Atrial fibrillation
| Atrial fibrillation | |
|---|---|
| Other names | Auricular fibrillation Irregular heartbeat[9] |
| Treatment | Lifestyle modifications, rate control, rhythm control, anticoagulation[5] |
| Frequency | 2.5% (developed world), 0.5% (developing world)[4] |
| Deaths | 315,000 with atrial flutter (2019)[10] |
Atrial fibrillation (AF, AFib or A-fib) is an
Episodes can be asymptomatic.
Other risk factors include excess
Healthy lifestyle changes, such as weight loss in people with obesity, increased physical activity, and drinking less
Atrial fibrillation is the most common serious abnormal heart rhythm and, as of 2020, affects more than 33 million people worldwide.
Signs and symptoms

AF is usually accompanied by symptoms related to a rapid heart rate. Rapid and irregular heart rates may be perceived as
Since most cases of AF are secondary to other medical problems, the presence of
Rapid heart rate
Presentation is similar to other forms of rapid heart rate and may be asymptomatic. Palpitations and chest discomfort are common complaints. The rapid uncoordinated heart rate may result in reduced output of blood pumped by the heart (cardiac output), resulting in inadequate blood flow, and therefore oxygen delivery to the rest of the body. Common symptoms of uncontrolled atrial fibrillation may include shortness of breath, shortness of breath when lying flat, dizziness, and sudden onset of shortness of breath during the night. This may progress to swelling of the lower extremities, a manifestation of congestive heart failure. Due to inadequate cardiac output, individuals with AF may also complain of lightheadedness.[26]
AF can cause
Causes
AF is linked to several forms of cardiovascular disease but may occur in otherwise normal hearts. Cardiovascular factors known to be associated with the development of AF include
Additionally, lung diseases (such as
Genetics
This Genetics section may be too technical for most readers to understand. (April 2023) |
A family history of AF may increase the risk of AF. A study of more than 2,200 people found an increased risk factor for AF of 1.85 for those that had at least one parent with AF.[43][44][45] Various genetic mutations may be responsible.[46][47]
Four types of genetic disorder are associated with atrial fibrillation:[48]
- Familial AF as a monogenic disease
- Familial AF presenting in the setting of another inherited cardiac disease (hypertrophic cardiomyopathy, familial amyloidosis)
- Inherited arrhythmic syndromes (congenital long QT syndrome, short QT syndrome, Brugada syndrome)
- Non-familial AF associated with genetic backgrounds (polymorphism in the ACE gene) that may predispose to atrial fibrillation
Family history in a first degree relative is associated with a 40% increase in risk of AF. This finding led to the
Sedentary lifestyle
A
Tobacco
The rate of AF in smokers is 1.4 times higher than in non-smokers.[61] However, snus consumption, which delivers nicotine at a dose equivalent to that of cigarettes and is debated as a harm-reduction product, is not correlated with AF.[62]
Alcohol
Acute alcohol consumption can directly trigger an episode of atrial fibrillation.
High blood pressure
According to the CHARGE Consortium, both systolic and diastolic
Other diseases
There is a relationship between risk factors such as
Medications
Several medications are associated with an increased risk of developing atrial fibrillation.[63] Few studies have examined this phenomenon, and the exact incidence of medication-induced atrial fibrillation is unknown.[63] Medications that are commonly associated with an increased risk of developing atrial fibrillation include dobutamine and the chemotherapy agent cisplatin.[63] Agents associated with a moderately increased risk include nonsteroidal anti-inflammatory drugs (e.g., ibuprofen), bisphosphonates, and other chemotherapeutic agents such as melphalan, interleukin 2, and anthracyclines.[63] Other medications that rarely increase the risk of developing atrial fibrillation include adenosine, aminophylline, corticosteroids, ivabradine, ondansetron, and antipsychotics.[63] This form of atrial fibrillation occurs in people of all ages but is most common in the elderly, in those with other atrial fibrillation risk factors, and after heart surgery.[63]
Pathophysiology
The normal
Pathology
The primary pathologic change seen in atrial fibrillation is the progressive fibrosis of the atria. This fibrosis is due primarily to atrial dilation; however, genetic causes and inflammation may be factors in some individuals. Dilation of the atria can be due to almost any structural abnormality of the heart that can cause a rise in the pressure within the heart. This includes valvular heart disease (such as mitral stenosis, mitral regurgitation, and tricuspid regurgitation), hypertension, and congestive heart failure. Any inflammatory state that affects the heart can cause fibrosis of the atria. This is typically due to sarcoidosis but may also be due to autoimmune disorders that create autoantibodies against myosin heavy chains. Mutation of the lamin AC gene is also associated with fibrosis of the atria that can lead to atrial fibrillation.[citation needed]
Once dilation of the atria has occurred, this begins a chain of events that leads to the activation of the
Fibrosis is not limited to the muscle mass of the atria and may occur in the
Along with fibrosis, alterations in the atria that predispose to atrial fibrillation affect their
Electrophysiology
| Conduction | ||
Sinus rhythm  |
Atrial fibrillation 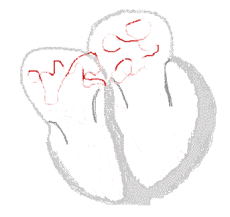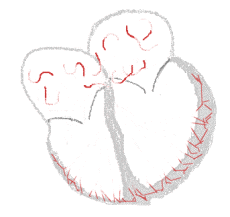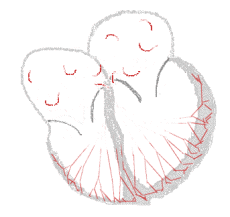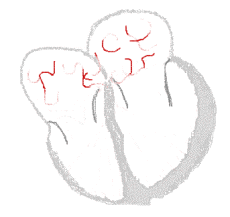 | |
There are multiple theories about the cause of atrial fibrillation. An important theory is that the regular impulses produced by the sinus node for a normal heartbeat are overwhelmed by rapid electrical discharges produced in the atria and adjacent parts of the
In a heart with AF, the increased calcium release from the
AF can be distinguished from
Although the electrical impulses of AF occur at a high rate, most of them do not result in a heartbeat. A heartbeat results when an electrical impulse from the atria passes through the atrioventricular (AV) node to the ventricles and causes them to contract. During AF, if all of the impulses from the atria passed through the AV node, there would be severe ventricular tachycardia, resulting in a severe reduction of cardiac output. This dangerous situation is prevented by the AV node since its limited conduction velocity reduces the rate at which impulses reach the ventricles during AF.[67]
Diagnosis

