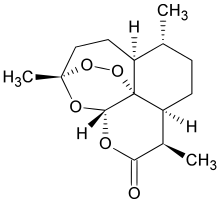
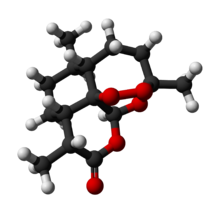
Artemisinin
 | |
 | |
| Clinical data | |
|---|---|
| Pronunciation | /ɑːrtɪˈmɪsɪnɪn/ |
| Other names | Artemisinine, qinghaosu |
| Routes of administration | Oral |
| ATC code | |
| Identifiers | |
| |
JSmol) | |
| Density | 1.24 ± 0.1 g/cm3 |
| Melting point | 152 to 157 °C (306 to 315 °F) |
| Boiling point | decomposes |
| |
| |
| | |
Artemisinin (
Artemisinin and its derivatives are all
Artemisinin and its derivatives have been used for the treatment of malarial and
Medical use
The
For
Artemisinins are not used for malaria prevention because of the extremely short activity (half-life) of the drug. To be effective, it would have to be administered multiple times each day.[citation needed]
Contraindications
The WHO recommends avoiding ACT for women in their first trimester of pregnancy due to a lack of research on artemisinin's safety in early pregnancy. Instead the WHO recommends a seven-day course of
Adverse effects
Artemisinins are generally well tolerated at the doses used to treat malaria.
Chemistry
An unusual component of the artemisinin molecules is an endoperoxide 1,2,4-trioxane ring. This is the main antimalarial centre of the molecule.[22] Modifications at carbon 10 (C10) position give rise to a variety of derivatives which are more powerful than the original compound.[23] Because the physical properties of artemisinin itself, such as poor bioavailability, limit its effectiveness, semisynthetic derivatives of artemisinin have been developed. Derivatives of dihydroartemisinin were made since 1976. Artesunate, arteether and artemether were first synthesized in 1986. Many derivatives have been produced of which artelinic acid, artemotil, artemisone, SM735, SM905, SM933, SM934, and SM1044 are among the most powerful compounds.[24][25] There are also simplified analogs in preclinical development.[26] Over 120 other derivatives have been prepared, but clinical testing has not been possible due to lack of financial support.[22]
Artemisinin is poorly soluble in oils and water. Therefore, it is typically administered via the digestive tract, either by oral or rectal administration. Artesunate however can be administered via the intravenous and intramuscular, as well as the oral and rectal routes.[27] A synthetic compound with a similar trioxolane structure (a ring containing three oxygen atoms) named RBx-11160[28] showed promise in in vitro testing. Phase II testing in patients with malaria was not as successful as hoped, but the manufacturer decided to start Phase III testing anyway.[29]
Mechanism of action
As of 2018, the exact mechanism of action of artemisinins has not been fully elucidated.
Resistance
Clinical evidence for artemisinin drug resistance in southeast Asia was first reported in 2008,[36] and was subsequently confirmed by a detailed study from western Cambodia.[37][38] Resistance in neighbouring Thailand was reported in 2012,[39] and in northern Cambodia, Vietnam and eastern Myanmar in 2014.[40][41] Emerging resistance was reported in southern Laos, central Myanmar and northeastern Cambodia in 2014.[40][41] The parasite's kelch gene on chromosome 13 appears to be a reliable molecular marker for clinical resistance in Southeast Asia.[42]
In 2011, the WHO stated that resistance to the most effective antimalarial drug, artemisinin, could unravel national Indian malaria control programs, which have achieved significant progress in the last decade. WHO advocates the rational use of antimalarial drugs and acknowledges the crucial role of community health workers in reducing malaria in the region.[43]
Artemisinins can be used alone, but this leads to a high rate of return of parasites and other drugs are required to clear the body of all parasites and prevent a recurrence. The WHO is pressuring manufacturers to stop making the uncompounded drug available to the medical community at large, aware of the catastrophe that would result if the malaria parasite developed resistance to artemisinins.[44]
Two main mechanisms of resistance drive Plasmodium resistance to antimalarial drugs. The first one is an efflux of the drug away from its action site due to mutations in different transporter genes (like pfcrt in chloroquine resistance) or an increased number of the gene copies (like pfmdr1 copy number in mefloquine resistance). The second is a change in the parasite target due to mutations in corresponding genes (like, at the cytosol level, dhfr and dhps in sulfadoxine-pyrimethamine resistance or, at the mitochondrion level, cytochrome b in atovaquone resistance). Resistance of P. falciparum to the new artemisinin compounds involves a novel mechanism corresponding to a quiescence phenomenon.[45]
