Lead poisoning
| Lead poisoning | |
|---|---|
| Other names | Plumbism, colica pictorum, saturnism, |
| Deaths | 540,000 (2016)[2] |
Lead poisoning, also known as plumbism and saturnism, is a type of
Exposure to lead can occur by contaminated air, water, dust, food, or consumer products.[2] Lead poisoning poses a significantly increased risk to children as they are far more likely to ingest lead indirectly by chewing on toys or other objects that are coated in lead paint.[2] The amount of lead that can be absorbed by children is also higher than that of adults. Exposure at work is a common cause of lead poisoning in adults with certain occupations at particular risk.[7] Diagnosis is typically by measurement of the blood lead level.[2] The Centers for Disease Control and Prevention (US) has set the upper limit for blood lead for adults at 10 µg/dl (10 µg/100 g) and for children at 3.5 µg/dl,[8] previously before October 2021 5 µg/dl[9][10] Elevated lead may also be detected by changes in red blood cells or dense lines in the bones of children as seen on X-ray.[4]
Lead poisoning is preventable.
In 2013, lead is believed to have resulted in 853,000 deaths worldwide.
People have been mining and using lead for thousands of years.[4] Descriptions of lead poisoning date to at least 2000 BC,[4] while efforts to limit lead's use date back to at least the 16th century.[5] Concerns for low levels of exposure began in the 1970s with there being no safe threshold for lead exposure.[2][4][16]
Classification
Classically, "lead poisoning" or "lead intoxication" has been defined as exposure to high levels of lead typically associated with severe health effects.
The amount of lead in the blood and tissues, as well as the time course of exposure, determine toxicity.[19] Lead poisoning may be acute (from intense exposure of short duration) or chronic (from repeat low-level exposure over a prolonged period), but the latter is much more common.[20] Diagnosis and treatment of lead exposure are based on blood lead level (the amount of lead in the blood), measured in
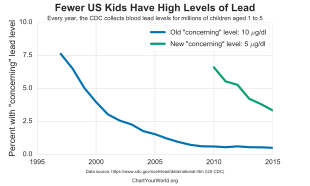
The US Centers for Disease Control and Prevention and the World Health Organization state that a blood lead level of 10 μg/dL or above is a cause for concern; however, lead may impair development and have harmful health effects even at lower levels, and there is no known safe exposure level.[22][23] Authorities such as the American Academy of Pediatrics define lead poisoning as blood lead levels higher than 10 μg/dL.[24]
Lead forms a variety of compounds and exists in the environment in various forms.
Signs and symptoms
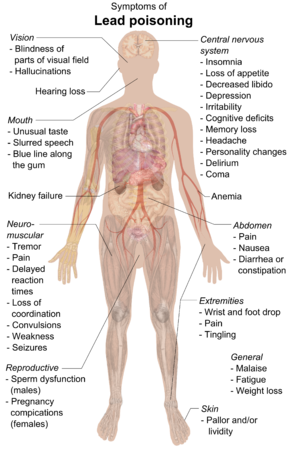
Lead poisoning can cause a variety of
Symptoms may be different in adults and children; the main symptoms in adults are headache,
Early symptoms of lead poisoning in adults are commonly nonspecific and include depression, loss of appetite, intermittent abdominal pain, nausea, diarrhea, constipation, and muscle pain.[33] Other early signs in adults include malaise, fatigue, decreased libido, and problems with sleep.[27] An unusual taste in the mouth and personality changes are also early signs.[34][35]
In adults, symptoms can occur at levels above 40 μg/dL, but are more likely to occur only above 50–60 μg/dL.
Acute poisoning
In acute poisoning, typical neurological signs are pain, muscle weakness,
Chronic poisoning
Chronic poisoning usually presents with symptoms affecting multiple systems,
Effects on children
A pregnant woman who has elevated blood lead levels is at greater risk of a premature birth or with a low birth weight.[44] Children are more at risk for lead poisoning because their smaller bodies are in a continuous state of growth and development.[45] Young children are much more vulnerable to lead poisoning, as they absorb 4 to 5 times more lead than an adult from a given source.[46] Furthermore, children, especially as they are learning to crawl and walk, are constantly on the floor and therefore more prone to ingesting and inhaling dust that is contaminated with lead.[47]
The classic signs and symptoms in children are loss of appetite, abdominal pain, vomiting, weight loss, constipation, anemia, kidney failure, irritability, lethargy, learning disabilities, and behavioral problems.[48] Slow development of normal childhood behaviors, such as talking and use of words, and permanent intellectual disability are both commonly seen. Although less common, it is possible for fingernails to develop leukonychia striata if exposed to abnormally high lead concentrations.[49]
On July 30, 2020, a report by UNICEF and Pure Earth revealed that lead poisoning is affecting children on a "massive and previously unknown scale". According to the report, one in three children, up to 800 million globally, have blood lead levels at, or above, 5 micrograms per decilitre (µg/dL), the amount at which action is required.[50][51]
By organ system
Lead affects every one of the body's organ systems, especially the nervous system, but also the bones and teeth, the kidneys, and the
Kidneys
Kidney damage occurs with exposure to high levels of lead, and evidence suggests that lower levels can damage kidneys as well.
Cardiovascular system
Evidence suggests lead exposure is associated with
Reproductive system
Lead affects both the male and female reproductive systems. In men, when blood lead levels exceed 40 μg/dL,
Nervous system


Lead affects the peripheral nervous system (especially motor nerves) and the central nervous system.[30] Peripheral nervous system effects are more prominent in adults and central nervous system effects are more prominent in children.[36] Lead causes the axons of nerve cells to degenerate and lose their myelin coats.[30]
Lead exposure in young children has been linked to
The effect of lead on children's cognitive abilities takes place at very low levels.
High blood lead levels in adults are also associated with decreases in cognitive performance and with psychiatric symptoms such as depression and anxiety.[81] It was found in a large group of current and former inorganic lead workers in Korea that blood lead levels in the range of 20–50 μg/dL were correlated with neuro-cognitive defects.[82] Increases in blood lead levels from about 50 to about 100 μg/dL in adults have been found to be associated with persistent, and possibly permanent, impairment of central nervous system function.[63]
Lead exposure in children is also correlated with neuropsychiatric disorders such as attention deficit hyperactivity disorder and anti-social behaviour.[76] Elevated lead levels in children are correlated with higher scores on aggression and delinquency measures.[5] A correlation has also been found between prenatal and early childhood lead exposure and violent crime in adulthood.[72] Countries with the highest air lead levels have also been found to have the highest murder rates, after adjusting for confounding factors.[5] A May 2000 study by economic consultant Rick Nevin theorizes that lead exposure explains 65% to 90% of the variation in violent crime rates in the US.[83][84] A 2007 paper by the same author claims to show a strong association between preschool blood lead and subsequent crime rate trends over several decades across nine countries.[85][86] Lead exposure in childhood appears to increase school suspensions and juvenile detention among boys.[87] It is believed that the US ban on lead paint in buildings in the late 1970s, as well as the phaseout of leaded gasoline in the 1970s and 1980s, partially helped contribute to the decline of violent crime in the United States since the early 1990s.[86]
Exposure routes
| Part of a series on |
| Pollution |
|---|
 |
Lead is a common environmental pollutant.
Occupational exposure

In adults, occupational exposure is the main cause of lead poisoning.
