Brain tumor
| Brain tumor | |
|---|---|
| Other names | Intracranial neoplasm, brain tumour |
five-year survival rate 33% (US)[4] | |
| Frequency | 1.2 million nervous system cancers (2015)[5] |
| Deaths | 228,800 (worldwide, 2015)[6] |
A brain tumor occurs when abnormal cells form within the
The cause of most brain tumors is unknown, though up to 4% of brain cancers may be caused by CT scan radiation.
Treatment may include some combination of surgery, radiation therapy and chemotherapy.[1] If seizures occur, anticonvulsant medication may be needed.[1] Dexamethasone and furosemide are medications that may be used to decrease swelling around the tumor.[1] Some tumors grow gradually, requiring only monitoring and possibly needing no further intervention.[1] Treatments that use a person's immune system are being studied.[2] Outcomes for malignant tumors vary considerably depending on the type of tumor and how far it has spread at diagnosis.[3] Although benign tumors only grow in one area, they may still be life-threatening depending on their size and location.[9] Malignant glioblastomas usually have very poor outcomes, while benign meningiomas usually have good outcomes.[3] The average five-year survival rate for all (malignant) brain cancers in the United States is 33%.[4]
Secondary, or
Signs and symptoms
The signs and symptoms of brain tumors are broad. People may experience symptoms regardless of whether the tumor is benign (not cancerous) or cancerous.[13] Primary and secondary brain tumors present with similar symptoms, depending on the location, size, and rate of growth of the tumor.[14] For example, larger tumors in the frontal lobe can cause changes in the ability to think. However, a smaller tumor in an area such as Wernicke's area (small area responsible for language comprehension) can result in a greater loss of function.[15]
Headaches
Headaches as a result of raised intracranial pressure can be an early symptom of brain cancer.[16] However, isolated headache without other symptoms is rare, and other symptoms including visual abnormalities may occur before headaches become common.[16] Certain warning signs for headache exist which make the headache more likely to be associated with brain cancer.[16] These are, as defined by the American Academy of Neurology: "abnormal neurological examination, headache worsened by Valsalva maneuver, headache causing awakening from sleep, new headache in the older population, progressively worsening headache, atypical headache features, or patients who do not fulfill the strict definition of migraine".[16] Other associated signs are headaches that are worse in the morning or that subside after vomiting.[17]
Location-specific symptoms
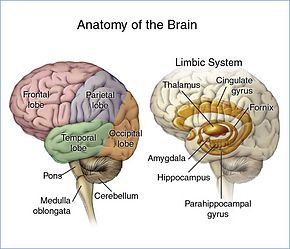
The brain is divided into lobes and each lobe or area has its own function.[18][19] A tumor in any of these lobes may affect the area's performance. The symptoms experienced are often linked to the location of the tumor, but each person may experience something different.[20]
- Frontal lobe: Tumors may contribute to poor reasoning, inappropriate social behavior, personality changes, poor planning, lower inhibition, and decreased production of speech (Broca's area).[20]
- Temporal lobe: Tumors in this lobe may contribute to poor memory, loss of hearing, and difficulty in language comprehension (Wernicke's area is located in this lobe).[19]
- Parietal lobe: Tumors here may result in poor interpretation of languages, difficulty with speaking, writing, drawing, naming, and recognizing, and poor spatial and visual perception.[21]
- Occipital lobe: Damage to this lobe may result in poor vision or loss of vision.[22]
- Cerebellum: Tumors in this area may cause poor balance, muscle movement, and posture.[23]
- Brain stem: Tumors on the brainstem can cause seizures, endocrine problems, respiratory changes, visual changes, headaches and partial paralysis.[23]
Behavior changes
A person's personality may be altered due to the tumor damaging lobes of the brain. Since the frontal, temporal, and parietal lobes[14] control inhibition, emotions, mood, judgement, reasoning, and behavior, a tumor in those regions can cause inappropriate social behavior,[24] temper tantrums,[24] laughing at things which merit no laughter,[24] and even psychological symptoms such as depression and anxiety.[20] More research is needed into the effectiveness and safety of medication for depression in people with brain tumors.[25]
Personality changes can have damaging effects such as unemployment, unstable relationships, and a lack of control.[18]
Cause
The best known cause of brain cancers is ionizing radiation.[8][26] Approximately 4% of brain cancers in the general population are caused by CT scan radiation.[8] For brain cancers that follow a CT scan at lags of 2 years or more, it has been estimated that 40% are attributable to CT scan radiation.[8] The relationship between ionizing radiation and brain cancers can be best explained by radiation carcinogenesis, and traditional models of oncogenesis. The stochastic effects of ionizing radiation demonstrate a dose-response relationship to the probability of occurrence, but no dose-response relationship to severity of disease. The majority of radiation-induced brain cancers are caused by ionizing radiation from medical sources such as CT scans.
