Vitamin K
| Vitamin K | |
|---|---|
B02BA | |
| Biological target | Gamma-glutamyl carboxylase |
| Clinical data | |
| Drugs.com | Medical Encyclopedia |
| External links | |
| MeSH | D014812 |
| Legal status | |
| In Wikidata | |
Vitamin K is a family of structurally similar,
Vitamin K is used in the liver as the intermediate VKH2 to deprotonate a
Chemically, the vitamin K family comprises 2-
Vitamin K1 is made by plants, and is found in highest amounts in
Definition
Vitamin K refers to structurally similar, fat-soluble vitamers found in foods and marketed as dietary supplements. "Vitamin K" include several chemical compounds. These are similar in structure in that they share a quinone ring, but differ in the length and degree of saturation of the carbon tail and the number of repeating isoprene units in the side chain (see figures in Chemistry section). Plant-sourced forms are primarily vitamin K1. Animal-sourced foods are primarily vitamin K2.[1][6][7] Vitamin K has several roles: an essential nutrient absorbed from food, a product synthesized and marketed as part of a multi-vitamin or as a single-vitamin dietary supplement, and a prescription medication for specific purposes.[1]
Dietary recommendations
The US
In the European Union, adequate intake is defined the same way as in the US. For women and men over age 18 the adequate intake is set at 70 μg/day, for pregnancy 70 μg/day, and for lactation 70 μg/day. For children ages 1–17 years, adequate intake values increase with age from 12 to 65 μg/day.[8] Japan set adequate intakes for adult women at 65 μg/day and for men at 75 μg/day.[9] The European Union and Japan also reviewed safety and concluded – as had the United States – that there was insufficient evidence to set an upper limit for vitamin K.[9][10]
For US food and dietary supplement labeling purposes, the amount in a serving is expressed as a percentage of daily value. For vitamin K labeling purposes, 100% of the daily value was 80 μg, but on 27 May 2016 it was revised upwards to 120 μg, to bring it into agreement with the highest value for adequate intake.
Fortification
According to the Global Fortification Data Exchange, vitamin K deficiency is so rare that no countries require that foods be fortified.[15] The World Health Organization does not have recommendations on vitamin K fortification.[16]
Sources
Vitamin K1 is primarily from plants, especially leafy green vegetables. Small amounts are provided by animal-sourced foods. Vitamin K2 is primarily from animal-sourced foods, with poultry and eggs much better sources than beef, pork or fish.[7] One exception to the latter is nattō, which is made from bacteria-fermented soybeans. It is a rich food source of vitamin K2 variant MK-7, made by the bacteria.[17]
Vitamin K1
| Plant-sourced[7] | Amount K1 (μg / measure) |
|---|---|
| Collard greens boiled, drained, 1⁄2 cup | 530 |
| Spinach boiled, drained, 1⁄2 cup | 445 |
Turnip greens boiled, drained, 1⁄2 cup |
425 |
| Spinach raw, 1 cup | 145 |
| Brussels sprouts boiled, drained, 1⁄2 cup | 110 |
| Kale raw, 1 cup | 82 |
| Broccoli boiled, drained, 1⁄2 cup | 81 |
| Asparagus boiled, drained, 4 spears | 48 |
| Kiwifruit peeled, sliced, 1⁄2 cup | 36 |
| Chinese cabbage cooked, 1⁄2 cup | 29 |
Blueberries frozen, 1⁄2 cup |
21 |
| Plant-sourced[7] | Amount K1 (μg / measure) |
|---|---|
Hazelnuts chopped, 1 cup |
16 |
Grapes , 1⁄2 cup |
11 |
| Tomato products, 1 cup | 9.2 |
| Olive oil, 1.0 tablespoon | 8.1 |
| Zucchini boiled, drained, 1.0 cup | 7.6 |
| Mango pieces, 1.0 cup | 6.9 |
| Pears, pieces, 1.0 cup | 6.2 |
| Potato baked, including skin, one | 6.0 |
| Sweet potato baked, one | 2.6 |
| Bread whole wheat, 1 slice | 2.5 |
| Bread white, 1 slice | 2.2 |
Vitamin K2
Animal-sourced foods are a source of vitamin K2.[19][20] The MK-4 form is from conversion of plant-sourced vitamin K1 in various tissues in the body.[21]
| Animal Source[19] | Amount K2 MK-4 to MK-7 (μg / 100 g) |
