Ascending cholangitis
| Ascending cholangitis | |
|---|---|
| Other names | acute cholangitis, cholangitis |
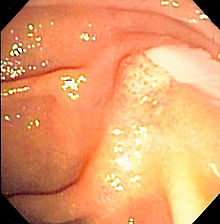 | |
| Duodenoscopy image of pus extruding from the ampulla of Vater, indicative of cholangitis | |
| Specialty | Gastroenterology General surgery |
| Symptoms | jaundice, fever and abdominal pain |
Ascending cholangitis, also known as acute cholangitis or simply cholangitis, is inflammation of the bile duct, usually caused by bacteria ascending from its junction with the duodenum (first part of the small intestine). It tends to occur if the bile duct is already partially obstructed by gallstones.[1][2]
Cholangitis can be life-threatening, and is regarded as a
Signs and symptoms

A person with cholangitis may complain of
In the elderly, the presentation may be atypical; they may directly collapse due to sepsis without first showing typical features.[2] Those with an indwelling stent in the bile duct (see below) may not develop jaundice.[2]
Causes
Bile duct obstruction, which is usually present in acute cholangitis, is generally due to
Parasites which may infect the liver and bile ducts may cause cholangitis; these include the
The presence of a permanent biliary stent (e.g. in pancreatic cancer) slightly increases the risk of cholangitis, but stents of this type are often needed to keep the bile duct patent under outside pressure.[1]
Pathogenesis

Bile is produced by the liver, and serves to eliminate
The biliary tree is normally relatively free of bacteria because of certain protective mechanisms. The sphincter of Oddi acts as a mechanical barrier. The biliary system normally has low pressure (8 to 12
Bacterial contamination alone in absence of obstruction does not usually result in cholangitis.
In ascending cholangitis, it is assumed that organisms migrate backwards up the bile duct as a result of partial obstruction and decreased function of the sphincter of Oddi.
Diagnosis
Blood tests
Routine
Blood cultures are often performed in people with fever and evidence of acute infection. These yield the bacteria causing the infection in 36% of cases,[12] usually after 24–48 hours of incubation. Bile, too, may be sent for culture during ERCP (see below). The most common bacteria linked to ascending cholangitis are gram-negative bacilli: Escherichia coli (25–50%), Klebsiella (15–20%) and Enterobacter (5–10%). Of the gram-positive cocci, Enterococcus causes 10–20%.[13]
Medical imaging

Given that ascending cholangitis usually occurs in the setting of bile duct obstruction, various forms of
The
If other causes rather than gallstones are suspected (such as a
Treatment
Fluids and antibiotics
Cholangitis requires admission to hospital.
Endoscopy
The definitive treatment for cholangitis is relief of the underlying biliary obstruction.[1] This is usually deferred until 24–48 hours after admission, when the patient is stable and has shown some improvement with antibiotics, but may need to happen as an emergency in case of ongoing deterioration despite adequate treatment,[1] or if antibiotics are not effective in reducing the signs of infection (which happens in 15% of cases).[2][3]
Narrowed areas may be bridged by a
Percutaneous biliary drainage
In cases where a person is too ill to tolerate endoscopy or when a retrograde endoscopic approach fails to access the obstruction, a percutaneous transhepatic cholangiogram (PTC) may be performed to evaluate the biliary system for placement of a percutaneous biliary drain (PBD).[20][3] This is often necessary in the case of a proximal stricture or a bilioenteric anastomosis (a surgical connection between the bile duct and small bowel, such as the duodenum or jejunum).[2] Once access across the stricture is obtained, balloon dilation can be performed and stones can be swept forward into the duodenum.[20] Due to potential complications of percutaneous biliary drain placement and the necessity of regular drain maintenance,[2] a retrograde approach via ERCP remains first-line therapy.[1]
Cholecystectomy
Not all gallstones implicated in ascending cholangitis actually originate from the gallbladder, but cholecystectomy (surgical removal of the gallbladder) is generally recommended in people who have been treated for cholangitis due to gallstone disease. This is typically delayed until all symptoms have resolved and ERCP or MRCP have confirmed that the bile duct is clear of gallstones.[1][2][3] Those who do not undergo cholecystectomy have an increased risk of recurrent biliary pain, jaundice, further episodes of cholangitis, and need for further ERCP or cholecystostomy; the risk of death is also significantly increased.[21]
Prognosis
Acute cholangitis carries a significant risk of death, the leading cause being irreversible
Risk factors indicating an increased risk of death include older age, female gender, a history of
Epidemiology
In the Western world, about 15% of all people have gallstones in their gallbladder but the majority are unaware of this and have no symptoms. Over ten years, 15–26% will have one or more episodes of biliary colic (abdominal pain due to the passage of gallstones through the bile duct into the digestive tract), and 2–3% will develop complications of obstruction: acute pancreatitis, cholecystitis or acute cholangitis.[3] Prevalence of gallstone disease increases with age and body mass index (a marker of obesity). However, the risk is also increased in those who lose weight rapidly (e.g. after weight loss surgery) due to alterations in the composition of the bile that makes it prone to form stones. Gallstones are slightly more common in women than in men, and pregnancy increases the risk further.[24]
History
Dr Jean-Martin Charcot, working at the Salpêtrière Hospital in Paris, France, is credited with early reports of cholangitis, as well as his eponymous triad, in 1877.[4] He referred to the condition as "hepatic fever" (fièvre hépatique).[4][7] Dr Benedict M. Reynolds, an American surgeon, reignited interest in the condition in his 1959 report with colleague Dr Everett L. Dargan, and formulated the pentad that carries his name.[5] It remained a condition generally treated by surgeons, with exploration of the bile duct and excision of gallstones, until the ascendancy of ERCP in 1968.[25] ERCP is generally performed by internal medicine or gastroenterology specialists. In 1992 it was shown that ERCP was generally safer than surgical intervention in ascending cholangitis.[26]
See also
- Primary sclerosing cholangitis (an autoimmune disease leading to narrowing of the bile ducts)
- Gallstone-related pancreatitis
References
- ^ PMID 17556149.
- ^ ISBN 978-0-07-141090-8.
- ^ S2CID 206945855.
- ^ ISBN 978-1-4212-1387-3.
- ^ PMID 13670595.
- PMID 21603286.
- ^ PMID 17252293.
- PMID 20927758.
- ISBN 978-0-19-262515-1.
- PMID 4888283.
- S2CID 21258760.
- PMID 7559196.
- ISBN 9789350903520.
- ^ PMID 10650107.
- PMID 17905013.
- PMID 17127190.
- PMID 14986790.
- S2CID 6147693.
- S2CID 2347888.
- ^ PMID 14975967.
- PMID 17943900.
- ^ PMID 2294844.
- PMID 2930289.
- PMID 10381713.
- PMID 5646296.
- PMID 1584258.