Mutations and deletions of
Although studies have not shown any link between
Pathophysiology
Meninges

Human brains are surrounded by a system of
Tumors of the meninges are meningiomas and are often benign. Though not technically a tumor of brain tissue, they are often considered brain tumors since they protrude into the space where the brain is, causing symptoms. Since they are usually slow-growing tumors, meningiomas can be quite large by the time symptoms appear.[35]
Brain matter
The brains of humans and other
These areas are composed of two broad classes of cells:
The
] are often benign.The brainstem lies between the large cerebral cortex and the spinal cord. It is divided into the midbrain, pons, and medulla oblongata.[34]
Spinal cord
The spinal cord is considered a part of the central nervous system.[39] It is made up of the same cells as the brain: neurons and glial cells.[34]
Diagnosis

Although there is no specific or singular symptom or sign, the presence of a combination of symptoms and the lack of corresponding indications of other causes can be an indicator for investigation towards the possibility of a brain tumor. Brain tumors have similar characteristics and obstacles when it comes to diagnosis and therapy with tumors located elsewhere in the body. However, they create specific issues that follow closely to the properties of the organ they are in.[40]
The diagnosis will often start by taking a
Brain tumors, when compared to tumors in other areas of the body, pose a challenge for diagnosis. Commonly, radioactive tracers are uptaken in large volumes in tumors due to the high activity of tumor cells, allowing for radioactive imaging of the tumor. However, most of the brain is separated from the blood by the blood–brain barrier (BBB), a membrane that exerts a strict control over what substances are allowed to pass into the brain. Therefore, many tracers that may reach tumors in other areas of the body easily would be unable to reach brain tumors until there was a disruption of the BBB by the tumor. Disruption of the BBB is well imaged via MRI or CT scan, and is therefore regarded as the main diagnostic indicator for malignant gliomas, meningiomas, and brain metastases.[40]
Swelling or obstruction of the passage of
A bilateral temporal
Imaging

- Benign brain tumors often show up as hypodense (darker than brain tissue) mass lesions on CT scans. On MRI, they appear either hypodense or isointense (same intensity as brain tissue) on T2-weightedMRI, although the appearance is variable.
- Contrast agent uptake, sometimes in characteristic patterns, can be demonstrated on either CT or MRI scans in most malignant primary and metastatic brain tumors.
- Pressure areas where the brain tissue has been compressed by a tumor also appear hyperintense on T2-weighted scans and might indicate the presence of a diffuse neoplasm due to an unclear outline. Swelling around the tumor known as peritumoral edema can also show a similar result. This is because these tumors disrupt the normal functioning of the BBB and lead to an increase in its permeability.
More recently, advancements have been made to increase the utility of MRI in providing physiological data that can help to inform diagnosis and prognosis. MRI itself is sufficient in identifying the brain tumor's location and morphology, but other types of MRI may be used on top of that, such as MRA, MRS, pMRI, fMRI, and DWI. These imaging techniques help doctors and surgeons to diagnose the type of tumor, to plan for surgery, and to assess treatment and radiation/chemotherapy. Treatment with radiation and chemotherapy can lead to treatment induced changes in the brain, visible on conventional imaging and which can be difficult to differentiate from tumor recurrence.[43]
Different Types of MRI Scans
Magnetic Resonance Angiography (MRA) – looks at the blood vessels in the brain. In the diagnosis of brain tumor, MRAs are typically carried out before surgery to help surgeons get a better understanding of the tumor vasculature. For example, a study was done where surgeons were able to separate benign brain tumors from malignant ones by analyzing the shapes of the blood vessels that were extracted from MRA.[44] Although not required, some MRA may inject contrast agent, gadolinium, into the patient to get an enhanced image
Magnetic Resonance Spectroscopy (MRS) – measures the metabolic changes or chemical changes inside the tumor. The most common MRS is proton spectroscopy with its frequency measured in parts per million (ppm). Gliomas or malignant brain tumors have different spectra from normal brain tissue in that they have greater choline levels and lower N-acetyl aspartate (NAA) signals.[45] Using MRS in brain tumor diagnosis can help doctors identify the type of tumor and its aggressiveness. For example, benign brain tumors or meningioma have increased alanine levels. It can also help to distinguish brain tumors from scar tissues or dead tissues caused by previous radiation treatment, which does not have increased choline levels[46] that brain tumors have, and from tumor-mimicking lesions such as abscesses or infarcts.
