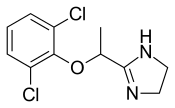
Lofexidine
 | |
| Clinical data | |
|---|---|
| Trade names | Britlofex, Lucemyra, Kai Er Ding, others |
| AHFS/Drugs.com | Monograph |
| Routes of administration | By mouth (tablets) |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | >90% |
| Protein binding | 80–90% |
| Metabolism | Liver (glucuronidation) |
| Elimination half-life | 11 hours |
| Excretion | Kidney |
| Identifiers | |
| |
JSmol) | |
| Chirality | Racemic mixture |
| |
| |
| | |
Lofexidine, sold under the brand name Lucemyra among others,
The U.S. Food and Drug Administration (FDA) considers it to be a first-in-class medication.[4]
Medical uses
In the United States, the brand name Lucemyra (lofexidine HCl) is approved for the "mitigation of withdrawal symptoms to facilitate abrupt discontinuation of opioids in adults," for a treatment duration of 14 days.[1] In the United Kingdom, lofexidine is commonly used in conjunction with the opioid receptor antagonist naltrexone in rapid detoxification cases. When these two drugs are paired, naltrexone is administered to induce an opioid-receptor blockade sending the subject into immediate withdrawal and accelerating the detoxification process, while lofexidine is given to relieve the symptoms associated with the withdrawal including chills, sweating, stomach cramps, muscle pain, and runny nose.[citation needed]
Opioid withdrawal
The United Kingdom's National Institute for Health and Care Excellence (NICE) guidelines recommend the use of methadone or buprenorphine as first-line agents in the management of opioid use disorder. However, lofexidine is considered an acceptable alternative for people with mild or uncertain opioid dependence in need of short-term detoxification.[5]
Lofexidine is not an opioid.[3] It does not eliminate the symptoms of opioid withdrawal but reduces them.[3] Indeed, one suggested use for lofexidine is to ease withdrawal symptoms of methadone dependence. Its use is approved in the United States for up to 14 days.[3]
Other clinical uses
The possibility of using lofexidine to treat
Special populations
Lofexidine's safety in pregnancy or in the setting of breastfeeding are unknown.[7] Caution is warranted if chronic kidney impairment is present.[7]
Adverse effects
Adverse effects that have occurred after taking lofexidine include the following:[7]
- Slow heart rate
- Dizziness
- Sleepiness
- Mouth dryness
- Low blood pressure
- QT prolongation
In addition, people may experience
Overdose
The LD50 of lofexidine is above 77 mg/kg in animals. Studies of high-dose, single administrations of lofexidine proved tolerable for animals, but repeat administration induced symptoms consistent with toxicity. In studies on mice, rats, and dogs, these included ataxia, somnolence, and tremors. It is expected that an overdose of lofexidine would result in symptoms akin to its pharmacological side effects in humans, such as bradycardia and hypotension.[8]
Interactions
Many drug-drug interactions with lofexidine are possible.[9]
QT prolongation
Lofexidine prolongs the
- increasing age
- female sex
- cardiac disease
- electrolyte disturbances (low blood potassium)
As a result, there are many QT-prolonging drugs that may interact with lofexidine. These include medications such as methadone, amiodarone, citalopram, and fluconazole. Other medications may increase the risk for a low level of potassium in the blood, thereby indirectly increasing the risk for QT prolongation. For example, dexamethasone, hydrochlorothiazide, and theophylline can lower the level of potassium in the blood.[9]
CNS depression
Lofexidine can depress the central nervous system (CNS), which, in combination with other CNS depressants, may reduce a person's ability to perform tasks that require skills and attention. For example, clobazam, gabapentin, and levetiracetam all can depress the CNS.[9]
Hypotension
The risk of hypotension (low blood pressure) is increased when lofexidine is combined with other drugs that lower blood pressure. These may include losartan, metoprolol, and pramipexole.[9]
Pharmacology
Lofexidine is an agonist at the α-2A, 2B, and 2C adrenergic receptor subtypes, with the highest activity at the α2A receptor.[10]
Ki for lofexidine[10] Adrenergic receptor Ki (nM) α2A 4 α2B 67 α2C 69
Ki represents the dissociation constant[11] for lofexidine's binding to a specific subtype of α2 receptor. The smaller the Ki value, the stronger the drug binds to the receptor to exert its activity.
Lofexidine inhibits the release of
Pharmacokinetics
Lofexidine's oral
Chemistry
Lofexidine exists as a solid at room temperature, with a
Comparison to clonidine

Lofexidine is structurally analogous to
Society and culture
Britannia Pharmaceuticals has licensed lofexidine to be sold by
See also
References
- ^ a b c d "Press Announcements - FDA approves the first non-opioid treatment for management of opioid withdrawal symptoms in adults". www.fda.gov. U.S. Food and Drug Administration. Retrieved 16 May 2018.
- ^ ISBN 978-0-85711-084-8.
- ^ a b c d e f "FDA approves the first non-opioid treatment for management of opioid withdrawal symptoms in adults". U.S. Food and Drug Administration (FDA) (Press release). Retrieved 18 May 2018.
- ^ New Drug Therapy Approvals 2018 (PDF). U.S. Food and Drug Administration (FDA) (Report). January 2019. Retrieved 16 September 2020.
- ^ "Pharmacological interventions in opioid detoxification for drug misuse in people over 16". pathways.nice.org.uk. NICE. Retrieved 16 May 2018.
- ^ Keaney F, Strang J, Gossop M, Marshall EJ, Farrell M, Welch S, Hahn B, Gonzalez A. A double-blind randomized placebo-controlled trial of lofexidine in alcohol withdrawal: lofexidine is not a useful adjunct to chlordiazepoxide. Alcohol Alcohol (2001) 36:426–30.
- ^ a b c "LOFEXIDINE HYDROCHLORIDE". bnf.nice.org.uk. NICE. Retrieved 16 May 2018.
- ^ a b c "Lofexidine". pubchem.ncbi.nlm.nih.gov. National Center for Biotechnology Information. Retrieved 16 May 2018.
- ^ a b c d e "Lofexidine | Interactions | BNF". bnf.nice.org.uk. NICE. Retrieved 16 May 2018.
- ^ ISBN 978-0470614167.
- S2CID 1729572.
- PMID 11516922.
- ^ Britannia Pharmaceuticals Limited
- ^ "Lucemyra (lofexidine hydrochloride) FDA Approval History - Drugs.com". Drugs.com. Retrieved 16 May 2018.
