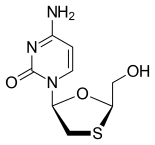
Lamivudine
 | |
| Clinical data | |
|---|---|
| Trade names | Epivir, Epivir-HBV, Zeffix, others[1] |
| Other names | (−)-L-2′,3′-dideoxy-3′-thiacytidine |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a696011 |
| License data |
|
| Pregnancy category |
|
| Routes of administration | By mouth |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | 86% |
| Protein binding | Less than 36% |
| Elimination half-life | 5 to 7 hours |
| Excretion | Kidney (circa 70%) |
| Identifiers | |
| |
JSmol) | |
| |
| |
| | |
Lamivudine, commonly called 3TC, is an
Common side effects include nausea, diarrhea, headaches,
Lamivudine was patented in 1995 and approved for use in the United States in 1995.
Medical uses
Lamivudine (Epivir) is indicated in combination with other antiretroviral agents for the treatment of HIV‑1 infection.[4][6] Lamivudine (Epivir HBV) is indicated for the treatment of chronic hepatitis B virus infection associated with evidence of hepatitis B viral replication and active liver inflammation.[5][7]
Lamivudine has been used for treatment of chronic hepatitis B at a lower dose than for treatment of HIV/AIDS. It improves the seroconversion of e-antigen positive hepatitis B and also improves histology staging of the liver. Long-term use of lamivudine leads to emergence of a resistant hepatitis B virus (YMDD) mutant.[11] Despite this, lamivudine is still used widely as it is well tolerated.[12]
Resistance
In HIV, high level resistance is associated with the M184V/I mutation in the
In hepatitis B, lamivudine resistance was first described in the YMDD (
Side effects
- Minor side effects may include .
- Do not prescribe lamivudine/zidovudine, abacavir/lamivudine, or abacavir/lamivudine/zidovudine to patients taking emtricitabine.
- Long-term use of lamivudine can trigger a resistant hepatitis B virus (YMDD) mutant.
- HIV or HBV-infected women on lamivudine are warned to discontinue breastfeeding as this puts the baby at risk for HIV transmission and medication side effects.
- Patients who are infected with HIV and HCV and are on both interferon and lamivudine can experience liver damage.
- The drug can trigger an Pneumocystisjirovecii [formerly P. carinii).
- antiretroviraltherapy.
- Use with caution for patients with impaired renal function and do not prescribe this treatment to patients with impaired liverfunction.
Mechanism of action
Lamivudine is an
Lamivudine is administered by mouth, and it is rapidly absorbed with a bio-availability of over 80%. Some research suggests that lamivudine can cross the blood–brain barrier. Lamivudine is often given in combination with zidovudine, with which it is highly synergistic. Lamivudine treatment has been shown to restore zidovudine sensitivity of previously resistant HIV. Lamivudine showed no evidence of carcinogenicity or mutagenicity in in vivo studies in mice and rats at doses from 10 to 58 times those used in humans.[4]
It has a half-life of 5–7 hours in adults and 2 hours in children.[medical citation needed]
History
Racemic BCH-189 (the minus form is known as lamivudine) was invented by Bernard Belleau while at work at McGill University and Paul Nguyen-Ba at the Montreal-based IAF BioChem International, Inc. laboratories in 1988 and the minus enantiomer isolated in 1989. Samples were first sent to Yung-Chi Cheng of Yale University for study of its toxicity.[16] When used in combination with AZT, he discovered that lamivudine's negative form reduced side effects and increased the drug's efficiency at inhibiting reverse transcriptase.[17] The combination of lamivudine and AZT increased the efficiency at inhibiting an enzyme HIV uses to reproduce its genetic material. As a result, lamivudine was identified as a less toxic agent to mitochondria DNA than other retroviral drugs.[18][19]
Lamivudine was approved by the US Food and Drug Administration (FDA) in November 1995, for use with zidovudine (AZT) and again in 2002. It is on the World Health Organization's List of Essential Medicines.[10]
Formulations
- Epivir tablets (GlaxoSmithKline; US and UK) for the treatment of HIV
- Epivir-HBV tablets (GlaxoSmithKline; US only) for the treatment of hepatitis B
- Zeffix tablets (GlaxoSmithKline; UK only) for the treatment of hepatitis B
- 3TC tablets (GlaxoSmithKline; South Africa) for the treatment of HIV
- 3TC-HBV tablets (GlaxoSmithKline; Indonesia) for the treatment of hepatitis B
- Lamivudine is available in fixed-dose combinationswith other HIV drugs such as:
- Lamivudine/zidovudine (with zidovudine)
- Abacavir/lamivudine (with abacavir)
- Abacavir/lamivudine/zidovudine (with zidovudine and abacavir)
- Dolutegravir/lamivudine (with dolutegravir)
References
- ^ a b c d e f g h i j k l m "Lamivudine". The American Society of Health-System Pharmacists. Archived from the original on 2 June 2016. Retrieved 31 July 2016.
- FDA. Retrieved 22 October 2023.
- ^ "3TC (lamivudine, Epivir)". Catie. 2014. Retrieved 22 August 2022.
- ^ a b c "Epivir- lamivudine tablet, film coated Epivir- lamivudine solution". DailyMed. 1 August 2020. Retrieved 28 November 2020.
- ^ a b "Epivir HBV- lamivudine tablet, film coated Epivir HBV- lamivudine solution". DailyMed. 17 August 2020. Retrieved 28 November 2020.
- ^ a b "Epivir EPAR". European Medicines Agency (EMA). 17 September 2018. Retrieved 29 November 2020.
- ^ a b "Zeffix EPAR". European Medicines Agency (EMA). 17 September 2018. Retrieved 28 November 2020.
- ISBN 9783662467596. Archivedfrom the original on 15 August 2016.
- ISBN 9783527607495.
- ^ hdl:10665/325771. WHO/MVP/EMP/IAU/2019.06. License: CC BY-NC-SA 3.0 IGO.
- S2CID 35040816.
- PMID 25937866.
- S2CID 25783477.
- ^ "Index". Archived from the original on 1 July 2010. Retrieved 23 July 2010. Stanford University Drug Resistance Database.
- PMID 17409326.
- ^ "Hunting Down HIV".
- ^ "US Patent Office" (PDF). Archived (PDF) from the original on 16 June 2016.
- ^ Soderstrom J (2003). "National Institutes of Health: Moving Research from the Bench to the Bedside". Archived from the original on 4 March 2016.
- ^ Gilden D (2000). "The Wide-Ranging Effects of Nucleoside Analogs:A Look at Mitochondrial Toxicity". Archived from the original on 16 September 2016.