Perfusion Magnetic Resonance Imaging (pMRI) – assess the blood volume and blood flow of different parts of the brain and brain tumors. pMRI requires the injection of contrast agent, usually gadopentetate dimeglumine (Gd-DTPA) into the veins in order to enhance the contrast. pMRI provides a cerebral blood volume map that shows the tumor vascularity and angiogenesis. Brain tumors would require a larger blood supply and thus, would show a high cerebral blood volume on the pMRI map. The vascular morphology and degree of angiogenesis from pMRI help to determine the grade and malignancy of brain tumors. For brain tumor diagnosis, pMRI is useful in determining the best site to perform biopsy and to help reduce sampling error. pMRI is also valuable for after treatment to determine if the abnormal area is a remaining tumor or a scar tissue. For patients that are undergoing anti-angiogenesis cancer therapy, pMRI can give the doctors a better sense of efficacy of the treatment by monitoring tumor cerebral blood volume.[47]
Functional MRI (fMRI) – measures blood flow changes in active parts of the brain while the patient is performing tasks and provides specific locations of the brain that are responsible for certain functions. Before performing a brain tumor surgery on patients, neurosurgeons would use fMRI to avoid damage to structures of the brain that correspond with important brain functions while resecting the tumor at the same time. Preoperative fMRI is important because it is often difficult to distinguish the anatomy near the tumor as it distorts its surrounding regions. Neurosurgeons would use fMRI to plan whether to perform a resection where tumor is surgically removed as much as possible, a biopsy where they take a surgical sampling amount to provide a diagnosis, or to not undergo surgery at all. For example, a neurosurgeon may be opposed to resecting a tumor near the motor cortex as that would affect the patient's movements. Without preoperative fMRI, the neurosurgeon would have to perform an awake-craniotomy where the patient would have to interact during open surgery to see if tumor removal would affect important brain functions.[48]
Diffusion Weighted Imaging (DWI) – a form of MRI that measures random Brownian motion of water molecules along a magnetic field gradient. For brain tumor diagnosis, measurement of apparent diffusion coefficient (ADC) in brain tumors allow doctors to categorize tumor type. Most brain tumors have higher ADC than normal brain tissues and doctors can match the observed ADC of the patient's brain tumor with a list of accepted ADC to identify tumor type. DWI is also useful for treatment and therapy purposes where changes in diffusion can be analyzed in response to drug, radiation, or gene therapy. Successful response results in apoptosis and increase in diffusion while failed treatment results in unchanged diffusion values.[49]
Other Types of Imaging Techniques
Computed Tomography (CT) Scan – uses x-rays to take pictures from different angles and computer processing to combine the pictures into a 3D image. A CT scan usually serves as an alternative to MRI in cases where the patient cannot have an MRI due to claustrophobia or pacemaker. Compared to MRI, a CT scan shows a more detailed image of the bone structures near the tumor and can be used to measure the tumor's size.[50] Like an MRI, a contrast dye may also be injected into the veins or ingested by mouth before a CT scan to better outline any tumors that may be present. CT scans use contrast materials that are iodine-based and barium sulfate compounds. The downside of using CT scans as opposed to MRI is that some brain tumors do not show up well on CT scans because some intra-axial masses are faint and resemble normal brain tissue. In some scenarios, brain tumors in CT scans may be mistaken for infarction, infection, and demyelination. To suspect that an intra-axial mass is a brain tumor instead of other possibilities, there must be unexplained calcifications in the brain, preservation of the cortex, and disproportionate mass effect.[51]
CT Angiography (CTA) – provides information about the blood vessels in the brain using X-rays. A contrast agent is always required to be injected into the patient in the CT scanner. CTA serves as an alternative to MRA.