As of 2020[update] future resistance research will make use of
Synthesis
Biosynthesis in Artemisia annua
The biosynthesis of artemisinin is believed to involve the

Chemical synthesis
The total synthesis of artemisinin has been performed from available organic starting materials, using basic organic reagents, many times. The first two total syntheses were a
A wide variety of further routes continue to be explored, from early days until today, including total synthesis routes from (R)-(+)-pulegone, isomenthene,[47] and even 2-cyclohexen-1-one,[50] as well as routes better described as partial or semisyntheses from a more plentiful biosynthetic precursor, artemisinic acid—in the latter case, including some very short and very high yielding biomimetic synthesis examples (of Roth and Acton, and Haynes et al., 3 steps, 30% yield), which again feature the singlet oxygen ene chemistry.[51][47][52][53]
Synthesis in engineered organisms
The partnership to develop semisynthetic artemisinin was led by PATH's Drug Development program (through an affiliation with OneWorld Health), with funding from the Bill & Melinda Gates Foundation. The project began in 2004, and initial project partners included the University of California, Berkeley (which provided the technology on which the project was based – a process that genetically altered yeast to produce artemisinic acid)[54] and Amyris (a biotechnology firm in California, which refined the process to enable large-scale production and developed scalable processes for transfer to an industrial partner).
In 2006, a team from UC Berkeley reported they had engineered Saccharomyces cerevisiae yeast to produce a small amount of the precursor artemisinic acid. The synthesized artemisinic acid can then be transported out, purified and chemically converted into artemisinin that they claim will cost roughly US$0.25 per dose. In this effort of synthetic biology, a modified mevalonate pathway was used, and the yeast cells were engineered to express the enzyme amorphadiene synthase and a cytochrome P450 monooxygenase (CYP71AV1), both from Artemisia annua. A three-step oxidation of amorpha-4,11-diene gives the resulting artemisinic acid.[55]
The UC Berkeley method was augmented using technology from various other organizations. The final successful technology is based on inventions licensed from UC Berkeley and the National Research Council (NRC) Plant Biotechnology Institute of Canada.[citation needed]
Commercial production of semisynthetic artemisinin is now underway at Sanofi's site in Garessio, Italy. This second source of artemisinin is poised to enable a more stable flow of key antimalarial treatments to those who need them most.[56] The production goal is set at 35 tonnes for 2013. It is expected to increase to 50–60 tons per year in 2014, supplying approximately one-third of the global annual need for artemisinin.[citation needed]
In 2013, WHO's Prequalification of Medicines Programme announced the acceptability of semisynthetic artemisinin for use in the manufacture of active pharmaceutical ingredients submitted to WHO for prequalification, or that have already been qualified by WHO.[57] Sanofi's active pharmaceutical ingredient (API) produced from semisynthetic artemisinin (artesunate) was also prequalified by WHO on May 8, 2013, making it the first semisynthetic artemisinin derivative prequalified.[citation needed]
In 2010, a team from
Production and price
China and Vietnam provide 70% and East Africa 20% of the raw plant material.[59] Seedlings are grown in nurseries and then transplanted into fields. It takes about 8 months for them to reach full size. The plants are harvested, the leaves are dried and sent to facilities where the artemisinin is extracted using a solvent, typically hexane. Alternative extraction methods have been proposed.[60] The market price for artemisinin has fluctuated widely, between US$120 and $1,200 per kilogram from 2005 to 2008.[61]