Food
Lead may be found in food when food is grown in soil that is high in lead, airborne lead contaminates the crops, animals eat lead in their diet, or lead enters the food either from what it was stored or cooked in.[108] Ingestion of lead paint and batteries is also a route of exposure for livestock, which can subsequently affect humans.[109] Milk produced by contaminated cattle can be diluted to a lower lead concentration and sold for consumption.[110]
In Bangladesh,
In Hong Kong, the maximum allowed lead parts per million is 6 in solid foods and 1 in liquid foods.[115]
In December 2022, 28 dark chocolate brands were tested by Consumer Reports, which found that 23 of them contained cadmium, lead or both.[116] When cocoa beans are set outside near polluting industrial plants, they can be contaminated by dust containing lead.[117]
Cannabis
In 2007, a mass poisoning due to adulterated
Besides adulteration, cannabis plants have an inherent ability to absorb heavy metals from the soil. This makes them useful for remediating contaminated sites. But this may also make cannabis dangerous for consumers who ingest it. Some cannabis strains have been bred specifically to remove pollutants from soil, air or water, a method known as phytoremediation.[120]
In 2022, around 40% of cannabis products sold at unlicensed storefronts in New York City were found to contain heavy metals (e.g., lead, nickel), pesticides, and bacteria.[121]
Paint
Some lead compounds are colorful and are used widely in paints,[122][123] and lead paint is a major route of lead exposure in children.[124] A study conducted in 1998–2000 found that 38 million housing units in the US had lead-based paint, down from a 1990 estimate of 64 million.[125] Deteriorating lead paint can produce dangerous lead levels in household dust and soil.[126] Deteriorating lead paint and lead-containing household dust are the main causes of chronic lead poisoning.[32] The lead breaks down into the dust and since children are more prone to crawling on the floor, it is easily ingested.[125] Many young children display pica, eating things that are not food. Even a small amount of a lead-containing product such as a paint chip or a sip of glaze can contain tens or hundreds of milligrams of lead.[127] Eating chips of lead paint presents a particular hazard to children, generally producing more severe poisoning than occurs from dust.[128] Because removing lead paint from dwellings, e.g. by sanding or torching, creates lead-containing dust and fumes, it is generally safer to seal the lead paint under new paint (excepting moveable windows and doors, which create paint dust when operated).[129] Alternatively, special precautions must be taken if the lead paint is to be removed.[129]
In
Soil

Residual lead in soil contributes to lead exposure in urban areas.[18] It has been thought that the more polluted an area is with various contaminants, the more likely it is to contain lead. However, this is not always the case, as there are several other reasons for lead contamination in soil.[131]
Lead content in soil may be caused by broken-down lead paint, residues from lead-containing gasoline, used engine oil, tire weights, or pesticides used in the past, contaminated landfills, or from nearby industries such as foundries or smelters.[47] For example, in the Montevideo neighborhood of La Teja, former industrial sites became important sources of exposure in local communities in the early 2000s.[132] Although leaded soil is less of a problem in countries that no longer have leaded gasoline, it remains prevalent, raising concerns about the safety of urban agriculture;[133] eating food grown in contaminated soil can present a lead hazard.[134] Interfacial solar evaporation has been recently studied as a technique for remediating lead-contaminated sites, which involves the evaporation of heavy metal ions from moist soil.[135]

Water
Lead from the atmosphere or soil can end up in groundwater and surface water.
Like Flint, Michigan, and Washington, D.C., a similar situation affects the state of Wisconsin, where estimates call for replacement of up to 176,000 underground pipes made of lead known as lead service lines. The City of Madison, Wisconsin, addressed the issue and replaced all of their lead service lines, but there are still other cities that have yet to follow suit. While there are chemical methods that could help reduce the amount of lead in the water distributed, a permanent fix would be to replace the pipes completely. While the state may replace the pipes below ground, homeowners must replace the pipes on their property, at an average cost of $3,000.[143] Experts say that if the city were to replace their pipes and the citizens were to keep the old pipes located within their homes, there would be a potential for more lead to dissolve into their drinking water.[143] The US Congress authorized the EPA to dedicate funds to assist states and nonprofits with the costs of lead service line removal under Section 50105 of the Safe Drinking Water Act.[144]
Collected rainwater from roof runoff used as potable water may contain lead, if there are lead contaminants on the roof or in the storage tank.[22] The Australian Drinking Water Guidelines allow a maximum of 0.01 mg/L (10 ppb) lead in water.[22]
Lead wheel weights have been found to accumulate on roads and interstates and erode in traffic entering the water runoff through drains. Leaded fishing weights accumulate in rivers, streams, ponds, and lakes.
Gasoline
Tetraethyllead was first added to gasoline in 1923, as it helped prevent engine knocking. Automotive exhaust represented a major way for lead to be inhaled, invade the bloodstream and pass into the brain.[145]
The use of lead in gasoline peaked in the 1970s. By the next decade most high-income countries prohibited the use of leaded petrol. As late as 2002, almost all low- and middle-income countries, including some
Lead-containing products
Lead can be found in products such as kohl, an ancient cosmetic from the Middle East, South Asia, and parts of Africa that has many other names; and from some toys.[18] In 2007, millions of toys made in China were recalled from multiple countries owing to safety hazards including lead paint.[147] Vinyl mini-blinds, found especially in older housing, may contain lead.[24] Lead is commonly incorporated into
Ingestion of metallic lead, such as small lead fishing lures, increases blood lead levels and can be fatal.[149][150][151][152] Ingestion of lead-contaminated food is also a threat. Ceramic glaze often contains lead, and dishes that have been improperly fired can leach the metal into food, potentially causing severe poisoning.[153] In some places, the solder in cans used for food contains lead.[34] When manufacturing medical instruments and hardware, solder containing lead may be present.[154] People who eat animals hunted with lead bullets may be at risk for lead exposure.[155] Bullets lodged in the human body rarely cause significant levels of lead,[156][157] but bullets lodged in the joints are the exception, as they deteriorate and release lead into the body over time.[158]
In May 2015, Indian food safety regulators in the state of Uttar Pradesh found that samples of
Bullets
Contact with ammunition is a source of lead exposure. As of 2013, lead-based ammunition production is the second largest annual use of lead in the US, accounting for over 84,800 metric tons in 2013,
Because game animals can be shot using lead bullets, the potential for lead ingestion from game meat consumption has been studied clinically and epidemiologically. In a recent study conducted by the CDC,[170] a cohort from North Dakota was enrolled and asked to self-report historical consumption of game meat, and participation in other activities that could cause lead exposure. The study found that participants' age, sex, housing age, current hobbies with potential for lead exposure, and game consumption were all associated with blood lead level (PbB).
According to a study published in 2008, 1.1% of the 736 persons consuming wild game meat tested had PbB ≥5 μg/dl[171] In November 2015 the US Health and Human Services (HHS), Centers for Disease Control and Prevention (CDC), and National Institute for Occupational Safety and Health (NIOSH) designated 5 µg/dL (five micrograms per deciliter) of whole blood, in a venous blood sample, as the reference blood lead level for adults. An elevated blood lead level (BLL) is defined as a BLL ≥5 µg/dL. This case definition is used by the Adult Blood Lead Epidemiology and Surveillance (ABLES) program, the Council of State and Territorial Epidemiologists (CSTE), and CDC's National Notifiable Diseases Surveillance System (NNDSS). Previously (i.e. from 2009 until November 2015), the case definition for an elevated BLL was a BLL ≥10 µg/dL.[172]

To virtually eliminate the potential for lead contamination, some researchers have suggested the use of lead-free copper non-fragmenting bullets.[155]
Bismuth is an element used as a lead-replacement for shotgun pellets used in waterfowl hunting although shotshells made from bismuth are nearly ten times the cost of lead.
Opium
Lead-contaminated opium has been the source of poisoning in Iran and other Middle Eastern countries. This has also appeared in the illicit narcotic supply in North America, resulting in confirmed lead poisoning.[173]
Toxicokinetics

Toxicokinetics describes how the body handles the toxin over time, including absorption, distribution, metabolism, and excretion.
Exposure occurs through
The main body tissues that store lead are the blood, soft tissues, and bone; the half-life of lead in these tissues is measured in weeks for blood, months for soft tissues, and years for bone.[27] Lead in the bones, teeth, hair, and nails is bound tightly and not available to other tissues, and is generally thought not to be harmful.[177] In adults, 94% of absorbed lead is deposited in the bones and teeth, but children only store 70% in this manner, a fact which may partially account for the more serious health effects on children.[23] The half-life of lead in bone has been estimated as years to decades, and bone can introduce lead into the bloodstream long after the initial exposure is gone.[178][179][180] The half-life of lead in the blood in men is about 40 days, but it may be longer in children and pregnant women, whose bones are undergoing remodeling, which allows the lead to be continuously re-introduced into the bloodstream.[23] Also, if lead exposure takes place over years, clearance is much slower, partly due to the re-release of lead from bone.[181] Many other tissues store lead, but those with the highest concentrations (other than blood, bone, and teeth) are the brain, spleen, kidneys, liver, and lungs.[30] Lead is removed from the body very slowly, mainly through urine.[19] Smaller amounts of lead are also eliminated through the feces, and very small amounts in hair, nails, and sweat.[182]
Toxicodynamics
Toxicodynamics describes how the toxin affects the body, including the mechanisms causing its symptoms.
Lead has no known physiologically necessary role in the body,
Enzymes

The primary cause of lead's toxicity is its interference with a variety of enzymes because it binds to
The lead ion has a lone pair in its electronic structure, which can result in a distortion in the coordination of ligands, and in 2007 was hypothesized to be important in lead poisoning's effects on enzymes (see Lone pair § Unusual lone pairs).[186]
One of the main causes for the pathology of lead is that it interferes with the activity of an essential enzyme called
Neurons

The brain is the organ most sensitive to lead exposure.