Positron Emission Tomography (PET) Scan – uses radioactive substances, with the most common one being a sugar known as FDG, while more specific tracers for glioma are emerging.[52] This injected substance is taken up by cells that are actively dividing. Tumor cells are more active in dividing so they would absorb more of the radioactive substance. After injection, a scanner would be used to create an image of the radioactive areas in the brain. PET scans are used more often for high-grade tumors than for low-grade tumors. It is useful after treatment to help doctors determine if the abnormal area on an MRI image is a remaining tumor or a scar tissue. Scar tissues will not show up on PET scans while tumors would.[50]
However, these techniques cannot alone diagnose high- versus low-grade gliomas, and thus the definitive
Pathology

Tumors have characteristics that allow the determination of malignancy and how they will evolve, and determining these characteristics will allow the medical team to determine the management plan.[citation needed]
Anaplasia or dedifferentiation: loss of differentiation of cells and of their orientation to one another and blood vessels, a characteristic of anaplastic tumor tissue. Anaplastic cells have lost total control of their normal functions and many have deteriorated cell structures. Anaplastic cells often have abnormally high nuclear-to-cytoplasmic ratios, and many are multinucleated. Additionally, the nucleus of anaplastic cells is usually unnaturally shaped or oversized. Cells can become anaplastic in two ways: neoplastic tumor cells can dedifferentiate to become anaplasias (the dedifferentiation causes the cells to lose all of their normal structure/function), or cancer stem cells can increase their capacity to multiply (i.e., uncontrollable growth due to failure of differentiation).[citation needed]
Atypia: an indication of abnormality of a cell (which may be indicative of malignancy). Significance of the abnormality is highly dependent on context.[53]
Necrosis: the (premature) death of cells, caused by external factors such as infection, toxin or trauma. Necrotic cells send the wrong chemical signals which prevent phagocytes from disposing of the dead cells, leading to a buildup of dead tissue, cell debris and toxins at or near the site of the necrotic cells[54]
Arterial and venous
Classification
Tumors can be
Grading of the tumors of the central nervous system commonly occurs on a 4-point scale (I-IV) created by the World Health Organization in 1993. Grade I tumors are the least severe and commonly associated with long-term survival, with severity and prognosis worsening as the grade increases. Low-grade tumors are often benign, while higher grades are aggressively malignant and/or metastatic. Other grading scales do exist, many based upon the same criteria as the WHO scale and graded from I-IV.[58]
Primary

The most common primary brain tumors are:[59]
These common tumors can also be organized according to tissue of origin as shown below:[61]
|
Tissue of origin |
Children | Adults |
|---|---|---|
Astrocytes |
Pilocytic Astrocytoma (PCA) | Glioblastoma |
Oligodendrocytes |
Oligodendroglioma | |
| Ependyma | Ependymoma | |
Neurons |
Medulloblastoma | |
| Meninges | Meningioma |
Secondary
Secondary tumors of the brain are
Secondary brain tumors are more common than primary ones; in the United States, there are about 170,000 new cases every year. Secondary brain tumors are the most common cause of tumors in the intracranial cavity. The
By behavior
Brain tumors or intracranial neoplasms can be
- uncontrolled mitosis (growth by division beyond the normal limits)
- Giant cells – considerably larger than their neighbors – may form and possess either one enormous nucleus or several nuclei (syncytia). Anaplastic nuclei are variable and bizarre in size and shape.
- invasion or infiltration (medical literature uses these terms as synonymous equivalents. However, for clarity, the articles that follow adhere to a convention that they mean slightly different things; this convention is not followed outside these articles):
- Invasion or invasiveness is the spatial expansion of the tumor through uncontrolled mitosis, in the sense that the neoplasm invades the space occupied by adjacent tissue, thereby pushing the other tissue aside and eventually compressing the tissue. Often these tumors are associated with clearly outlined tumors in imaging.
- Infiltration is the behavior of the tumor either to grow (microscopic) tentacles that push into the surrounding tissue (often making the outline of the tumor undefined or diffuse) or to have tumor cells "seeded" into the tissue beyond the circumference of the tumorous mass; this does not mean that an infiltrative tumor does not take up space or does not compress the surrounding tissue as it grows, but an infiltrating neoplasm makes it difficult to say where the tumor ends and the healthy tissue starts.
- metastasis (spread to other locations in the body via lymph or blood).
Of the above malignant characteristics, some elements do not apply to primary neoplasms of the brain:
- Primary brain tumors rarely metastasize to other organs; some forms of primary brain tumors can metastasize but will not spread outside the intracranial cavity or the central spinal canal. Due to the BBB, cancerous cells of a primary neoplasm cannot enter the bloodstream and get carried to another location in the body. (Occasional isolated case reports suggest spread of certain brain tumors outside the central nervous system, e.g. bone metastasis of glioblastoma.[64])
- Primary brain tumors generally are invasive (i.e. they will expand spatially and intrude into the space occupied by other brain tissue and compress those brain tissues); however, some of the more malignant primary brain tumors will infiltrate the surrounding tissue.
By genetics
In 2016, the WHO restructured their classifications of some categories of
- Mutations in IDH1 and IDH2 genes are commonly found in low-grade gliomas
- Loss of both IDH genes combined with loss of chromosome arms 1p and 19q indicates the tumor is an oligodendroglioma[65]
- Loss of TP53 and ATRX characterizes astrocytomas
- Genes EGFR, TERT, and PTEN, are commonly altered in gliomas and are useful in differentiating tumor grade and biology[42]
Specific types
Treatment
A medical team generally assesses the treatment options and presents them to the person affected and their family. Various types of treatment are available depending on tumor type and location, and may be combined to produce the best chances of survival:[60]
- Surgery:resectionof the tumor with the objective of removing as many tumor cells as possible.
- Radiotherapy:[60] the most commonly used treatment for brain tumors; the tumor is irradiated with beta, x rays or gamma rays.
- Chemotherapy:[60] a treatment option for cancer, however, it is not always used to treat brain tumors as the blood–brain barrier can prevent some drugs from reaching the cancerous cells.
- A variety of experimental therapies are available through clinical trials.