The Chinese company Artepharm created a combination artemisinin and piperaquine drug marketed as Artequick. In addition to clinical research performed in China and southeast Asia, Artequick was used in large-scale malaria eradication efforts in the Comoros. Those efforts, conducted in 2007, 2012, and 2013–14, produced a 95–97% reduction in the number of malaria cases in the Comoros.[62]
After negotiation with the WHO, Novartis and Sanofi provide ACT drugs at cost on a nonprofit basis; however, these drugs are still more expensive than other malaria treatments.[63] Artesunate injection for severe malaria treatment is made by the Guilin Pharmaceutical factory in China where production has received WHO prequalification.[64] High-yield varieties of Artemisia are being produced by the Centre for Novel Agricultural Products at the University of York using molecular breeding techniques.[61]
Using seed supplied by Action for Natural Medicine (ANAMED), the World Agroforestry Centre (ICRAF) has developed a hybrid, dubbed A3, which can grow to a height of 3 meters and produce 20 times more artemisinin than wild varieties. In northwestern Mozambique, ICRAF is working together with a medical organization, Médecins Sans Frontières, ANAMED and the Ministry of Agriculture and Rural Development to train farmers on how to grow the shrub from cuttings, and to harvest and dry the leaves to make artemisia tea. However, the WHO does not recommend the use of A. annua plant materials, including tea, for the prevention and treatment of malaria.[65]
In 2013, Sanofi announced the launch
A 2016 systematic review of four studies from East Africa concluded that subsidizing ACT in the private retail sector in combination with training and marketing has led to the increased availability of ACT in stores, increased use of ACT for febrile children under five years of age, and decrease in the use of older, less effective antimalarials among children under five years of age. The underlying studies did not determine if the children had malaria nor determine if there were health benefits.[68]
Metabolism
After ingestion or injection, artemisinin and its derivatives (arteether, artemether, and artesunate) are all rapidly converted in the bloodstream to dihydroartemisinin (DHA), which has 5–10 times greater antimalarial potency than artemisinin.[69] DHA is eventually converted in the liver into metabolites such as deoxyartemisinin, deoxydihydroartemisinin, and 9,10-dihydrodeoxyartemisinin. These reactions are catalyzed by the enzymes CYP2A6, CYP3A4, and CYP3A5, which belong to the cytochrome P450 group present in the smooth endoplasmic reticulum. These metabolites lack antimalarial properties due to the loss of the endoperoxide group (deoxyartemisinin however has anti-inflammatory and antiulcer properties.[70]) All these metabolites undergo glucuronidation, after which they are excreted through the urine or feces. Glucuronosyltransferases, in particular UGT1A9 and UGT2B7, are responsible for this process. DHA is also removed through bile as minor glucuronides. Due to their rapid metabolism, artemisinin and its derivatives are relatively safe drugs with a relatively high therapeutic index.[6]
History
Etymology
Artemisinin is an antimalarial lactone derived from qinghao (青蒿,
Discovery

Artemisia annua – a common herb found in many parts of the world. In 1967, a plant screening research program, under a secret military program code-named "Project 523", was set up by the People's Liberation Army to find an adequate treatment for malaria; the program and early clinical work were ordered by Mao Zedong at the request of North Vietnamese leaders to provide assistance for their malaria-ridden army.[72] In the course of this research in 1972, Tu Youyou discovered artemisinin in the leaves of Artemisia annua.[73]
Named qinghaosu (Chinese: 青蒿素; lit. 'compound of green-blue wormwood'),[73][74] it was one of many candidates tested as possible treatments for malaria by Chinese scientists, from a list of nearly 2,000 traditional Chinese medicines.[75] Tu Youyou also discovered that a low-temperature extraction process could be used to isolate an effective antimalarial substance from the plant. Tu says she was influenced by a traditional Chinese herbal medicine source The Handbook of Prescriptions for Emergency Treatments written in 340 CE by Ge Hong saying that this herb should be steeped in cold water.[76] This book contained the useful reference to the herb: "A handful of qinghao immersed with two litres of water, wring out the juice and drink it all."
