron-deficiency anemia affects another 375 million.[13] Severe anaemia is prevalent globally, and especially in sub-Saharan Africa[111] where it is associated with infections including malaria and invasive bacterial infections.[112]
History
This section needs expansion. You can help by adding to it. (August 2020) |
Signs of severe anemia in human bones from 4000 years ago have been uncovered in Thailand.[113]
References
- ^ PMID 24716235.
- ^ PMID 27733282.
- ^ "Anemia: Practice Essentials, Pathophysiology, Etiology". 9 November 2021. Retrieved 8 February 2022.
- ^ a b "Anemia | NHLBI, NIH". www.nhlbi.nih.gov. Retrieved 8 February 2022.
- ^ "anaemia". Dictionary.com. Archived from the original on 14 July 2014. Retrieved 7 July 2014.
- ^ "Anemia - Symptoms and causes". Mayo Clinic. Retrieved 1 April 2022.
- PMID 20297873.
- PMID 30855920. Retrieved 4 May 2019.
- S2CID 11748341.
- ^ S2CID 4712203.
- PMID 26561626.
- ^ a b c "Anemia Treatment Drugs: 2019 Global Market Study; Analyzed by Type of Anemia, Type of Drug, and Geography". GlobeNewswire (Press release). 26 April 2019. Retrieved 2 August 2023.
- ^ PMID 23245607.
- PMID 25530442.
- ^ "WHO Global Anaemia estimates, 2021 Edition". Wolrd Health Organization. Retrieved 27 February 2022.
- ^ "WHO | Interventions by global target". www.who.int. World Health Organization. Archived from the original on 14 August 2016.
- ^ "The case for action on anemia". Devex. 14 June 2016.
- ^ a b eMedicineHealth > anemia article Archived 2009-04-17 at the Wayback Machine Author: Saimak T. Nabili, MD, MPH. Editor: Melissa Conrad Stöppler, MD. Last Editorial Review: 12/9/2008. Retrieved on 4 April 2009
- ^ "Exercising With Anemia: Prescription for Health". Medscape. Retrieved 8 January 2022.
- PMID 36769569.
- ^ a b c d "What Are Symptoms of Anemia?". National Heart, Lung, and Blood Institute. 24 March 2022. Retrieved 26 June 2022.
- ^ "Anemia". www.hematology.org. Retrieved 8 January 2022.
- PMID 28528999.
- ISBN 9781451154542.
- ^ "Mental Health and Pica". WebMD. Retrieved 26 April 2022.
- S2CID 35587006.
- ^ "Sickle Cell Disease". National Heart, Lung, and Blood Institute. 22 July 2022.
- ^ ISBN 978-1-4160-2973-1.
- ^ Gregg XT, Prchal JT (2007). "Anemia of Endocrine Disorders". Williams Hermatology. McGraw-Hill.
- ^ "the definition of leukoerythroblastosis". www.dictionary.com. Archived from the original on 2 December 2018. Retrieved 2 December 2018.
- ^ Despotovic J, Mahoney D, Armsby C (2021). "Overview of hemolytic anemias in children". The Lecturio Medical Concept Library. UpToDate. Retrieved 28 June 2021.
- )
- ISBN 978-1-4160-2973-1.
- ISBN 978-0-7216-0187-8.
- ^ "Autoimmune Hemolytic Anemia (AIHA)" By J.L. Jenkins. The Regional Cancer Center. 2001 Archived October 7, 2009, at the Wayback Machine
- PMID 17891600.
- PMID 17560035.
- ^ "Do Hemorrhoids Cause Iron Deficiency Anemia?". 26 June 2018.
- PMID 18820740.
- S2CID 205391965.
- PMID 31399052.
- S2CID 30859103.
- PMID 16700423.
- PMID 25559015.
- ISBN 978-1-58255-678-9.
- ^ "ISBT: 8. Obstetric anaemia". www.isbtweb.org. Retrieved 22 May 2018.
- PMID 28067386.
- PMID 24707137.
- ^ S2CID 15561525.
- ^ PMID 27672287.
- PMID 24077239.
- PMID 15825115.
- PMID 21450124.
- PMID 21564345.
- PMID 16189263.
- ^ Anemia at eMedicine
- ISBN 978-1-4160-3006-5. Archivedfrom the original on 25 April 2016.
- ISBN 978-0-323-29854-4.