Lead ions (Pb2+), like magnesium ions (Mg2+), block NMDA receptors. Therefore, an increase in Pb2+ concentration will effectively inhibit ongoing long-term potentiation (LTP), and lead to an abnormal increase in long-term depression (LTD) on neurons in the affected parts of the nervous system. These abnormalities lead to the indirect downregulation of NMDA-receptors, effectively initiating a positive feedback-loop for LTD.[201] The targeting of NMDA receptors is thought to be one of the main causes for lead's toxicity to neurons.[198]
Diagnosis
Diagnosis includes determining the clinical signs and the medical history, with inquiry into possible routes of exposure.[202] Clinical toxicologists, medical specialists in the area of poisoning, may be involved in diagnosis and treatment. The main tool in diagnosing and assessing the severity of lead poisoning is laboratory analysis of the blood lead level (BLL).[29]
Exposure to lead also can be evaluated by measuring
Blood lead levels are an indicator mainly of recent or current lead exposure, not of total
Fecal lead content that is measured over the course of a few days may also be an accurate way to estimate the overall amount of childhood lead intake. This form of measurement may serve as a useful way to see the extent of oral lead exposure from all the diet and environmental sources of lead.[210]
Lead poisoning shares symptoms with other conditions and may be easily missed.
Reference levels
The current reference range for acceptable blood lead concentrations in healthy persons without excessive exposure to environmental sources of lead is less than 3.5 µg/dL for children.[9] It was less than 25 µg/dL for adults.[211] Previous to 2012 the value for children was 10 (µg/dl).[212] Lead-exposed workers in the US are required to be removed from work when their level is greater than 50 µg/dL if they do construction and otherwise greater than 60 µg/dL.[213]
In 2015, the US Health and Human Services (HHS), Centers for Disease Control and Prevention (CDC), and National Institute for Occupational Safety and Health (NIOSH) designated 5 µg/dL (five micrograms per deciliter) of whole blood, in a venous blood sample, as the reference blood lead level for adults. An elevated blood lead level (BLL) is defined as a BLL ≥5 µg/dL. This case definition is used by the Adult Blood Lead Epidemiology and Surveillance (ABLES) program, the Council of State and Territorial Epidemiologists (CSTE), and CDC's National Notifiable Diseases Surveillance System (NNDSS). Previously (i.e. from 2009 until November 2015), the case definition for an elevated BLL was a BLL ≥10 µg/dL.[172] The US national BLL geometric mean among adults was 1.2 μg/dL in 2009–2010.[214]
Blood lead concentrations in poisoning victims have ranged from 30 to 80 µg/dL in children exposed to lead paint in older houses, 77–104 µg/dL in persons working with pottery glazes, 90–137 µg/dL in individuals consuming contaminated herbal medicines, 109–139 µg/dL in indoor shooting range instructors and as high as 330 µg/dL in those drinking fruit juices from glazed earthenware containers.[215]
Prevention

In most cases, lead poisoning is preventable[94] by avoiding exposure to lead.[22] Prevention strategies can be divided into individual (measures taken by a family), preventive medicine (identifying and intervening with high-risk individuals), and public health (reducing risk on a population level).[18]
Recommended steps by individuals to reduce the blood lead levels of children include increasing their frequency of hand washing and their intake of calcium and iron, discouraging them from putting their hands to their mouths, vacuuming frequently, and eliminating the presence of lead-containing objects such as blinds and jewellery in the house.[216] In houses with lead pipes or plumbing solder, these can be replaced.[216] Less permanent but cheaper methods include running water in the morning to flush out the most contaminated water, or adjusting the water's chemistry to prevent corrosion of pipes.[216] Lead testing kits are commercially available for detecting the presence of lead in the household.[217][153] Testing kit accuracy depends on the user testing all layers of paint and the quality of the kit; the US Environmental Protection Agency (EPA) only approves kits with an accuracy rating of at least 95%.[218][219] Professional lead testing companies caution that DIY test kits can create health risks for users that do not understand their limitations and liability issues for employers with regard to worker protection.[218] As hot water is more likely than cold water to contain higher amounts of lead, only cold water from the tap should be used for drinking, cooking, and making baby formula. Since most of the lead in household water usually comes from plumbing in the house and not from the local water supply, using cold water can avoid lead exposure.[220] Measures such as dust control and household education do not appear to be effective in changing children's blood levels.[221]
Prevention measures also exist on national and municipal levels. Recommendations by health professionals for lowering childhood exposures include banning the use of lead where it is not essential and strengthening regulations that limit the amount of lead in soil, water, air, household dust, and products.
Screening
Screening may be an important method of prevention for those at high risk,[18] such as those who live near lead-related industries.[29] The United States Preventive Services Task Force (USPSTF) has stated that general screening of those without symptoms include children and pregnant women is of unclear benefit as of 2019[update].[226] The American College of Obstetricians and Gynecologists (ACOG) and American Academy of Pediatrics (AAP), however, recommend asking about risk factors and testing those who have them.[227]
Education
The education of workers on lead, its danger and how its workplace exposure can be decreased, especially when initial blood lead level and urine lead level are high, could help reduce the risk of lead poisoning in the workplace.[11]
Treatment
| Blood lead level (μg/dL) |
Treatment |
|---|---|
| 10–14 | Education, repeat screening |
| 15–19 | Repeat screening, case management to abate sources |
| 20–44 | Medical evaluation, case management |
| 45–69 | Medical evaluation, chelation, case management |
| >69 | Hospitalization, immediate chelation, case management |
The mainstays of treatment are removal from the source of lead and, for people who have significantly high blood lead levels or who have symptoms of poisoning,
Before the advent of organic chelating agents, salts of iodide were given orally, such as heavily popularized by Louis Melsens and many nineteenth- and early twentieth-century doctors.[234][235]
![a chemical diagram of [CH2N(CH2CO2-)2]2 (shown in black) with the four O- tails binding a metal ion (shown in red).](http://upload.wikimedia.org/wikipedia/commons/thumb/0/09/Metal-EDTA.svg/220px-Metal-EDTA.svg.png)
A chelating agent is a molecule with at least two negatively charged groups that allow it to form complexes with metal ions with multiple positive charges, such as lead.
People receiving dimercaprol need to be assessed for peanut allergies since the commercial formulation contains peanut oil. Calcium EDTA is also effective if administered four hours after the administration of dimercaprol. Administering dimercaprol, DMSA (Succimer), or DMPS prior to calcium EDTA is necessary to prevent the redistribution of lead into the central nervous system.[240] Dimercaprol used alone may also redistribute lead to the brain and testes.[240] An adverse side effect of calcium EDTA is renal toxicity. Succimer (DMSA) is the preferred agent in mild to moderate lead poisoning cases. This may be the case in instances where children have a blood lead level >25μg/dL. The most reported adverse side effect for succimer is gastrointestinal disturbances.[7] It is also important to note that chelation therapy only lowers blood lead levels and may not prevent the lead-induced cognitive problems associated with lower lead levels in tissue. This may be because of the inability of these agents to remove sufficient amounts of lead from tissue or inability to reverse preexisting damage.[7] Chelating agents can have
Chelation challenge, also known as provocation testing, is used to indicate an elevated and mobilizable body burden of heavy metals including lead.[103] This testing involves collecting urine before and after administering a one-off dose of chelating agent to mobilize heavy metals into the urine.[103] Then urine is analyzed by a laboratory for levels of heavy metals; from this analysis overall body burden is inferred.[243] Chelation challenge mainly measures the burden of lead in soft tissues, though whether it accurately reflects long-term exposure or the amount of lead stored in bone remains controversial.[21][26] Although the technique has been used to determine whether chelation therapy is indicated and to diagnose heavy metal exposure, some evidence does not support these uses as blood levels after chelation are not comparable to the reference range typically used to diagnose heavy metal poisoning.[103] The single chelation dose could also redistribute the heavy metals to more sensitive areas such as central nervous system tissue.[103]
Epidemiology
Since lead has been used widely for centuries, the effects of exposure are worldwide.
Although regulation reducing lead in products has greatly reduced exposure in the developed world since the 1970s, lead is still allowed in products in many developing countries.
In developed countries, people with low levels of education living in poorer areas are most at risk for elevated lead.[54] In the US, the groups most at risk for lead exposure are the impoverished, city-dwellers, and immigrants.[72] African-American children and those living in old housing have also been found to be at elevated risk for high blood lead levels in the US.[250] Low-income people often live in old housing with lead paint, which may begin to peel, exposing residents to high levels of lead-containing dust.