Tu's team subsequently isolated an extract.[73] Results were published in the Chinese Medical Journal in 1979.[73][77][5] The extracted substance, once subject to purification, proved to be useful starting point to obtain purified artemisinin.[73] A 2012 review reported that artemisinin-based therapies were the most effective drugs for treatment of malaria at that time;[78] it was also reported to clear malaria parasites from patients' bodies faster than other drugs. In addition to artemisinin, Project 523 developed a number of products that can be used in combination with artemisinin, including lumefantrine, piperaquine, and pyronaridine.[73]
In the late 1990s, Novartis filed a new Chinese patent for a combination treatment with artemether/lumefantrine, providing the first artemisinin-based combination therapies (Coartem) at reduced prices to the WHO.[79] In 2006, after artemisinin had become the treatment of choice for malaria, the WHO called for an immediate halt to single-drug artemisinin preparations in favor of combinations of artemisinin with another malaria drug, to reduce the risk of parasites developing resistance.[80]
In 2011, Tu Youyou was awarded the
Research
New artemisinin-based combination therapies
The WHO notes four additional ACTs that are in preliminary clinical trials or regionally used for which there is no evidence to recommend widespread use: artesunate/pyronaridine, arterolane-piperaquine, artemisinin-piperaquine base, and artemisinin/naphthoquine.[82]
Helminthiasis
A serendipitous discovery was made in China in the early 1980s while searching for novel
Cancer
Artemisinin and its derivatives are under laboratory research for their potential anti-cancer effects.[1][86] As of 2018, only preliminary clinical research had been conducted using artemisininin derivatives in various cancers, with no approved clinical applications.[87]
Autoimmune disease
Artemisinin derivatives may suppress immune reactions, such as inflammation. One derivative, SM934, was approved in 2015 by the Chinese
See also
- Artemisia (genus)
- Artemisin
- Santonin
- Pharmacognosy
References
- ^ .
- ^ a b c "The Nobel Prize in Physiology or Medicine 2015". Nobel Foundation. Retrieved 2020-10-12.
- ^ a b c WHO 2015, pp. 9–11.
- PMID 18991643.
- ^ a b Brown G (2006). "Artemisinin and a new generation of antimalarial drugs". Education in Chemistry. 43 (4). Royal Society of Chemistry: 97–9. Retrieved 2018-03-09.
- ^ PMID 22992668.
- ^ "Development of Novel Antimalarials". MalariaWorld. September 6, 2010. Retrieved 2016-10-22.
- ^ "WHO calls for an immediate halt to provision of single-drug artemisinin malaria pills". WHO. 19 January 2006. Archived from the original on November 16, 2006.
- PMID 25855638.
- ^ Talman et al. 2019, "Artemisin, the Front-Line Compound against Malaria.
- ^ WHO 2015, p. 34.
- ^ a b c WHO 2015, p. 72.
- ^ WHO 2015, pp. 78–79.
- ^ WHO 2015, pp. 49–50.
- ^ WHO 2015, pp. 50–51.
- ^ WHO 2015, p. 52.
- ^ WHO 2015, pp. 55–56.
- ^ S2CID 28284347.
- PMID 11355556.
- ^ "Hepatitis Temporally Associated with an Herbal Supplement Containing Artemisinin — Washington, 2008". CDC.
- S2CID 13910573.
- ^ PMID 30855103.
- PMID 15701735.
- PMID 22922345.
- PMID 28230749.
- PMID 9925735.
- PMID 21914160.
- S2CID 4320974.
- ^ Unnikrishnan CH (September 21, 2007). "Blow to Ranbaxy drug research plans". livemint.com.
- S2CID 19133224.
- PMID 27289273.
- PMID 25470531.
- PMID 25910626.
- PMID 26694030.
- S2CID 24983411.
- PMID 19064625.
- ^ Morelle R (20 October 2015). "Drug-resistant malaria can infect African mosquitoes". BBC News. Retrieved 20 October 2015.
- PMID 19641202.
- PMID 22484134.
- ^ a b Briggs M (July 30, 2014). "Call for 'radical action' on drug-resistant malaria". BBC News. Retrieved 2013-07-30.
- ^ PMID 25075834.
- PMID 24352242.
- ^ "Drugs immunity 'may' fail malaria fight". The Jakarta Post. April 23, 2011. Archived from the original on 4 March 2016.
- PMID 16709988.
- PMID 29676250.

- PMID 32905757.
- ^ ISBN 978-0-470-12962-3.
- .
- S2CID 13460563.
- PMID 22866604.
