Beta-lactam antibiotics
| β-lactam antibiotic | |
|---|---|
Penicillin binding protein | |
| External links | |
| MeSH | D047090 |
| Legal status | |
| In Wikidata | |
β-lactam antibiotics (beta-lactam antibiotics) are antibiotics that contain a beta-lactam ring in their chemical structure. This includes penicillin derivatives (penams), cephalosporins and cephamycins (cephems), monobactams, carbapenems[1] and carbacephems.[2] Most β-lactam antibiotics work by inhibiting cell wall biosynthesis in the bacterial organism and are the most widely used group of antibiotics. Until 2003, when measured by sales, more than half of all commercially available antibiotics in use were β-lactam compounds.[3] The first β-lactam antibiotic discovered, penicillin, was isolated from a strain of Penicillium rubens (named as Penicillium notatum at the time).[4][5]
Bacteria often develop resistance to β-lactam antibiotics by synthesizing a β-lactamase, an enzyme that attacks the β-lactam ring. To overcome this resistance, β-lactam antibiotics can be given with β-lactamase inhibitors such as clavulanic acid.[6]
Medical use
β-lactam antibiotics are indicated for the
In uninflamed (normal) brain meninges, the penetration of beta-lactam antibiotics is low, at 0.15 of AUCCSF/AUCS ratio (the ratio of area under curve of cerebrosopinal fluid against area under curve of serum).[7]
Adverse effects
Adverse drug reactions
Common
Infrequent
Pain and inflammation at the injection site is also common for parenterally administered β-lactam antibiotics.[citation needed]
Allergy/hypersensitivity
Immunologically mediated adverse reactions to any β-lactam antibiotic may occur in up to 10% of patients receiving that agent (a small fraction of which are truly IgE-mediated allergic reactions, see amoxicillin rash). Anaphylaxis will occur in approximately 0.01% of patients.[8][9] There is perhaps a 5–10% cross-sensitivity between penicillin-derivatives, cephalosporins, and carbapenems;[citation needed] but this figure has been challenged by various investigators.[who?][citation needed]
Nevertheless, the risk of cross-reactivity is sufficient to warrant the contraindication of all β-lactam antibiotics in patients with a history of severe allergic reactions (
A Jarisch–Herxheimer reaction may occur after initial treatment of a spirochetal infection such as syphilis with a β-lactam antibiotic.
Mechanism of action
Inhibition of cell wall synthesis

β-lactam antibiotics are
β-lactam antibiotics are analogues of d-alanyl-d-alanine—the terminal amino acid residues on the precursor NAM/NAG-peptide subunits of the nascent peptidoglycan layer. The structural similarity between β-lactam antibiotics and d-alanyl-d-alanine facilitates their binding to the active site of PBPs. The β-lactam nucleus of the molecule irreversibly binds to (acylates) the Ser403 residue of the PBP active site. This irreversible inhibition of the PBPs prevents the final crosslinking (transpeptidation) of the nascent peptidoglycan layer, disrupting cell wall synthesis.[13] β-lactam antibiotics block not only the division of bacteria, including
Under normal circumstances, peptidoglycan precursors signal a reorganisation of the bacterial cell wall and, as a consequence, trigger the activation of autolytic cell wall hydrolases. Inhibition of cross-linkage by β-lactams causes a build-up of peptidoglycan precursors, which triggers the digestion of existing peptidoglycan by autolytic hydrolases without the production of new peptidoglycan. As a result, the bactericidal action of β-lactam antibiotics is further enhanced.[citation needed]
Guanine oxidation
Another possibility that has been proposed to account for much of the cytotoxicity of beta lactams focuses on the oxidation of the
Potency
Two structural features of β-lactam antibiotics have been correlated with their antibiotic potency.
Modes of resistance
By definition, all β-lactam antibiotics have a β-lactam ring in their structure. The effectiveness of these antibiotics relies on their ability to reach the PBP intact and their ability to bind to the PBP. Hence, there are two main modes of bacterial resistance to β-lactams: enzymatic hydrolysis of the β-lactam ring and possession of altered penicillin-binding proteins.