Survival rates in primary brain tumors depend on the type of tumor, age, functional status of the patient, the extent of surgical removal and other factors specific to each case.[66]
Standard care for anaplastic oligodendrogliomas and anaplastic oligoastrocytomas is surgery followed by radiotherapy. One study found a survival benefit for the addition of chemotherapy to radiotherapy after surgery, compared with radiotherapy alone.[67]
Surgery
The primary and most desired course of action described in medical literature is surgical removal (resection) via
Many
Several current research studies aim to improve the surgical removal of brain tumors by labeling tumor cells with 5-aminolevulinic acid that causes them to fluoresce.[71] Postoperative radiotherapy and chemotherapy are integral parts of the therapeutic standard for malignant tumors.[72][73]
Multiple metastatic tumors are generally treated with radiotherapy and chemotherapy rather than surgery and the prognosis in such cases is determined by the primary tumor, and is generally poor.
Radiation therapy
The goal of radiation therapy is to kill tumor cells while leaving normal brain tissue unharmed. In standard
People who receive stereotactic radiosurgery (SRS) and whole-brain radiation therapy (WBRT) for the treatment of metastatic brain tumors have more than twice the risk of developing learning and memory problems than those treated with SRS alone.[76][77] Results of a 2021 systematic review found that when using SRS as the initial treatment, survival or death related to brain metastasis was not greater than alone versus SRS with WBRT.[78]
Postoperative conventional daily radiotherapy improves survival for adults with good functional well-being and high grade glioma compared to no postoperative radiotherapy. Hypofractionated radiation therapy has similar efficacy for survival as compared to conventional radiotherapy, particularly for individuals aged 60 and older with glioblastoma.[79]
Chemotherapy
Patients undergoing
UCLA Neuro-Oncology publishes real-time survival data for patients with a diagnosis of glioblastoma. They are the only institution in the United States that displays how brain tumor patients are performing on current therapies. They also show a listing of chemotherapy agents used to treat high-grade glioma tumors.[81]
Genetic mutations have significant effects on the effectiveness of chemotherapy. Gliomas with IDH1 or IDH2 mutations respond better to chemotherapy than those without the mutation. Loss of chromosome arms 1p and 19q also indicate better response to chemoradiation.[42]
Other
A shunt may be used to relieve symptoms caused by intracranial pressure, by reducing the build-up of fluid (hydrocephalus) caused by the blockage of the free flow of cerebrospinal fluid.[82]
Prognosis
The prognosis of brain cancer depends on the type of cancer diagnosed. Medulloblastoma has a good prognosis with chemotherapy, radiotherapy, and surgical resection while glioblastoma has a median survival of only 15 months even with aggressive chemoradiotherapy and surgery.[83] Brainstem gliomas have the poorest prognosis of any form of brain cancer, with most patients dying within one year, even with therapy that typically consists of radiation to the tumor along with corticosteroids. However, one type, focal brainstem gliomas in children, seems open to exceptional prognosis and long-term survival has frequently been reported.[84]
Prognosis is also affected by presentation of genetic mutations. Certain mutations provide better prognosis than others. IDH1 and IDH2 mutations in gliomas, as well as deletion of chromosome arms 1p and 19q, generally indicate better prognosis. TP53, ATRX, EGFR, PTEN, and TERT mutations are also useful in determining prognosis.[42]
Glioblastoma
Oligodendrogliomas
Acoustic neuroma
Acoustic neuromas are non-cancerous tumors.[91] They can be treated with surgery, radiation therapy, or observation. Early intervention with surgery or radiation is recommended to prevent progressive hearing loss.[92]
Epidemiology
Figures for incidences of cancers of the brain show a significant difference between more- and less-developed countries (the less-developed countries have lower incidences of tumors of the brain).[93] This could be explained by undiagnosed tumor-related deaths (patients in extremely poor situations do not get diagnosed, simply because they do not have access to the modern diagnostic facilities required to diagnose a brain tumor) and by deaths caused by other poverty-related causes that preempt a patient's life before tumors develop or tumors become life-threatening. Nevertheless, statistics suggest that certain forms of primary brain tumors are more common among certain populations.[94]
The incidence of low-grade astrocytoma has not been shown to vary significantly with nationality. However, studies examining the incidence of malignant central nervous system (CNS) tumors have shown some variation with national origin. Since some high-grade lesions arise from low-grade tumors, these trends are worth mentioning. Specifically, the incidence of CNS tumors in the United States, Israel, and the Nordic countries is relatively high, while Japan and Asian countries have a lower incidence. These differences probably reflect some biological differences as well as differences in pathologic diagnosis and reporting.[95] Worldwide data on incidence of cancer can be found at the