Risk factors for elevated lead exposure include alcohol consumption and smoking (possibly because of contamination of tobacco leaves with lead-containing pesticides).[181] Adults with certain risk factors might be more susceptible to toxicity; these include calcium and iron deficiencies, old age, disease of organs targeted by lead (e.g. the brain, the kidneys), and possibly genetic susceptibility.[82] Differences in vulnerability to lead-induced neurological damage between males and females have also been found, but some studies have found males to be at greater risk, while others have found females to be.[36]
In adults, blood lead levels steadily increase with increasing age.[22] In adults of all ages, men have higher blood lead levels than women do.[22] Children are more sensitive to elevated blood lead levels than adults are.[251] Children may also have a higher intake of lead than adults; they breathe faster and may be more likely to have contact with and ingest soil.[126] Children of ages one to three tend to have the highest blood lead levels, possibly because at that age they begin to walk and explore their environment, and they use their mouths in their exploration.[36] Blood levels usually peak at about 18–24 months old.[19] In many countries including the US, household paint and dust are the major route of exposure in children.[126]
-
Map showing the mean blood lead levels (BLLs) of adults in China during 1980–2018.
-
Trend of blood lead levels (BLLs) in Chinese adults in different regions from 1980 to 2018. A decreasing trend was found in all regions except for South China.[252]
Notable cases
Cases of mass lead poisoning can occur. In 2009, 15,000 people were planned to be relocated from
The
Sex-specific susceptibility
Neuroanatomical pathology due to lead exposure is more pronounced in males, suggesting that lead-related toxicity has a disparate impact across sexes.[74]
Prognosis
Reversibility
Outcome is related to the extent and duration of lead exposure.[256] Effects of lead on the physiology of the kidneys and blood are generally reversible; its effects on the central nervous system are not.[64] While peripheral effects in adults often go away when lead exposure ceases, evidence suggests that most of lead's effects on a child's central nervous system are irreversible.[36] Children with lead poisoning may thus have adverse health, cognitive, and behavioral effects that follow them into adulthood.[47]
Encephalopathy
Lead encephalopathy is a medical emergency and causes permanent brain damage in 70–80% of children affected by it, even those that receive the best treatment.[29] The mortality rate for people who develop cerebral involvement is about 25%, and of those who survive who had lead encephalopathy symptoms by the time chelation therapy was begun, about 40% have permanent neurological problems such as cerebral palsy.[39]
Long-term
Exposure to lead may also decrease lifespan and have health effects in the long term.
Violence
Lead poisoning in children has been linked to changes in brain function that can result in low
History


Lead poisoning was among the first known and most widely studied work-related environmental hazards.[183] One of the first metals to be smelted and used,[122] lead is thought to have been discovered and first mined in Anatolia around 6500 BC.[124] Its density, workability, and corrosion resistance were among the metal's attractions.[183]
In the 2nd century BC the Greek botanist Nicander described the colic and paralysis seen in lead-poisoned people.[32][5] Dioscorides, a Greek physician who lived in the 1st century AD, wrote that lead makes the mind "give way".[122][263]
Lead was used extensively in
a hypothesis thoroughly disputed:The great disadvantage of lead has always been that it is poisonous. This was fully recognised by the ancients, and Vitruvius specifically warns against its use. Because it was nevertheless used in profusion for carrying drinking water, the conclusion has often been drawn that the Romans must therefore have suffered from lead poisoning; sometimes conclusions are carried even further and it is inferred that this caused infertility and other unwelcome conditions, and that lead plumbing was largely responsible for the decline and fall of Rome. Two things make this otherwise attractive hypothesis impossible. First, the
taps and the water was constantly running, it was never inside the pipes for more than a few minutes, and certainly not long enough to become contaminated.[266]
However, recent research supports the idea that the lead found in the water came from the supply pipes, rather than another source of contamination. It was not unknown for locals to punch holes in the pipes to draw water off, increasing the number of people exposed to the lead.
Romans also consumed lead through the consumption of
In 1983, environmental chemist
After
The painter Caravaggio might have died of lead poisoning. Bones with high lead levels were recently found in a grave thought likely to be his.[276] Paints used at the time contained high amounts of lead salts. Caravaggio is known to have exhibited violent behavior, a symptom commonly associated with lead poisoning.
In 17th-century Germany, the physician
In the 18th century lead poisoning was fairly frequent on account of the widespread drinking of
With the Industrial Revolution in the 19th century, lead poisoning became common in the work setting.[122] The introduction of lead paint for residential use in the 19th century increased childhood exposure to lead; for millennia before this, most lead exposure had been occupational.[36] The first legislation in the UK to limit pottery workers' exposure to lead was included in the Factories Act Extension Act in 1864, with further introduced in 1899.[283][284] William James Furnival (1853–1928), research ceramist of City & Guilds London Institute, appeared before Parliament in 1901 and presented a decade's evidence to convince the nation's leaders to remove lead completely from the British ceramic industry. His 852-page treatise, Leadless Decorative Tiles, Faience, and Mosaic of 1904 published that campaign and provided recipes to promote lead-free ceramics.[285] At the request of the Illinois state government in the US, Alice Hamilton (1869–1970) documented lead toxicity in Illinois industry and in 1911 presented results to the 23rd Annual Meeting of the American Economic Association.[286] Hamilton was a founder of the field of occupational safety and health and published the first edition of her manual, Industrial Toxicology, in 1934, yet in print in revised forms.[287] An important step in the understanding of childhood lead poisoning occurred when toxicity in children from lead paint was recognized in Australia in 1897.[122] France, Belgium, and Austria banned white lead interior paints in 1909; the League of Nations followed suit in 1922.[124] However, in the United States, laws banning lead house paint were not passed until 1971, and it was phased out and not fully banned until 1978.[124]
The 20th century saw an increase in worldwide lead exposure levels due to the increased widespread use of the metal.
The levels found today in most people are orders of magnitude greater than those of
In the late 1950s through the 1970s Herbert Needleman and Clair Cameron Patterson did research trying to prove lead's toxicity to humans.[295] In the 1980s Needleman was falsely accused of scientific misconduct by lead industry associates.[296][297]
In 2002 Tommy Thompson, United States Secretary of Health and Human Services, appointed at least two persons with conflicts of interest to the CDC's Lead Advisory Committee.[298][299]
In 2014 a case by the State of California against a number of companies decided against
... the judgment is reversed, and the matter is remanded to the trial court with directions to (1) recalculate the amount of the abatement fund to limit it to the amount necessary to cover the cost of remediating pre-1951 homes, and (2) hold an evidentiary hearing regarding the appointment of a suitable receiver. The Plaintiff shall recover its costs on appeal.[301]
On 6 December 2017, the petitions for rehearing from NL Industries, Inc., ConAgra Grocery Products Company and The Sherwin-Williams Company were denied.[301]
Studies have found a weak link between lead from leaded gasoline and crime rates.[302]
As of 2022[update] in the United States lead paint in rental housing remains a hazard to children. Both landlords and insurance companies have adopted strategies which limit the chance of recovery for damages due to lead poisoning: insurance companies by excluding coverage for lead poisoning from policies and landlords by crafting barriers to collection of any money damages compensating plaintiffs for damage.[303]
Other species
Humans are not alone in suffering from lead's effects; plants and animals are also affected by lead toxicity to varying degrees depending on species.
Farm animals such as cows and horses[306] as well as pet animals are also susceptible to the effects of lead toxicity.[237] Sources of lead exposure in pets can be the same as those that present health threats to humans sharing the environment, such as paint and blinds, and there is sometimes lead in toys made for pets.[237] Lead poisoning in a pet dog may indicate that children in the same household are at increased risk for elevated lead levels.[54]
Wildlife
Lead, one of the leading causes of toxicity in waterfowl, has been known to cause die-offs of wild bird populations.
The
See also
- 2015 incidents of lead in drinking water in Hong Kong
- Lead in chocolate
- Lead abatement
- Lead-based paint in the United States
- Lead production and applications
- Sick building syndrome
- Substance-induced psychosis
- Risk factors of schizophrenia
Notes
- ^ a b c d "Lead Information for Workers". CDC. 30 September 2013. Archived from the original on 18 October 2016. Retrieved 14 October 2016.
- ^ a b c d e f g h i j k l m n o p q r s t "Lead poisoning and health". WHO. September 2016. Archived from the original on 18 October 2016. Retrieved 14 October 2016.
- ISBN 978-0-323-07699-9.
- ^ PMID 25037135.
- ^ PMID 14746518.
- ^ a b "Lead Information for Employers". CDC. 30 September 2013. Archived from the original on 18 October 2016. Retrieved 14 October 2016.