|---|---|
| Goose | 31 |
| Chicken | 8.9 |
| Pork | 2.1 |
| Beef | 1.1 |
| Salmon | 0.5 |
Egg yolk |
32 |
| Egg white | 0.9 |
Vitamin K deficiency
Because vitamin K aids mechanisms for blood clotting, its deficiency may lead to reduced blood clotting, and in severe cases, can result in reduced clotting, increased bleeding, and increased prothrombin time.[2][5]
Normal diets are usually not deficient in vitamin K, indicating that deficiency is uncommon in healthy children and adults.[4] An exception may be infants who are at an increased risk of deficiency regardless of the vitamin status of the mother during pregnancy and breast feeding due to poor transfer of the vitamin to the placenta and low amounts of the vitamin in breast milk.[18]
Secondary deficiencies can occur in people who consume adequate amounts, but have malabsorption conditions, such as cystic fibrosis or chronic pancreatitis, and in people who have liver damage or disease.[2] Secondary vitamin K deficiency can also occur in people who have a prescription for a vitamin K antagonist drug, such as warfarin.[2][4] A drug associated with increased risk of vitamin K deficiency is cefamandole, although the mechanism is unknown.[22]
Medical uses

Treating vitamin deficiency in newborns
Vitamin K is given as an injection to newborns to prevent vitamin K deficiency bleeding.[18] The blood clotting factors of newborn babies are roughly 30–60% that of adult values; this appears to be a consequence of poor transfer of the vitamin across the placenta, and thus low fetal plasma vitamin K.[18] Occurrence of vitamin K deficiency bleeding in the first week of the infant's life is estimated at between 1 in 60 and 1 in 250[23].
Bleeding in infants due to vitamin K deficiency can be severe, leading to hospitalization,
Managing warfarin therapy
Warfarin is an anticoagulant drug. It functions by inhibiting an enzyme that is responsible for recycling vitamin K to a functional state. As a consequence, proteins that should be modified by vitamin K are not, including proteins essential to blood clotting, and are thus not functional.[25] The purpose of the drug is to reduce risk of inappropriate blood clotting, which can have serious, potentially fatal consequences.[2] The proper anticoagulant action of warfarin is a function of vitamin K intake and drug dose. Due to differing absorption of the drug and amounts of vitamin K in the diet, dosing must be monitored and customized for each patient.[26] Some foods are so high in vitamin K1 that medical advice is to avoid those (examples: collard greens, spinach, turnip greens) entirely, and for foods with a modestly high vitamin content, keep consumption as consistent as possible, so that the combination of vitamin intake and warfarin keep the anti-clotting activity in the therapeutic range.[27]
Vitamin K is a treatment for bleeding events caused by overdose of the drug.
Treating rodenticide poisoning
Methods of assessment
An increase in prothrombin time, a coagulation assay, has been used as an indicator of vitamin K status, but it lacks sufficient sensitivity and specificity for this application.[35] Serum phylloquinone is the most commonly used marker of vitamin K status. Concentrations <0.15 µg/L are indicative of deficiency. Disadvantages include exclusion of the other vitamin K vitamers and interference from recent dietary intake.[35] Vitamin K is required for the gamma-carboxylation of specific glutamic acid residues within the Gla domain of the 17 vitamin K–dependent proteins. Thus, a rise in uncarboxylated versions of these proteins is an indirect but sensitive and specific marker for vitamin K deficiency. If uncarboxylated prothrombin is being measured, this "Protein induced by Vitamin K Absence/antagonism (PIVKA-II)" is elevated in vitamin K deficiency.
The test is used to assess risk of vitamin K–deficient bleeding in newborn infants.