United States
In the United States in 2015, approximately 166,039 people were living with brain or other central nervous system tumors. Over 2018, it was projected that there would be 23,880 new cases of brain tumors and 16,830 deaths in 2018 as a result,[94] accounting for 1.4 percent of all cancers and 2.8 percent of all cancer deaths.[97] Median age of diagnosis was 58 years old, while median age of death was 65. Diagnosis was slightly more common in males, at approximately 7.5 cases per 100 000 people, while females saw 2 fewer at 5.4. Deaths as a result of brain cancer were 5.3 per 100 000 for males, and 3.6 per 100 000 for females, making brain cancer the 10th leading cause of cancer death in the United States. Overall lifetime risk of developing brain cancer is approximated at 0.6 percent for men and women.[94][98]
UK
Brain, other CNS or intracranial tumors are the ninth most common cancer in the UK (around 10,600 people were diagnosed in 2013), and it is the eighth most common cause of cancer death (around 5,200 people died in 2012).[99] White British patients with brain tumour are 30% more likely to die within a year of diagnosis than patients from other ethnicities. The reason for this is unknown.[100]
Children
In the United States more than 28,000 people under 20 are estimated to have a brain tumor.[101] About 3,720 new cases of brain tumors are expected to be diagnosed in those under 15 in 2019.[102] Higher rates were reported in 1985–1994 than in 1975–1983. There is some debate as to the reasons; one theory is that the trend is the result of improved diagnosis and reporting, since the jump occurred at the same time that MRIs became available widely, and there was no coincident jump in mortality. Central nervous system tumors make up 20–25 percent of cancers in children.[103][97][104]
The average survival rate for all primary brain cancers in children is 74%.[101] Brain cancers are the most common cancer in children under 19, are result in more death in this group than leukemia.[105] Younger people do less well.[106]
The most common brain tumor types in children (0–14) are: pilocytic astrocytoma, malignant glioma, medulloblastoma, neuronal and mixed neuronal-glial tumors, and ependymoma.[107]
In children under 2, about 70% of brain tumors are
In the UK, 429 children aged 14 and under are diagnosed with a brain tumour on average each year, and 563 children and young people under the age of 19 are diagnosed.[110]
Research
Immunotherapy
Cancer immunotherapy is being actively studied. For malignant gliomas no therapy has been shown to improve life expectancy as of 2015.[111]
Vesicular stomatitis virus
In 2000, researchers used the
Retroviral replicating vectors
Led by Prof. Nori Kasahara, researchers from
Non-invasive detection
Efforts to detect and monitor development and treatment response of brain tumors by liquid biopsy from blood, cerebrospinal fluid or urine, are in the early stages of development.[117][118]
See also
- Brain
- Tumor
- Nervous system neoplasm
- List of brain tumor cases
References
- ^ a b c d e f g h i j k l m n o p "Adult Brain Tumors Treatment". NCI. 28 February 2014. Archived from the original on 5 July 2014. Retrieved 8 June 2014.
- ^ a b c d e f g h i j k l m n o "General Information About Adult Brain Tumors". NCI. 14 April 2014. Archived from the original on 5 July 2014. Retrieved 8 June 2014.
- ^ ISBN 978-92-832-0429-9. Archivedfrom the original on 19 September 2016.
- ^ a b "Cancer of the Brain and Other Nervous System – Cancer Stat Facts". SEER. Retrieved 22 July 2019.
- PMID 27733282.
- PMID 27733281.
- ISBN 978-0-07-174887-2.
- ^ a b c d Smoll NR, Brady Z, Scurrah KJ, Lee C, Berrington de González A, Mathews JD. Computed tomography scan radiation and brain cancer incidence. Neuro-Oncology. 2023 Jan 14;https://doi.org/10.1093/neuonc/noad012
- ^ "Benign brain tumour (non-cancerous)". nhs.uk. 20 October 2017. Retrieved 29 July 2019.
- ^ PMID 23149521.
- ISBN 978-92-832-0429-9.
- ^ "Brain Tumour Facts 2011" (PDF). Brain Tumour Alliance Australia. Archived from the original (PDF) on 25 January 2014. Retrieved 9 June 2014.
- ^ "Brain Tumors". Archived from the original on 12 August 2016. Retrieved 2 August 2016.
- ^ a b "Mood Swings and Cognitive Changes | American Brain Tumor Association". abta.org. Archived from the original on 2 August 2016. Retrieved 3 August 2016.
- ^ "Coping With Personality & Behavioral Changes". brainsciencefoundation.org. Archived from the original on 30 July 2016. Retrieved 3 August 2016.
- ^ S2CID 5820118.
- ^ "Nosebleeds & Headaches: Do You Have Brain Cancer?". Advanced Neurosurgery Associates. 19 November 2020. Retrieved 26 November 2020.
- ^ S2CID 2072277.
- ^ a b "Coping With Personality & Behavioral Changes". brainsciencefoundation.org. Archived from the original on 30 July 2016. Retrieved 27 July 2016.