- ISBN 978-0-323-35232-1. Archivedfrom the original on 31 October 2016.
- ISBN 978-1-60473-701-1. Archivedfrom the original on 31 October 2016.
- ^ hdl:10665/85839.
- ISBN 978-92-4-159665-7. Archived(PDF) from the original on 12 March 2009. Retrieved 25 March 2009.
- ^ "Anemia". Radiologyinfo.org. Retrieved 11 October 2021.
- ^ "How Anemia Is Diagnosed and Treated". WebMD. Retrieved 11 October 2021.
- ^ "Anemia Types, Treatment, Symptoms, Signs, Causes & Iron Deficiency". eMedicineHealth. Retrieved 11 October 2021.
- PMID 28731309.
- ^ Recommendations to Prevent and Control Iron Deficiency in the United States Archived 2007-04-20 at the Wayback Machine MMWR 1998;47 (No. RR-3) p. 5
- from the original on 5 May 2012. Retrieved 21 April 2012.
- ^ "Global Iron-Deficiency Anemia Therapy Market – Industry Trends and Forecast to 2027 -". Data Bridge Market Research. Retrieved 2 August 2023.
- S2CID 33404386.
- PMID 11160596.
- ^ "Iron Deficiency Anaemia: Assessment, Prevention, and Control: A guide for programme managers" (PDF). Archived from the original (PDF) on 16 May 2011. Retrieved 24 August 2010.
- PMID 4123424.
- ^ "Macrocytic Anemia - an overview". ScienceDirect Topics. Retrieved 26 April 2022.
- ^ eMedicine – "Vitamin B-12 Associated Neurological Diseases": Article by Niranjan N Singh, July 18, 2006. Archived 2007-03-15 at the Wayback Machine.
- ^ "Physiology or Medicine 1934 – Presentation Speech". Nobelprize.org. 10 December 1934. Archived from the original on 28 August 2010. Retrieved 24 August 2010.
- ^ ISBN 978-1-4377-0173-9.
- ISBN 978-1-119-03652-4.
- ISBN 978-0-323-24216-5.
- PMID 3577135.
- ^ "MedTerms Definition: Refractory Anemia". Medterms.com. 27 April 2011. Archived from the original on 8 December 2011. Retrieved 31 October 2011.
- ^ "Good Source for later". Atlasgeneticsoncology.org. Archived from the original on 3 November 2011. Retrieved 31 October 2011.
- S2CID 38832868.
- PMID 20692036.
- ^ PMID 18024657.
- ISBN 9780702036255.
- ISBN 978-1416022466.
- ISBN 978-0323378222.
- PMID 8901803.
- PMID 27087396.
- PMID 11952508.
- ^ "Anaemia management in people with chronic kidney disease | Guidance and guidelines | NICE". 9 February 2011. Archived from the original on 24 June 2013. Retrieved 9 August 2013.
- PMID 31811820.
- PMID 21239816.
- ^ S2CID 27062899.
- PMID 21561874.
- PMID 22336857.
- ^ "Pernicious anemia: MedlinePlus Medical Encyclopedia". medlineplus.gov. Retrieved 4 August 2022.
- OCLC 503441695.
- ^ PMID 28925645.
- ^ a b "Pernicious Anemia Clinical Presentation: History, Physical Examination". 14 September 2017. Archived from the original on 14 September 2017. Retrieved 4 August 2022.
- ^ PMID 18458123.
- ABIM Foundation, American Society of Nephrology, archived(PDF) from the original on 16 April 2012, retrieved 17 August 2012
- PMID 32790892.
- ^ a b c Undersea and Hyperbaric Medical Society. "Exceptional Blood Loss – Anemia". Archived from the original on 5 July 2008. Retrieved 19 May 2008.
- ^ Hart GB, Lennon PA, Strauss MB (1987). "Hyperbaric oxygen in exceptional acute blood-loss anemia". J. Hyperbaric Med. 2 (4): 205–210. Archived from the original on 16 January 2009. Retrieved 19 May 2008.
{{cite journal}}: CS1 maint: unfit URL (link) - PMID 15796315. Archived from the original on 16 January 2009.)
{{cite journal}}: CS1 maint: unfit URL (link - ^ PMID 32790892.
- S2CID 37709527.
- PMID 27040955.
- S2CID 205268648.
- PMID 32972031.
- PMID 8876811.
External links
[About Anemia]