- ^ PMID 17189579.
- ^ "CDC Updates Blood Lead Reference Value for Children". CDC. 28 October 2021. Archived from the original on Sep 22, 2023.
- ^ a b "Blood Lead Reference Value | Lead". CDC. 2021-10-28. Retrieved 2021-12-01.
- ^ The Code of Federal Regulations of the United States of America. U.S. Government Printing Office. 2005. p. 116. Archived from the original on 2017-11-05.
- ^ S2CID 226951902.
- ^ "What Do Parents Need to Know to Protect Their Children?". CDC. 30 October 2012. Archived from the original on 9 October 2016. Retrieved 14 October 2016.
- ^ Laborers' Health and Safety Fund of North America (11 February 2017). "Thousands of US Cities Have Worse Lead Problems Than Flint". Retrieved 26 September 2021.
- ^ "Lead exposure in last century shrunk IQ scores of half of Americans". Duke University. Retrieved 18 April 2022.
- PMID 35254913.
- PMID 763299. Retrieved 17 November 2020.
- ^ Grant (2009) p. 785
- ^ PMID 17448358.
- ^ a b c d e Pearson, Schonfeld (2003) p. 369
- ^ Trevor, Katzung, Masters (2007) p. 479
- ^ a b Lowry JA (2010). "Oral Chelation Therapy for Patients with Lead Poisoning" (PDF). WHO. Archived from the original (PDF) on 2016-01-26.
- ^ PMID 18787644.
- ^ PMID 16330345.
- ^ S2CID 41456653.
- ^ Grant (2009) p. 761
- ^ a b c d e f g h i j k Kosnett (2007) p. 948
- ^ PMID 18690981.
- ^ a b c d e Kosnett (2005) p. 825
- ^ a b c d e Mycyk, Hryhorczuk, Amitai (2005) p. 463
- ^ a b c d e f g h Dart, Hurlbut, Boyer-Hassen (2004) p. 1426
- ISBN 978-0-8493-7302-2.
- ^ S2CID 41427430.
- ^ a b c d Merrill, Morton, Soileau (2007) p. 860
- ^ PMID 16597190.
- ^ "Childhood Lead Exposure, Adult Personality, and Later-Life Mental Health". AMA Ed Hub. JN Learning. 3 September 2019. Retrieved 13 December 2020.
This JAMA Medical News video summarizes findings from a recent cohort study reporting an association between childhood lead exposure in Dunedin, New Zealand, and adult personality traits and psychopathology.
- ^ PMID 15060194.
- ^ a b c Kosnett (2006) p.240
- ^ a b Henretig (2006) p. 1314
- ^ a b c d e f g h i j k l Brunton (2007) p. 1131
- ISBN 0-7216-2921-0.
- PMID 20101339.
- ^ Rambousek (2008) p.177
- ^ Fintak DR (30 January 2007). "Wills Eye Resident Case Series". Archived from the original on 14 July 2014.
- ISBN 978-0-323-26462-4. Archivedfrom the original on 2017-10-30.
- PMID 12117650.
- ^ "Lead poisoning and health". www.who.int. Retrieved 2020-11-28.
- ^ PMID 17448360.
- ^ "Blood Lead Level Testing". Department of Ecology State of Washington. 2011. Archived from the original on 2016-02-04.
- ISBN 978-1-118-28670-8.
- ^ "Revealed: A third of world's children poisoned by lead, UNICEF analysis finds". UN News. 29 July 2020. Retrieved 30 July 2020.
- ^ "The Toxic Truth: Children's Exposure to Lead Pollution Undermines a Generation of Future Potential" (PDF). UNICEF. Retrieved 30 July 2020.
- ^ PMID 17904601.
- ^ PMID 16002379.
- ^ S2CID 21280606.
- S2CID 5453470.
- S2CID 37185511.
- PMID 2088735.
- PMID 10386553.
- PMID 11102303.
- PMID 12361944.
- PMID 15060208.
- ^ Agency for Toxic Substances and Disease Registry (August 20, 2007). "Lead Toxicity: Who Is at Risk of Lead Exposure?". Environmental Health and Medicine Education. U.S. Department of Health and Human Services. Course: WB 1105. Archived from the original on February 4, 2016.
- ^ a b Grant (2009) p. 789
- ^ a b c Rubin, Strayer (2008) p. 267
- S2CID 2043132.
- PMID 6434739.
- PMID 8035397.
- PMID 10914856.
- PMID 18091001.
- ^ Grant (2009) p. 792
- ^ PMID 18827541.
- PMID 15880700.
- ^ PMID 18507499.
- ^ PMID 12971691.
- ^ S2CID 22985838.
- PMID 2294437.
- ^ a b Merrill, Morton, Soileau (2007) p. 861
- ^ Casarett, Klaassen, Doull (2007) p. 944
- S2CID 39425465.
- PMID 17431502.
- ^ PMID 17431500.
- ^ "Research Links Lead Exposure to Changes in Violent Crime Rates Throughout the 20th century" (PDF). ICF International. Archived from the original (PDF) on 2010-12-30.
- S2CID 18983793.
- PMID 17451672.
- ^ a b Vedantam S (July 8, 2007). "Research links lead exposure, criminal activity". The Washington Post. Archived from the original on September 20, 2010. Retrieved September 24, 2009.
- doi:10.3386/w23392.
- ^ "Protect Your Family from Sources of Lead". 12 February 2013.
- ^ PMID 18418955.
- ^ "Parkinson s disease in occupational exposure to joss paper, a report of two cases".
- S2CID 226353498.
- ^ "Health risk of aerosols and toxic metals from incense and joss paper burning".
- ^ a b c "2013 Minerals Yearbook: LEAD" (PDF). Retrieved 2017-02-21.
- ^ PMID 12041847.
- S2CID 28603179.
- ^ Lewis J (May 1985). "Lead Poisoning: A Historical Perspective". EPA. Archived from the original on 2016-02-08.
- ^ Blum D (January 5, 2013). "Looney Gas and Lead Poisoning: A Short, Sad History". Wired. Archived from the original on March 21, 2017.
- ^ Drum K (January 2013). "America's Real Criminal Element: Lead". Mother Jones. Archived from the original on 2014-05-12.
- ^ Casciani D (April 20, 2014). "Did removing lead from petrol spark a decline in crime?". BBC. Archived from the original on January 24, 2017.
- PMID 32158988.
- ^ Blakemore E (June 2, 2017). "Humans Polluted the Air Much Earlier than Previously Thought". Smithsonian Magazine.
- ^ American Geophysical Union (May 31, 2017). "Human Activity Has Polluted European Air for 2000 Years". Eos Science News. Archived from the original on June 27, 2017.
- ^ PMID 17200393.
- ^ Turns A. "Mapping Our 'Pollution Landscape'". www.resurgence.org. Retrieved 2022-04-04.
- ^ a b Dart, Hurlbut, Boyer-Hassen (2004) p. 1424
- PMID 28376827.
- ^ "Occupational health and safety – chemical exposure". www.sbu.se. Swedish Agency for Health Technology Assessment and Assessment of Social Services (SBU). 2017-03-28. Archived from the original on 2017-06-06. Retrieved 2017-06-07.
- ISBN 978-0-87371-997-1. Archivedfrom the original on 2017-11-05.
- S2CID 3938066.
- PMID 9539015.
- ^ a b University S (24 September 2019). "Lead found in turmeric". Stanford News. Retrieved 25 September 2019.
- ^ "Researchers find lead in turmeric". phys.org. Retrieved 25 September 2019.
- ^ Piper K (20 September 2023). "Lead poisoning kills millions annually. One country is showing the way forward". Vox.
- PMID 37286126.
- ^ "Maximum Permitted Concentration of Certain Metals Present in Specified Foods". www.elegislation.gov.hk. Retrieved 15 April 2020.
- ^ "Consumer Reports urges dark chocolate makers to reduce lead, cadmium levels". www.yahoo.com. 23 January 2023. Retrieved 2023-01-28.
- ^ Dark chocolate is high in cadmium and lead. How much is safe to eat?
- ^ "Lead-Tainted Marijuana Poisons Users". ABC News.
- PMID 19623274.
- ^ "Cannabis may contain heavy metals and affect consumer health, study finds".
- ^ "Unlicensed weed tainted with E. coli, lead and salmonella, study finds". CBS News. December 2022.
- ^ a b c d e f g Henretig (2006) p. 1310
- ^ "Study results: Malawi and Botswana". Lead Elimination. 2021-07-13. Retrieved 2021-12-01.