- PMID 25898584.)
{{cite journal}}: CS1 maint: DOI inactive as of March 2024 (link - S2CID 32213495.
- .
- ^ Ball P (2016). "Man Made: A History of Synthetic Life". Distillations. 2 (1): 15–23. Retrieved 20 March 2018.
- S2CID 3199654.
- ^ a b Pantjushenko E. "Sanofi and PATH announce the launch of large-scale production of semisynthetic artemisinin against malaria". PATH.
- ^ Pantjushenko E. "Semisynthetic artemisinin achieves WHO prequalification". PATH. Retrieved 8 February 2014.
- PMID 21151979.
- ^ ole-MoiYoi K, Rodriguez W (2011). "Investing in Global Health: Botanical Extracts Ltd" (PDF). Global Health Delivery Project.
- doi:10.1039/b922001a. and literature cited therein
- ^ a b "Report of the Artemisinin Enterprise Conference 2008" (PDF). Archived from the original (PDF) on 2014-06-17. Retrieved 2011-07-12.
- ^ "Cure all?". The Economist. January 25, 2014. Retrieved 2016-10-22.
- ^ "Artemisinin combination therapies". CNAP Artemisia Project. University of York. Archived from the original on 2012-10-05. Retrieved 2011-07-12.
- ^ "Guilin Pharmaceutical ─ The world's first producer of WHO prequalified artesunate for injection for severe malaria". mmv.org. 2010. Archived from the original on 2016-10-22. Retrieved 2016-10-22.
- ^ "Effectiveness of Non-Pharmaceutical Forms of Artemisia annua L. against malaria". World Health Organization. Global Malaria Programme. Position Statement (June 2012). Retrieved April 2020.
- ^ Peplow M (April 2013). "Sanofi launches malaria drug production to maintain stability in artemisinin availability". Chemistryworld Online. RSC. Retrieved 2013-04-19.
- ^ Palmer E (19 August 2014). "Sanofi shipping new malaria treatment manufactured from 'semisynthetic artemisinin'". Fierce Pharma Manufacturing. Retrieved 2014-09-14.
- PMID 26954551.
- ISBN 978-0-7020-4064-1.
- PMID 33458540.
- PMC 4073852.
- ISBN 978-1-62212-164-9.
- ^ PMID 21907397.
- OCLC 41467509.
素:...5. 带有根本性质的物质 'substance with the fundamental properties of'
- ^ Katie Hunt and Shen Lu (6 October 2015). "Nobel Prize winner scoured ancient texts for malaria cure". CNN. Retrieved 2021-10-22.
- ^ Hao C (2011-09-29). "Lasker Award Rekindles Debate Over Artemisinin's Discovery". Science. Retrieved 2014-01-07.
- PMID 117984.
- PMID 22855752.
- ^ Neil DM (January 17, 2012). "For Intrigue, Malaria Drug Gets the Prize". New York Times. Retrieved 20 April 2013.
- ^ "WHO calls for an immediate halt to provision of single-drug artemisinin malaria pills" (Press release). World Health Organization. January 19, 2006. Archived from the original on November 16, 2006.
- ^ Weise E (September 12, 2011). "'America's Nobel' awarded to Chinese scientist". USA Today. Retrieved 2011-09-12.
- ^ WHO 2015, p. 94.
- PMID 7324954.
- PMID 7115549. Archived from the originalon 2019-08-28. Retrieved 2017-04-30.
- PMID 16112072.
- PMID 29495461.
- S2CID 46753659.
- PMID 25960615.
Further reading
- Guidelines for the Treatment of Malaria (3 ed.). Geneva: OCLC 908628497.
- Talman AM, Clain J, Duval R, Ménard R, Ariey F (2019). "Artemisinin Bioactivity and Resistance in Malaria Parasites". Trends Parasitol. 35 (12): 953–63. PMID 31699532.
External links
 Media related to Artemisinin at Wikimedia Commons
Media related to Artemisinin at Wikimedia Commons- "Defeating the Curse". BBC Horizon.
Artemisinin has proven to be the most effective anti-malarial drug ever produced.
- "BBC World Service - Witness History, China's breakthrough malaria cure". BBC. 11 March 2019.