Enzymatic hydrolysis of the β-lactam ring
If the bacterium produces the


The production of a β-lactamase by a bacterium does not necessarily rule out all treatment options with β-lactam antibiotics. In some instances, β-lactam antibiotics may be co-administered with a
Other β-lactamase inhibitors such as boronic acids are being studied in which they irreversibly bind to the active site of β-lactamases. This is a benefit over clavulanic acid and similar beta-lactam competitors, because they cannot be hydrolysed, and therefore rendered useless. Extensive research is currently being done to develop tailored boronic acids to target different isozymes of beta-lactamases.[21]
However, in all cases where infection with β-lactamase-producing bacteria is suspected, the choice of a suitable β-lactam antibiotic should be carefully considered prior to treatment. In particular, choosing appropriate β-lactam antibiotic therapy is of utmost importance against organisms which harbor some level of β-lactamase expression. In this case, failure to use the most appropriate β-lactam antibiotic therapy at the onset of treatment could result in selection for bacteria with higher levels of β-lactamase expression, thereby making further efforts with other β-lactam antibiotics more difficult.[22]
In the context of medical pharmacology, penicillins, cephalosporins, and carbapenems, while all have the β-lactam ring that serves as the fundamental structure, also have an auxiliary ring that carries a carboxylate group that is positioned on the same side as the carbonyl group within the β-lactam ring, and, as such, this structural configuration is critical to their antimicrobial activity.
Possession of altered penicillin-binding proteins
As a response to the use of β-lactams to control bacterial infections, some bacteria have evolved penicillin binding proteins with novel structures. β-lactam antibiotics cannot bind as effectively to these altered PBPs, and, as a result, the β-lactams are less effective at disrupting cell wall synthesis. Notable examples of this mode of resistance include methicillin-resistant Staphylococcus aureus (MRSA)[32] and penicillin-resistant Streptococcus pneumoniae. Altered PBPs do not necessarily rule out all treatment options with β-lactam antibiotics.[medical citation needed]
Nomenclature

β-lactams are classified according to their core ring structures.[33]
- β-lactams fused to saturated five-membered rings:
- β-lactams containing thiazolidine rings are named penams.
- β-lactams containing pyrrolidine rings are named carbapenams.
- β-lactams fused to oxazolidine rings are named oxapenams or clavams.
- β-lactams fused to unsaturated five-membered rings:
- β-lactams containing 2,3-dihydrothiazole rings are named penems.
- β-lactams containing 2,3-dihydro-1H-pyrrole rings are named carbapenems.
- β-lactams fused to unsaturated six-membered rings:
- β-lactams containing 3,6-dihydro-2H-1,3-thiazine rings are named cephems.
- β-lactams containing 1,2,3,4-tetrahydropyridine rings are named carbacephems.
- β-lactams containing 3,6-dihydro-2H-1,3-oxazine rings are named oxacephems.
- β-lactams not fused to any other ring are named monobactams.
By convention, the bicyclic β-lactams are numbered starting with the position occupied by sulfur in the penams and cephems, regardless of which atom it is in a given class. That is, position 1 is always adjacent to the β-carbon of β-lactam ring. The numbering continues clockwise from position one until the β-carbon of β-lactam is reached, at which point numbering continues counterclockwise around the lactam ring to number the remaining to carbons. For example, the nitrogen atom of all bicyclic β-lactams fused to five-membered rings is labelled position 4, as it is in penams, while in cephems, the nitrogen is position 5.[medical citation needed]
The numbering of monobactams follows that of the
Biosynthesis
To date, two distinct methods of biosynthesizing the β-lactam core of this family of antibiotics have been discovered. The first pathway discovered was that of the penams and cephems. This path begins with a nonribosomal peptide synthetase (NRPS), ACV synthetase (ACVS), which generates the linear tripeptide δ-(L-α-aminoadipyl)-L-cysteine-D-valine (ACV). ACV is oxidatively cyclized (two cyclizations by a single enzyme) to bicyclic intermediate isopenicillin N by isopenicillin N synthase (IPNS) to form the penam core structure.[34] Various transamidations lead to the different natural penicillins.