- ^ a b c "Mood Swings and Cognitive Changes | American Brain Tumor Association". abta.org. Archived from the original on 15 August 2016. Retrieved 27 July 2016.
- ^ Warnick R (August 2018). "Brain Tumors: an introduction". Mayfield Brain and Spine Clinic.
- ^ "Changes in Vision – Brain Tumour Symptoms". thebraintumourcharity.org. Archived from the original on 10 February 2018. Retrieved 9 February 2018.
- ^ a b "Brain Tumors". Children's Hospital of Wisconsin. 6 March 2019.
- ^ a b c Jones C. "Brain Tumor Symptoms | Miles for Hope | Brain Tumor Foundation". milesforhope.org. Archived from the original on 14 August 2016. Retrieved 3 August 2016.
- PMID 32678464.
- ^ Smoll NR, Brady Z, Scurrah K, Mathews JD. Exposure to ionizing radiation and brain cancer incidence: The Life Span Study cohort. Cancer Epidemiology. 2016 Jun;42:60–5.
- ISBN 978-3-540-57351-7.
- S2CID 29232748.
- PMID 25343186.
- S2CID 12795861.
- ^ "Brain Cancer Causes, Symptoms, Stages & Life Expectancy". MedicineNet. Retrieved 24 February 2020.
- PMID 22016439.
- ^ "IARC classifies radiofrequency electromagnetic fields as possibly carcinogenic to humans" (PDF). World Health Organization press release N° 208 (Press release). International Agency for Research on Cancer. 31 May 2011. Archived (PDF) from the original on 1 June 2011. Retrieved 2 June 2011.
- ^ OCLC 978362025.
- ^ "Meningioma Brain Tumor". neurosurgery.ucla.edu. Retrieved 29 July 2019.
- ^ "Neurons & Glial Cells | SEER Training". training.seer.cancer.gov. Retrieved 29 July 2019.
- PMID 24137015.
- ^ "Pituitary tumours". www.cancerresearchuk.org. Archived from the original on 1 March 2024. Retrieved 18 April 2024.
- ^ a b "Adult Central Nervous System Tumors Treatment (PDQ®)–Patient Version – National Cancer Institute". cancer.gov. 11 May 2020. Retrieved 29 January 2021.
- ^ PMID 23026359.
- S2CID 37522684.
- ^ PMID 29405955.
- S2CID 221674217– via Elsevier.
- ISBN 978-3-540-22977-3.
- PMID 20708548.
- ^ "MRI (magnetic resonance imaging)". mayfieldclinic.com. Retrieved 28 November 2022.
- S2CID 25773559.
- S2CID 45995537.
- PMID 20886568.
- ^ a b "Tests for Brain and Spinal Cord Tumors in Adults". cancer.org. Retrieved 28 November 2022.
- ^ "Recognizing intra-axial tumors on brain computed tomography (CT) | Medmastery". public-nuxt.frontend.prod.medmastery.io. Retrieved 28 November 2022.
- PMID 36215231.
- ^ Watson AN (1 January 2007). "Significance of "Atypia" Found on Needle Biopsy of the Breast: Correlation with Surgical Outcome". Yale Medicine Thesis Digital Library.
- ^ MedlinePlus Encyclopedia: Necrosis
- PMID 33472628.
- ISBN 81-250-2695-9.
- ^ "What you need to know about brain tumors". National Cancer Institute. Archived from the original on 27 January 2012. Retrieved 25 February 2012.
- PMID 29204027.
- ISBN 978-1-84882-910-7.
- ^ a b c d e f g h i "Brain Tumors – Classifications, Symptoms, Diagnosis and Treatments". aans.org. Retrieved 29 January 2021.
- ^ "Classifications of Brain Tumors". AANS. American Association of Neurological Surgeons. Archived from the original on 24 April 2017. Retrieved 23 April 2017.
- ^ MedlinePlus Encyclopedia: Metastatic brain tumor
- PMID 34185076.
- S2CID 40327650.
- ^ "Oligodendroglioma". The Lecturio Medical Concept Library. Retrieved 21 August 2021.
- PMID 8545771.
- PMID 24833028.
- PMID 21981642.
- ^ "Brain & Spinal Tumors: Surgery & Recovery | Advanced Neurosurgery". Advanced Neurosurgery Associates. Retrieved 8 October 2020.
- PMID 31149219.
- ^ Brennan P (4 August 2008). "Introduction to brain cancer". cliniclog.com. Archived from the original on 17 February 2012. Retrieved 19 December 2011.
- S2CID 246623373.
- PMID 11150363.
- ^ "Radiosurgery treatment comparisons – Cyberknife, Gamma knife, Novalis Tx". Archived from the original on 20 May 2007. Retrieved 22 July 2014.