- ^ PMID 16889836.
- ^ PMID 12361941.
- ^ a b c Dart, Hurlbut, Boyer-Hassen (2004) p. 1423
- ^ a b Kosnett (2006) p. 241
- ^ a b c d Chisolm (2004) pp. 221–22
- ^ a b Salvato (2003) p. 116
- ^ Kington T (2010-06-16). "The mystery of Caravaggio's death solved at last – painting killed him". The Guardian. Archived from the original on 2013-08-25.
- PMID 1208289.
- ^ "Living with lead in Uruguay". Toxic News. 2020-02-28. Retrieved 2022-01-26.
- ^ Murphy K (May 13, 2009). "For urban gardeners, lead is a concern". The New York Times. Archived from the original on May 3, 2014. Retrieved September 18, 2009.
- ^ a b Yu (2005) p. 188
- S2CID 239680091.
- ^ Yu (2005) p. 187
- ^ Menkes (2006) p. 703
- ^ PMID 16134575.
- University of Maryland. February 25, 2005. Archived from the originalon September 12, 2006. Retrieved 2007-11-07.
- ^ "HONORS". The Washington Post. February 23, 2005.
- ^ Ingraham C (15 January 2016). "This is how toxic Flint's water really is". The Washington Post.
- ^ McLaughlin EC (18 January 2016). "Flint's water crisis: 5 things to know". CNN. Archived from the original on 23 January 2016.
- ^ a b Johnson S (2017-10-30). "Wisconsin Senate Unanimously Passes Bill to Remove Lead Water Pipes". Wisconsin Public Radio.
- ^ Humphreys Elena, H., Ramseur J (2022-01-04). "Infrastructure Investment and Jobs Act (IIJA): Drinking Water and Wastewater Infrastructure". Congressional Research Service. Library of Congress. Retrieved 2023-01-15.
{{cite web}}: CS1 maint: multiple names: authors list (link) - ^ Lead Exposure in Last Century Shrank IQ Scores of Half of Americans
- ^ Era of leaded petrol over, eliminating a major threat to human and planetary health
- ^ "Mattel CEO: 'Rigorous standards' after massive toy recall". CNN. November 15, 2007. Archived from the original on August 25, 2009. Retrieved September 26, 2009.
- ^ "Lead Poisoning from Mexican Folk Remedies – California". Morbidity and Mortality Weekly Report. 32 (42). October 28, 1983.
- PMID 16625019.
- PMID 3190952.
- S2CID 1834967.
- PMID 16572103.
- ^ a b Salvato (2003) p.117
- ^ Bastow E (2011-02-28). "The Best Way To Solder Nitinol". Indium Corporation Blogs. Archived from the original on 2015-04-18. Retrieved 2011-12-03.
- ^ PMID 19390698.
- PMID 18813727.
- PMID 6859004.
- PMID 2926538.
- ^ Merofact Awareness Team (19 May 2015). "Doubts over MSG and Lead Content in Maggi Instant Noodles". Archived from the original on 14 January 2016.
- ^ "Beware! Eating 2 -Minute Maggi Noodles can ruin your Nervous System". news.biharprabha.com. 18 May 2015. Archived from the original on 21 May 2015. Retrieved 18 May 2015.
- ^ "Maggi Noodles Packets Recalled Across Uttar Pradesh, Say Food Inspectors: Report". NDTV. New Delhi, India. 20 May 2015. Archived from the original on 25 May 2015. Retrieved 20 May 2015.
- ^ Dey S (16 May 2015). "'Maggi' under regulatory scanner for lead, MSG beyond permissible limit". The Times of India. New Delhi, India. Archived from the original on 26 May 2015. Retrieved 20 May 2015.
- from the original on 16 October 2015. Retrieved 3 June 2015.
- ^ IANS (June 4, 2015). "Gujarat bans Maggi noodles for 30 days". The Times of India. (The Times Group). Archived from the original on 2015-06-07. Retrieved June 4, 2015.
- FirstPost. Archivedfrom the original on 4 June 2015. Retrieved 3 June 2015.
- ^ "Lead Statistics and Information" (PDF). Mineral Industry Surveys. U.S. Department of the Interior. Archived (PDF) from the original on 2016-03-10. Retrieved 2016-07-11.
- ^ "Trumpeter Swan Society vs EPA" (PDF). United States Court of Appeals for the District of Columbia Circuit. Archived from the original (PDF) on 2016-05-06.
- ^ "Lead Exposure in Wisconsin Birds" (PDF). Wisconsin Department of Natural Resources. 3 September 2008. Archived (PDF) from the original on 28 July 2013. Retrieved 10 December 2012.
- ^ Wheeling K (8 February 2018). "An Environmental Case for Biodegradable Bullets". Pacific Standard. Retrieved 9 February 2018.
- PMID 19747676.
- ^ Iqbal S. "Epi-AID Trip Report: Assessment of human health risk from consumption of wild game meat with possible lead contamination among the residents of the State of North Dakota" (PDF). Epi-AID Trip Report. National Center for Environmental Health, Centers for Disease Control and Prevention: Atlanta, Georgia, USA. Archived from the original (PDF) on May 26, 2011. Retrieved March 2, 2011.
- ^ a b "CDC - Adult Blood Lead Epidemiology and Surveillance (ABLES): Program Description: NIOSH Workplace Safety and Health Topic". The National Institute for Occupational Safety and Health (NIOSH). US Center for Disease Control. 2017-08-10. Retrieved 2017-11-19.
- S2CID 221017132.
- PMID 35051994.
- ISBN 978-0-87371-997-1.
- ^ Grant (2009) p. 767
- ^ Rubin, Strayer (2008) p. 266
- ^ "Biomonitoring Summary, Lead". CDC. 7 April 2017. Retrieved 3 February 2021.
- PMID 8277545. Retrieved 3 February 2021.
- PMID 2040248.
- ^ PMID 17431499.
- ^ a b Kosnett (2006) p.238
- ^ PMID 19106443.
- ^ Yu (2005) p.193
- ^ a b c Casarett, Klaassen, Doull (2007) p. 946
- PMID 17152108.
- S2CID 38826214.
- PMID 17366816.
- ^ Chhabra N (November 15, 2015). "Effect of Lead poisoning on heme biosynthetic pathway". Clinical Cases: Biochemistry For Medics. Archived from the original on 3 April 2016. Retrieved 30 October 2016.
- PMID 12498316.
- ^ a b Mycyk, Hryhorczuk, Amitai (2005) p. 462
- ^ a b Kosnett (2005) p. 822
- ^ Vannotti A (1954). Porphyrins: Their Biological and Chemical Importance. Hilger & Watts, Hilger Division. p. 126.
Indeed, lead poisoning, like all porphyrin diseases, is accompanied by obstinate constipation, nervous lesions, hyperpigmentation and abdominal attacks.
- ISBN 978-3-642-04519-6. Archivedfrom the original on 8 September 2017.
- PMID 25653942.
- PMID 28630774.
- PMID 23236641. Retrieved 28 February 2020.
the symptoms in lead poisoning closely mimic those of acute porphyria
- ^ PMID 19374778.
- PMID 12477693.
- PMID 19476290.
- ^ "How Lead Changes the Brain to Impair Learning and Memory, How Lead Changes the Brain to Impair Learning and Memory". Johns Hopkins Bloomberg School of Public Health. 3 August 2000. Archived from the original on 2007-08-16. Retrieved 2007-08-14.
- ^ a b Henretig (2006) p. 1316
- ^ Fred HL, van Dijk HA. "Images of Memorable Cases: Case 81". Connexions. Retrieved August 25, 2009.
- PMID 6999974.
- ^ Fischer C (2007). Kaplan Medical USMLE Steps 2 and 3 Notes: Internal Medicine, Hematology. pp. 176–177.
- ISBN 978-1-4511-7268-3.
- ^ Grant (2009) p. 784
- PMID 18567711.
- ^ a b c Mycyk, Hryhorczuk, Amitai (2005) p. 464
- PMID 15626656.
- ^ Wu, A. (2006) Tietz Clinical Guide to Laboratory Tests, 4th ed., Saunders Elsevier, St. Louis, MO, pp. 658–659.
- ^ "Low Level Lead Exposure Harms Children: A Renewed Call for Primary Prevention" (PDF). U.S. Centers for Disease Control and Prevention. Archived (PDF) from the original on 9 January 2012. Retrieved 5 January 2012.
- ^ "CDC - Adult Blood Lead Epidemiology and Surveillance (ABLES): Program Description: NIOSH Workplace Safety and Health Topic". www.cdc.gov. 28 November 2018. Retrieved 31 October 2019.