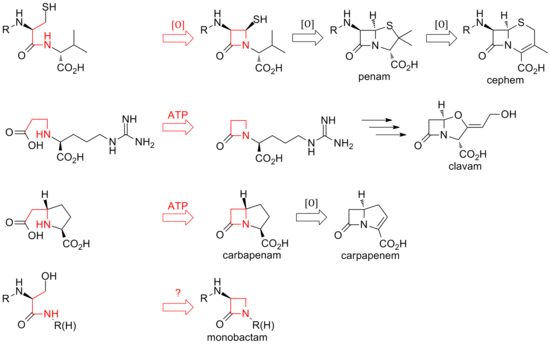
The biosynthesis of cephems branch off at isopenicillin N by an oxidative
While the ring closure in penams and cephems is between positions 1 and 4 of the β-lactam and is oxidative, the clavams and carbapenems have their rings closed by two-electron processes between positions 1 and 2 of the ring. β-lactam synthetases are responsible for these cyclizations, and the carboxylate of the open-ring substrates is activated by ATP.[35] In clavams, the β-lactam is formed prior to the second ring; in carbapenems, the β-lactam ring is closed second in sequence.[citation needed]
The biosynthesis of the β-lactam ring of tabtoxin mirrors that of the clavams and carbapenems. The closure of the lactam ring in the other monobactams, such as sulfazecin and the nocardicins, may involve a third mechanism involving inversion of configuration at the β-carbon.[36]
See also
- List of β-lactam antibiotics
- ATC code J01C Beta-lactam antibacterials, penicillins
- ATC code J01D Other beta-lactam antibacterials
- Bacteria
- Cell wall
- Discovery and development of cephalosporins
- History of penicillin
- Nitrocefin
References
- PMID 10950216. Archived from the originalon June 6, 2011. Retrieved November 8, 2008.
- ^ Yao, JDC, Moellering, RC Jr. (2007). "Antibacterial agents". In Murray, PR, et al. (eds.). Manual of Clinical Microbiology (9th ed.). Washington D.C.: ASM Press. Cited in Non-Penicillin Beta Lactam Drugs: A CGMP Framework for Preventing Cross-Contamination (Report). U.S. Department of Health and Human Services; Food and Drug Administration; Center for Drug Evaluation and Research (CDER). April 2013. Archived from the original on December 13, 2019. Retrieved May 27, 2019 – via US FDA website.
- S2CID 43996071.
- PMID 22679592.
- PMID 32973216.
- ^ from the original on December 15, 2020. Retrieved May 5, 2020.
- PMID 20930076.
- ^ ISBN 0-9578521-4-2.
- ^
Pichichero ME (April 2005). "A review of evidence supporting the American Academy of Pediatrics recommendation for prescribing cephalosporin antibiotics for penicillin-allergic patients". S2CID 21246804.
- from the original on April 25, 2023. Retrieved February 27, 2021.
- ^ S2CID 210814189.
- from the original on October 7, 2017. Retrieved May 5, 2020.
- PMID 15700950.
- .
- ^ PMID 22517853.
- ^ ISSN 1364-5471.
- PMID 6109320.
- PMID 6827544.
- PMID 20065329.
- S2CID 68837323.
- PMID 23902256.
- PMID 22477821.
- PMID 36788654.
- PMID 35563620.
- ^ "Archived copy" (PDF). Archived (PDF) from the original on February 16, 2022. Retrieved February 22, 2024.
{{cite web}}: CS1 maint: archived copy as title (link) - ISBN 978-0-7020-3468-8.
- ^ a b "Archived copy". Archived from the original on February 22, 2024. Retrieved February 22, 2024.
{{cite web}}: CS1 maint: archived copy as title (link) - ^ PMID 23163348.
- ^ from the original on February 27, 2024. Retrieved February 22, 2024.
- ^ "Ceftriaxone: Package Insert". Archived from the original on April 2, 2023.
- ^ https://web.archive.org/web/20240222172948/https://www.accessdata.fda.gov/drugsatfda_docs/label/2009/0550585s063lbl.pdf
- PMID 2708325.
- PMID 16413506.
- from the original on September 22, 2017. Retrieved October 28, 2017.
- PMID 9689037.
- .