Side effects
No known toxicity is associated with high oral doses of the vitamin K1 or vitamin K2 forms of vitamin K, so regulatory agencies from US, Japan and European Union concur that no
Non-human uses
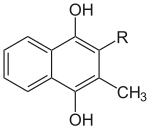
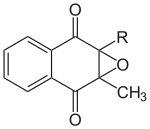
Menadione, a natural
Chemistry

The structure of phylloquinone, Vitamin K1, is marked by the presence of a

Conversion of vitamin K1 to vitamin K2
In animals, the MK-4 form of vitamin K2 is produced by conversion of vitamin K1 in the
Physiology
In animals, vitamin K is involved in the
17 human proteins with Gla domains have been discovered; they play key roles in the regulation of three physiological processes:
- Bone metabolism: osteocalcin, matrix Gla protein (MGP),[51] periostin,[52] and Gla-rich protein.[53][54]
- Vascular biology: Matrix Gla protein, growth arrest – specific protein 6 (Gas6)[55]
- Unknown functions: proline-rich γ-carboxyglutamyl proteins 1 and 2, and transmembrane γ-carboxy glutamyl proteins 3 and 4.[56]
Absorption
Vitamin K is absorbed through the jejunum and ileum in the small intestine. The process requires bile and pancreatic juices. Estimates for absorption are on the order of 80% for vitamin K1 in its free form (as a dietary supplement) but much lower when present in foods. For example, the absorption of vitamin K from kale and spinach – foods identified as having a high vitamin K content – are on the order of 4% to 17% regardless of whether raw or cooked.[4] Less information is available for absorption of vitamin K2 from foods.[4][5]
The intestinal membrane protein Niemann–Pick C1-like 1 (NPC1L1) mediates cholesterol absorption. Animal studies show that it also factors into absorption of vitamins E and K1.[57] The same study predicts potential interaction between SR-BI and CD36 proteins as well.[57] The drug ezetimibe inhibits NPC1L1 causing a reduction in cholesterol absorption in humans, and in animal studies, also reduces vitamin E and vitamin K1 absorption. An expected consequence would be that administration of ezetimibe to people who take warfarin (a vitamin K antagonist) would potentiate the warfarin effect. This has been confirmed in humans.[57]
Biochemistry
Function in animals
This section is missing information about invertebrates. (January 2021) |

Vitamin K is distributed differently within animals depending on its specific homologue. Vitamin K1 is mainly present in the liver, heart and pancreas, while MK-4 is better represented in the kidneys, brain and pancreas. The liver also contains longer chain homologues MK-7 to MK-13.[58]
The function of vitamin K2 in the animal cell is to add a
Within the cell, vitamin K participates in a cyclic process. The vitamin undergoes electron reduction to a reduced form called vitamin K hydroquinone (quinol), catalyzed by the enzyme vitamin K epoxide reductase (VKOR).[60] Another enzyme then oxidizes vitamin K hydroquinone to allow carboxylation of Glu to Gla; this enzyme is called gamma-glutamyl carboxylase[61] or the vitamin K–dependent carboxylase. The carboxylation reaction only proceeds if the carboxylase enzyme is able to oxidize vitamin K hydroquinone to vitamin K epoxide at the same time. The carboxylation and epoxidation reactions are said to be coupled. Vitamin K epoxide is then restored to vitamin K by VKOR. The reduction and subsequent reoxidation of vitamin K coupled with carboxylation of Glu is called the vitamin K cycle.[62] Humans are rarely deficient in vitamin K because, in part, vitamin K2 is continuously recycled in cells.[63]
Gamma-carboxyglutamate proteins
The following human Gla-containing proteins ("Gla proteins") have been characterized to the level of primary structure: blood coagulation factors II (
Gla proteins are known to occur in a wide variety of vertebrates: mammals, birds, reptiles, and fish. The venom of a number of Australian snakes acts by activating the human blood-clotting system. In some cases, activation is accomplished by snake Gla-containing enzymes that bind to the endothelium of human blood vessels and catalyze the conversion of procoagulant clotting factors into activated ones, leading to unwanted and potentially deadly clotting.[64]
Another interesting class of invertebrate Gla-containing proteins is synthesized by the fish-hunting snail
Function in plants and cyanobacteria