- ^ "Fourth National Report on Human Exposure to Environmental Chemicals. Updated Tables" (PDF). US Department of Health and Human Services. Atlanta, GA: cdc.gov. September 2012. Archived (PDF) from the original on 2017-05-01.
- ISBN 978-0-9626523-7-0.
- ^ PMID 18663205.
- ^ "How to Test Paint With a DIY Lead Test Kit: CR's step-by-step guide to getting accurate results from 3M LeadCheck and D-Lead". Consumer Reports. 15 October 2017. Retrieved 2021-02-12.
- ^ a b "DIY Lead Paint Test Kits Explained: Do They Really Work?". 27 August 2020.
- ^ "Lead Test Kits". 12 February 2013.
- ^ National Environmental Public Health Tracking Network, 2010.
- PMID 33022752.
- ^ Chisamera D (October 19, 2008). "EPA Sets Tightest Lead Air Emission Standard". eFluxMedia. Archived from the original on June 4, 2009.
- National Public Radio. August 25, 2009. Archivedfrom the original on August 27, 2009. Retrieved August 25, 2009.
- ^ Saulny S (September 13, 2009). "Treece Journal: Welcome to Our Town. Wish We Weren't Here". The New York Times. Archived from the original on 2013-08-13.
- ^ "10 Policies to Prevent and Respond to Childhood Lead Exposure". The Pew Charitable Trusts. 30 August 2017. Retrieved 14 June 2018.
- S2CID 116860513.
- from the original on 16 April 2019.
- ^ Kosnett (2006) p. 242
- ^ Henretig (2006) p. 1321
- ^ Mycyk, Hryhorczuk, Amitai (2005) p. 465
- ^ a b Olson (2007) p. 1658
- ^ Kosnett (2005) p. 832
- ^ Kosnett (2007) p. 949
- ^ "Sur l'emploi de l'iodure de potassium pour combattre les affections saturnines et mercurielles", in Annales de chimie et de physique, t. 26, 3e série, 1849.
- ^ "On the Employment of Iodide of Potassium as a Remedy for the Affections Caused by Lead and Mercury", in Br Foreign Med Chir Rev. 1853 Jan; 11(21): 201–224.
- ^ Trevor, Katzung, Masters (2007) p. 480
- ^ PMID 18406386.
- ^ Menkes (2006) p.706
- ^ PMID 18436472.
- ^ PMID 20717537.
- S2CID 29615354.
- ^ Pearson, Schonfeld (2003) p. 370
- PMID 7697134.
- ^ Needleman HL (June 28, 1999). "The Removal of Lead from Gasoline" (PDF). University of North Carolina. Archived (PDF) from the original on March 3, 2016.
- ISBN 978-92-4-156387-1. Archived(PDF) from the original on 2012-02-14.
- ^ "Legally-binding controls on lead paint". www.who.int. Retrieved 2023-01-15.
- OCLC 1102765674.)
{{cite book}}: CS1 maint: location missing publisher (link - PMID 14580791.
- ^ "THE PUBLIC HEALTH IMPACT OF CHEMICALS: KNOWNS AND UNKNOWNS". World Health Organization. 2016-05-23. Retrieved 2023-01-15.
- S2CID 29464201.
- S2CID 27759109.
- S2CID 234495451.
- ^ "China to relocate 15,000 from lead-poisoned area". AFP. 2009-10-16. Archived from the original on 2009-10-19. Retrieved 2009-10-20.
- ^ "China to move residents from lead smelter base-report". Reuters. 2009-10-18. Archived from the original on 2018-03-14. Retrieved 2009-10-20.
- ^ "Aid groups say lead poisoning has killed 400 children in Nigeria". Associated Press. 2010-10-05. Archived from the original on 2011-08-05. Retrieved 2010-10-05.
- ^ Chisolm (2004) p. 223
- ^ Merrill, Morton, Soileau (2007) p. 862
- PMID 31932788.
- S2CID 85530942. Retrieved March 13, 2021.
Associations between childhood BLL and adult personality and psychopathology remained significant even after adjusting for sex, maternal IQ, socioeconomic status, and family history of mental illness.
- ISSN 0037-7732.
- S2CID 5706643.
- ^ PMID 22484219.
- PMID 19344860.
- ISBN 978-1-888456-03-5.
- PMID 17079773.
- ^ Hodge 1992, p. 308
- ^ Director: Chris Warren (2004). Tales of the Living Dead: Poisoned Roman Babies (television). Brighton TV for National Geographic.
- PMID 6338384.
- PMID 6389691.
- PMID 24753588.
- ^ "Ancient Rome's tap water heavily contaminated with lead, researchers say". The Guardian. 21 April 2014. Archived from the original on 2017-02-27.
- ^ Tarlach G. "Lead in Ancient Rome's Water Was 100 Times Natural Levels". Discover. Archived from the original on 2016-01-14.
- ^ PMID 10940962.
- ^ PMID 6750289.
- S2CID 35548035.
- ^ Kington T (16 June 2010). "The mystery of Caravaggio's death solved at last – painting killed him". The Guardian. Archived from the original on 2013-08-25.
- ^ Varney TL, Murphy AR, et al. (October 2012). "A Preliminary Investigation of Lead Poisoning in a Napoleonic Era Naval Cemetery in Antigua, W.I." (PDF). Caribbean Connection. 2. Archived from the original (PDF) on November 22, 2021.
- ISBN 978-0-521-38922-8.
- ISBN 978-0-385-49540-0.
- ^ "Benjamin Franklin's Lead Letter, History's Lead Story". The Franklin Institute. 2010. Archived from the original on 2014-04-09.
- ^ PMID 17214130.
- ^ Weiss R (December 6, 2005). "Study Concludes Beethoven Died From Lead Poisoning". The Washington Post. Archived from the original on 2017-02-15.
- ^ "Stoke Museums - Health Risks in a Victorian Pottery Industry". Stoke Museums. 7 July 2012. Archived from the original on 7 July 2012. Retrieved 23 February 2022.
- ^ "Timeline - History of Occupational Safety and Health".
- ^ Furnival WJ (1904). Leadless Decorative Tiles, Faience, and Mosaic, comprising notes and receipts on the History, Materials, Manufacture & Use of Ornamental Flooring Tiles, Ceramic Mosaic, and Decorative Tiles and Faience. W.J. Furival, Stone, Staffordshire.
- ^ Hamilton A (April 1911). "Lead Poisoning in Illinois". The American Economic Review. 1 (2): 257–264.
- ^ Hamilton DA (1934). Industrial Toxicology. University of Michigan.
- ^ Grant (2009) p. 757
- ^ Jenssen V (2022). "Ch.16 Unsafe Studio Practice; Lead Poisoning". The Art of Carol Janeway. Friesen Press. pp. 198–206.
- ^ Mycyk, Hryhorczuk, Amitai (2005) p. 467
- ISBN 978-0-7637-5925-4.
- S2CID 232222146.[permanent dead link]
- ^ Grant (2009) p. 758
- ^ Agency for Toxic Substances and Disease Registry (August 20, 2007). "Lead Toxicity Cover Page". Environmental Health and Medicine Education. U.S. Department of Health and Human Services. Course: WB 1105. Archived from the original on July 18, 2012.
- ISBN 978-0-8070-0032-8.
- ISBN 978-0-674-00222-7.
- from the original on 3 September 2014.
- ^ "Lead Poisoning Prevention Panel Influenced by Industry". The Center for Science and Democracy. Union of Concerned Scientists. 8 February 2004. Archived from the original on 25 October 2008. Retrieved 8 October 2002.
- ^ Markey EJ (8 October 2002). "Turning Lead Into Gold: How the Bush Administration is Poisoning the Lead Advisory Committee at the CDC" (PDF). US House of Representatives. Archived from the original (PDF) on 24 October 2002. Retrieved 28 August 2014.
- ^ Hsiao H, Stanley A. "Lead Paint Companies Hit With Billion Dollar Judgment in California Public Nuisance Case" (PDF). Archived from the original (PDF) on 1 December 2017. Retrieved 21 August 2016.
- ^ a b Mihara ND, Premo EM, Elia FD (2017-11-14). "The People v. ConAgra Grocery Products Company et al". California Courts - Appellate Court Case Information. Judicial Council of California. Retrieved 2017-11-19.
...we can accept the inference that defendants' pre-1951 promotions increased the use of lead paint on residential interiors during the period of those promotions...
- PMID 24555074.
- ^ Ellen Gabler (March 29, 2022). "How 2 Industries Stymied Justice for Young Lead Paint Victims". The New York Times. Retrieved March 29, 2022.