- ^ "Treating secondary brain tumours with WBRT". Cancer Research UK. Archived from the original on 25 October 2007. Retrieved 5 June 2012.
- ^ "Whole Brain Radiation increases risk of learning and memory problems in cancer patients with brain metastases". MD Anderson Cancer Center. Archived from the original on 5 October 2008. Retrieved 5 June 2012.
- ^ "Metastatic brain tumors". International RadioSurgery Association. Archived from the original on 16 June 2012. Retrieved 5 June 2012.
- S2CID 236256085.
- PMID 32437039.
- PMID 26926614.
- ^ "How Our Patients Perform: Glioblastoma Multiforme". UCLA Neuro-Oncology Program. Archived from the original on 9 June 2012. Retrieved 5 June 2012.
- ^ Dalvi A. "Normal Pressure Hydrocephalus Causes, Symptoms, Treatment". eMedicineHealth. Emedicinehealth.com. Archived from the original on 22 February 2012. Retrieved 17 February 2012.
- ^ ISBN 978-92-832-4508-7.
- ^ "Brain Stem Gliomas in Childhood". Childhoodbraintumor.org. Archived from the original on 9 March 2012. Retrieved 17 February 2012.
- PMID 28840962.
- ^ "GBM Guide – MGH Brain Tumor Center". Brain.mgh.harvard.edu. Archived from the original on 16 February 2012. Retrieved 17 February 2012.
- PMID 17981778. Archived from the original(PDF) on 19 March 2012.
- PMID 23246627.
- from the original on 20 July 2008.
- ^ "Neurology". Neurology. Archived from the original on 19 February 2012. Retrieved 17 February 2012.
- ^ "Acoustic Neuroma (Vestibular Schwannoma)". hopkinsmedicine.org. Retrieved 19 July 2019.
- ^ "UpToDate". uptodate.com. Retrieved 19 July 2019.
- PMID 18798534.
- ^ a b c "Cancer Stat Facts: Brain and Other Nervous System Cancer". National Cancer Institute. 31 March 2019.
- ^ Jallo GI, Benardete EA (January 2010). "Low-Grade Astrocytoma". Archived from the original on 27 July 2010.
- ^ "CANCERMondial". International Agency for Research on Cancer. Archived from the original on 17 February 2012. Retrieved 17 February 2012.
- ^ a b "What are the key statistics about brain and spinal cord tumors?". American Cancer Society. 1 May 2012. Archived from the original on 2 July 2012.
- ^ "2018 CBTRUS Fact Sheet". Central Brain Tumor Registry of the United States. 31 March 2019. Archived from the original on 14 February 2019. Retrieved 14 February 2019.
- ^ "Brain, other CNS and intracranial tumours statistics". Cancer Research UK. Archived from the original on 16 October 2014. Retrieved 27 October 2014.
- ^ White British brain tumour patients 'more likely to die in a year' The Guardian
- ^ a b "Quick Brain Tumor Facts". National Brain Tumor Society. Retrieved 14 February 2019.
- ^ "CBTRUS – 2018 CBTRUS Fact Sheet". cbtrus.org. Archived from the original on 14 February 2019. Retrieved 14 February 2019.
- .
- PMID 9499745.
- ^ "Childhood Brain Cancer Now Leads to More Deaths than Leukemia". Fortune. Retrieved 14 February 2019.
- ^ Gurney JG, Smith MA, Bunin GR. "CNS and Miscellaneous Intracranial and Intraspinal Neoplasms" (PDF). SEER Pediatric Monograph. National Cancer Institute. pp. 51–57. Archived (PDF) from the original on 17 December 2008. Retrieved 4 December 2008.
In the US, approximately 2,200 children and adolescents younger than 20 years of age are diagnosed with malignant central nervous system tumors each year. More than 90 percent of primary CNS malignancies in children are located within the brain.
- ^ "Ependymoma". The Lecturio Medical Concept Library. Retrieved 19 July 2021.
- ^ Rood BR. "Infantile Brain Tumors". The Childhood Brain Tumor Foundation. Archived from the original on 11 November 2012. Retrieved 23 July 2014.
- S2CID 8114229.
- ^ "About childhood brain tumours". Archived from the original on 7 August 2016. Retrieved 16 June 2016.
- PMID 25468230.
- PMID 22149027.
- PMID 16507823.
- PMID 11387057.
- PMID 16257382.
- ^ "A Study of a Retroviral Replicating Vector Administered to Subjects With Recurrent Malignant Glioma". Clinical Trials.gov. July 2014. Archived from the original on 26 November 2011.
- PMID 31614115.
- PMID 34771592.
External links
- Brain and CNS cancers at Curlie
- Brain tumour information from Cancer Research UK
- Neuro-Oncology: Cancer Management Guidelines
- MedPix Teaching File MR Scans of Primary Brain Lymphoma, etc.