Vitamin K1 is an important chemical in green plants (including land plants and green algae) and some species of cyanobacteria, where it functions as an electron acceptor transferring one electron in photosystem I during photosynthesis.[67] For this reason, vitamin K1 is found in large quantities in the photosynthetic tissues of plants (green leaves, and dark green leafy vegetables such as romaine lettuce, kale, and spinach), but it occurs in far smaller quantities in other plant tissues.[7][67]
Detection of VKORC1 homologues active on the K1-epioxide suggest that K1 may have a non-redox function in these organisms. In plants but not cyanobacteria, knockout of this gene show growth restriction similar to mutants lacking the ability to produce K1.[68]
Function in other bacteria
Many bacteria, including
Some of these reactions generate a cellular energy source,
History
In 1929, Danish scientist
For several decades, the vitamin K–deficient chick model was the only method of quantifying vitamin K in various foods: the chicks were made vitamin K–deficient and subsequently fed with known amounts of vitamin K–containing food. The extent to which blood coagulation was restored by the diet was taken as a measure for its vitamin K content. Three groups of physicians independently found this: Biochemical Institute, University of Copenhagen (Dam and Johannes Glavind), University of Iowa Department of Pathology (Emory Warner, Kenneth Brinkhous, and Harry Pratt Smith), and the Mayo Clinic (Hugh Butt, Albert Snell, and Arnold Osterberg).[76]
The first published report of successful treatment with vitamin K of life-threatening hemorrhage in a jaundiced patient with prothrombin deficiency was made in 1938 by Smith, Warner, and Brinkhous.[77]
The precise function of vitamin K was not discovered until 1974, when
Research
Osteoporosis
Vitamin K is required for the gamma-carboxylation of
Cardiovascular health
Matrix Gla protein is a vitamin K-dependent protein found in bone, but also in soft tissues such as arteries, where it appears to function as an anti-calcification protein. In animal studies, animals that lack the gene for MGP exhibit calcification of arteries and other soft tissues.
In
Other
Population studies suggest that vitamin K status may have roles in inflammation, brain function, endocrine function and an anti-cancer effect. For all of these, there is not sufficient evidence from intervention trials to draw any conclusions.[4] From a review of observational trials, long-term use of vitamin K antagonists as anticoagulation therapy is associated with lower cancer incidence in general.[91] There are conflicting reviews as to whether agonists reduce the risk of prostate cancer.[92][93]
References
- ^ a b c "Fact Sheet for Health Professionals – Vitamin K". US National Institutes of Health, Office of Dietary Supplements. June 2020. Retrieved 26 August 2020.
- ^ a b c d e f g h "Vitamin K". Corvallis, OR: Micronutrient Information Center, Linus Pauling Institute, Oregon State University. July 2014. Retrieved 20 March 2017.
- S2CID 207573643.
- ^ ISBN 978-0-323-66162-1.
- ^ PMID 25057538.
- ^ "Nutrition facts, calories in food, labels, nutritional information and analysis". Nutritiondata.com. 13 February 2008. Retrieved 21 April 2013.
- ^ a b c d e f "USDA National Nutrient Database for Standard Reference Legacy: Vitamin K" (PDF). U.S. Department of Agriculture, Agricultural Research Service. 2018. Retrieved 27 September 2020.
- ^ "Overview on Dietary Reference Values for the EU population as derived by the EFSA Panel on Dietetic Products, Nutrition and Allergies" (PDF). 2017.
- ^ PMID 18460442.
- ^ a b "Tolerable Upper Intake Levels For Vitamins And Minerals" (PDF). European Food Safety Authority. 2006.
- ^ "Federal Register May 27, 2016 Food Labeling: Revision of the Nutrition and Supplement Facts Labels. FR page 33982" (PDF).
- ^ "Daily Value Reference of the Dietary Supplement Label Database (DSLD)". Dietary Supplement Label Database (DSLD). Archived from the original on 7 April 2020. Retrieved 16 May 2020.
- ^ "Changes to the Nutrition Facts Label". U.S. Food and Drug Administration (FDA). 27 May 2016. Retrieved 16 May 2020.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ "Industry Resources on the Changes to the Nutrition Facts Label". U.S. Food and Drug Administration (FDA). 21 December 2018. Retrieved 16 May 2020.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ^ "Map: Count of Nutrients in Fortification Standards". Global Fortification Data Exchange. Retrieved 3 September 2019.