- PMID 18406387.
- ^ Grant (2009) pp. 768, 771, 774
- PMID 1107364.
- S2CID 9693691.
- ^ Federal Cartridge Company Waterfowl and Steel Shot Guide. Volume I; 1988.
- ^ PMID 18406388.
- ^ PMID 19107211.
- ^ "Get the Lead Out (Protecting the Condor)". California Department of Fish and Game. Archived from the original on 2007-12-19. Retrieved 2009-07-28.
References
- Brunton LL, Goodman LS, Blumenthal D, Buxton I, Parker KL, eds. (2007). "Principles of toxicology". Goodman and Gilman's Manual of Pharmacology and Therapeutics. McGraw-Hill Professional. ISBN 978-0-07-144343-2.
- Casarett LJ, Klaassen CD, Doull J, eds. (2007). "Toxic effects of metals". Casarett and Doull's Toxicology: The Basic Science of Poisons (7th ed.). McGraw-Hill Professional. ISBN 978-0-07-147051-3.
- Chisolm JJ (2004). "Lead poisoning". In Crocetti M, Barone MA, Oski FA (eds.). Oski's Essential Pediatrics (2nd ed.). Lippincott Williams & Wilkins. ISBN 978-0-7817-3770-8.
- Dart RC, Hurlbut KM, Boyer-Hassen LV (2004). "Lead". In Dart RC (ed.). Medical Toxicology (3rd ed.). Lippincott Williams & Wilkins. ISBN 978-0-7817-2845-4.
- Grant LD (2009). "Lead and compounds". In Lippmann M (ed.). Environmental Toxicants: Human Exposures and Their Health Effects (3rd ed.). Wiley-Interscience. ISBN 978-0-471-79335-9.
- Henretig FM (2006). "Lead". In Goldfrank LR (ed.). Goldfrank's Toxicologic Emergencies (8th ed.). McGraw-Hill Professional. ISBN 978-0-07-143763-9.
- Hodge AT (1992). Roman Aqueducts & Water Supply. London: Duckworth. ISBN 978-0-7156-2194-3.
- Kosnett MJ (2005). "Lead". In Brent J (ed.). Critical Care Toxicology: Diagnosis and Management of the Critically Poisoned Patient. Gulf Professional Publishing. ISBN 978-0-8151-4387-1.
- Kosnett MJ (2007). "Heavy metal intoxication and chelators". In Katzung BG (ed.). Basic and Clinical Pharmacology. McGraw-Hill Professional. ISBN 978-0-07-145153-6.
- Kosnett MJ (2006-09-18). "Lead". In Olson KR (ed.). Poisoning and Drug Overdose (5th ed.). McGraw-Hill Professional. p. 2006. ISBN 978-0-07-144333-3.
- Menkes JH (2006). "Toxic and nutritional disorders". In Menkes JH, Sarnat HB, Maria BL (eds.). Child Neurology (7th ed.). Lippincott Williams & Wilkins. p. 706. ISBN 978-0-7817-5104-9.
- Merrill JG, Morton JJ, Soileau SD (2007). "Metals". In Hayes AW (ed.). Principles and Methods of Toxicology (5th ed.). CRC Press. ISBN 978-0-8493-3778-9.
- Mycyk M, Hryhorczuk D, Amitai Y (2005). "Lead". In Erickson TB, Ahrens WR, Aks S, Ling L (eds.). Pediatric Toxicology: Diagnosis and Management of the Poisoned Child. McGraw-Hill Professional. ISBN 978-0-07-141736-5.
- Olson KR (2007). "Poisoning". In McPhee SJ, Tierney LM, Papadakis MA (eds.). Current Medical Diagnosis and Treatment (46th ed.). McGraw-Hill Professional. ISBN 978-0-07-147247-0.
- Pearson HA, Schonfeld DJ (2003). "Lead". In Rudolph CD (ed.). Rudolph's Pediatrics (21st ed.). McGraw-Hill Professional. ISBN 978-0-8385-8285-5.
- Rambousek AJ, ed. (2008). "The symptoms and treatment of industrial poisoning". Industrial Poisoning from Fumes, Gases, and Poisons of Manufacturing Processes. READ BOOKS. ISBN 978-1-4086-7025-5.
- Rubin R, Strayer DS, eds. (2008). "Environmental and nutritional pathology". Rubin's Pathology: Clinicopathologic Foundations of Medicine (5th ed.). Lippincott Williams & Wilkins. ISBN 978-0-7817-9516-6.
- Salvato JA, Nemerow NL, Agardy FJ, eds. (2003). "Noninfectious and noncommunicable diseases and conditions associated with the environment, including air, water, and food". Environmental Engineering (5th ed.). John Wiley and Sons. ISBN 978-0-471-41813-9.
- Trevor AJ, Katzung BG, Masters SB, eds. (2007). "Heavy metals". Katzung & Trevor's Pharmacology: Examination & Board Review (8th ed.). McGraw-Hill Professional. ISBN 978-0-07-148869-3.
- Yu MH (2005). "Soil and water pollution: Environmental metals and metalloids". Environmental Toxicology: Biological and Health Effects of Pollutants. CRC Press. ISBN 978-1-56670-670-4.
Further reading
- Binns HJ, Ricks OB. "Helping Parents Prevent Lead Poisoning". ERIC Digest. Archived from the original on 2004-05-05. Retrieved 2004-06-23.
- Karalus DE (2010). "Review: The Great Lead Water Pipe Disaster". Electronic Green Journal. 1 (29). .
- Küpper H (2017). "Chapter 15. Lead Toxicity in Plants". In Astrid S, Helmut S, Sigel RK (eds.). Lead: Its Effects on Environment and Health. Metal Ions in Life Sciences. Vol. 17. de Gruyter. pp. 491–500. PMID 28731308.
- Liu KS, Hao JH, Zeng Y, Dai FC, Gu PQ (September 2013). "Neurotoxicity and biomarkers of lead exposure: a review". Chin Med Sci J. 28 (3): 178–88. PMID 24074621.
- Ordemann JM, Austin RN (June 2016). "Lead neurotoxicity: exploring the potential impact of lead substitution in zinc-finger proteins on mental health". Metallomics. 8 (6): 579–88. PMID 26745006.
- Vorvolakos T, Arseniou S, Samakouri M (2016). "There is no safe threshold for lead exposure: Α literature review". Psychiatriki. 27 (3): 204–214. PMID 27837574.
External links
- Agency for Toxic Substances and Disease Registry (August 20, 2007). "Lead Toxicity". Environmental Health and Medicine Education. U.S. Department of Health and Human Services. Course: WB 1105.
- Agency for Toxic Substances and Disease Registry. "Lead | Medical Management Guidelines | Toxic Substance Portal | ATSDR".
- "Toxicological Profile for Lead". ATSDR, CDC. 2020. ) Peer-reviewed profile that characterizes the toxicology and health effects information, identifies and reviews the key literature that describes lead's toxicological properties.
- Health and Safety Executive UK. "Lead". Working safely with lead. HSE.
- Katz NL (June 26, 2007). "City payout to Brooklyn family largest ever in lead poisoning". NY Daily News. Archived from the original on 2011-06-03. Retrieved 2009-09-28.
- National Institute for Occupational Safety and Health (2018-06-20). "Lead". NIOSH Workplace Safety & Health Topics. Centers for Disease Control and Prevention.
- National Pollutant Inventory. "Lead and compounds: Health effects". Fact Sheets. Canberra, Australia: Department of Sustainability, Environment, Water, Population and Communities. Archived from the original on 2012-03-20.
- National Safety Council (2008). "Lead Poisoning" (PDF). Fact Sheets. Itasca, Illinois, U.S.: National Safety Council. Archived from the original (PDF) on 2017-12-22. Retrieved 2016-06-11.
- The Associated Press (30 Nov 2023). "Biden administration proposes strictest lead pipe rules in more than three decades". NPR. Retrieved 13 Mar 2024.
- Davenport C (12 Jul 2023). "E.P.A. Proposes Tighter Limits on Lead Dust in Homes and Child Care Facilities". The New York Times. Retrieved 13 Mar 2024.


![Trend of blood lead levels (BLLs) in Chinese adults in different regions from 1980 to 2018. A decreasing trend was found in all regions except for South China.[252]](http://upload.wikimedia.org/wikipedia/commons/thumb/6/60/Trend_of_blood_lead_levels_in_Chinese_adults_in_different_regions_from_1980_to_2018.jpg/330px-Trend_of_blood_lead_levels_in_Chinese_adults_in_different_regions_from_1980_to_2018.jpg)