- ^ Allen L, de Benoist B, Dary O, Hurrell R, Horton S (2006). "Guidelines on food fortification with micronutrients" (PDF). World Health Organization (WHO). Archived from the original (PDF) on 24 December 2006. Retrieved 3 September 2019.
- ^ S2CID 73427205.
- ^ S2CID 4499477.
- ^ S2CID 84592720.
- ^ PMID 16417305.
- ^ S2CID 7743991.
- PMID 16369967.
- ^ "What is Vitamin K Deficiency Bleeding?". 24 July 2023. Retrieved 18 April 2024.
{{cite web}}: CS1 maint: url-status (link) - PMID 27109090.
- ^ PMID 646989.
- ^ PMID 22114699.
- ^ National Institute of Health Clinical Center Drug-Nutrient Interaction Task Force. Archived from the original(PDF) on 5 April 2019. Retrieved 17 April 2015.
- ^ PMID 29203195.
- PMID 31573167.
- S2CID 43611422.
- ^ a b "Coumarin". PubChem, National Library of Medicine, US National Institutes of Health. 4 April 2019. Retrieved 13 April 2019.
- PMID 26255881.
- ^ Lung D (December 2015). Tarabar A (ed.). "Rodenticide Toxicity Treatment & Management". Medscape. WebMD.
- ^ Routt Reigart J, Roberts J (2013). Recognition and Management of Pesticide Poisonings: 6th Edition (PDF). p. 175.
- ^ S2CID 209435449.
- S2CID 59616051.
- ^ S2CID 162181757.
- PMID 28301903.
- PMID 24085302.
- .
- PMID 5867645.
- S2CID 94291300.
- ISSN 0021-9258.
- PMID 5910960.
- PMID 9446847.
- PMID 7947656.
- PMID 1453219.
- PMID 24489112.
- PMID 10068650.
- S2CID 38487783.
- PMID 3060178.
- PMID 18450759.
- PMID 18836183.
- PMID 19893032.
- S2CID 13383158.
- PMID 17502622.
- ^ PMID 28100881.
- PMID 29263734.
- ^ a b "Gamma-carboxyglutamic acid-rich (GLA) domain (IPR000294) < InterPro < EMBL-EBI". www.ebi.ac.uk. Retrieved 22 December 2015.
- PMID 16677080.
- S2CID 27634025.
- S2CID 19814205.
- ISBN 978-1-118-06572-3.
- PMID 12403650.
- PMID 14715910.
- S2CID 25647743.
- ^ PMID 27337968.
- ISBN 9780123858535.
- PMID 6127606.
- ^ PMID 140652.
- doi:10.1038/135652b0.
- (PDF). Nobel Prize Laureate Lecture.
- PMID 17330453. Archived from the original(PDF) on 6 March 2010.
- .
- .
- Dam CP (12 December 1946). "The discovery of vitamin K, its biological functions and therapeutical application"(PDF). Nobel Prize lecture.
- S2CID 87870462.
- PMID 4528109.
- ^ PMID 24090644.
- PMID 30511289.
- S2CID 149445288.
- PMID 28445289.
- S2CID 1244954.
- PMID 15514282.
- PMID 30717170.
- PMID 26770129.
- PMID 19179058.
- S2CID 53037302.
- PMID 32359159.
- PMID 32977548.
- S2CID 197421591.
- PMID 30544443.
- S2CID 52339455. Archived from the original(PDF) on 17 April 2021. Retrieved 13 October 2020.
Further reading
- "Vitamin K: Another Reason to Eat Your Greens" (PDF). Agricultural Research. 48 (1). January 2000. ISSN 2169-8244.
External links
- Vitamin K: CID 5280483 from PubChem
- Vitamin K1 (phylloquinone, phytomenadione): CID 5284607 from PubChem
- Vitamin K2 (menaquinone 6): CID 5283547 from PubChem
- Vitamin K3 (menadione): CID 4055 from PubChem