The evaluation of atrial fibrillation involves a determination of the cause of the arrhythmia, and classification of the arrhythmia. Diagnostic investigation of AF typically includes a complete history and physical examination, ECG,
Screening
Numerous guidelines recommend opportunistic screening for atrial fibrillation in those 65 years and older. These organizations include the: European Society of Cardiology,[69] National Heart Foundation of Australia and the Cardiac Society of Australia and New Zealand[70] European Heart Rhythm Society,[71][72] AF-SCREEN International Collaboration,[73] Royal College of Physicians of Edinburgh[74] European Primary Care Cardiovascular Society,[75] and Irish Health Information and Quality Authority.[76]
Single timepoint screening detects undiagnosed AF, which is often asymptomatic, in approximately 1.4% of people in this age group.[77] A Scottish inquiry into atrial fibrillation estimated that as many as one-third of people with AF are undiagnosed. Despite this, in 2018, the United States Preventive Services Task Force found insufficient evidence to determine the usefulness of routine screening.[78] Given the importance of having a pathway to treatment, general practice is potentially an ideal setting to conduct AF screening. General practice was identified as a 'preferred' setting for AF screening by the AF-SCREEN international collaboration report due to the availability of nursing support and the natural pathway to treatment.[73] Screening in primary care has been trialled in a number of countries. These include: a recent Canadian study conducted in 184 general practices;[79] a screening program conducted alongside influenza vaccinations in 10 Dutch practices;[80] and several Australian studies showed that opportunistic screening in primary care by GPs and nurses using eHealth tools was feasible.[81][82][83][84]
Minimal evaluation
In general, the minimal evaluation of atrial fibrillation should be performed in all individuals with AF. The goal of this evaluation is to determine the general treatment regimen for the individual. If the results of the general evaluation warrant it, further studies may then be performed.[citation needed]
History and physical examination
The history of the individual's atrial fibrillation episodes is probably the most important part of the evaluation. Distinctions should be made between those who are entirely asymptomatic when they are in AF (in which case the AF is found as an incidental finding on an ECG or physical examination) and those who have gross and obvious symptoms due to AF and can pinpoint whenever they go into AF or revert to sinus rhythm.[citation needed]
Routine bloodwork
While many cases of AF have no definite cause, it may be the result of various other problems. Hence,
In acute-onset AF associated with
Electrocardiogram

Atrial fibrillation is diagnosed on an electrocardiogram (ECG), an investigation performed routinely whenever an irregular heartbeat is suspected. Characteristic findings are the absence of P waves, with disorganized electrical activity in their place, and irregular R–R intervals due to irregular conduction of impulses to the ventricles.[23] At very fast heart rates, atrial fibrillation may look more regular, which may make it more difficult to separate from other supraventricular tachycardias or ventricular tachycardia.[85]
If paroxysmal AF is suspected, but an ECG during an office visit shows only a regular rhythm, AF episodes may be detected and documented with the use of ambulatory
Echocardiography
In general, a non-invasive transthoracic
Significant enlargement of both the left and right atria is associated with long-standing atrial fibrillation and, if noted at the initial presentation of atrial fibrillation, suggests that the atrial fibrillation is likely to be of a longer duration than the individual's symptoms.[citation needed]
Extended evaluation
In general, an extended evaluation is not necessary for most individuals with atrial fibrillation and is performed only if abnormalities are noted in the limited evaluation, if a reversible cause of the atrial fibrillation is suggested, or if further evaluation may change the treatment course.
Chest X-ray
In general, a
Transesophageal echocardiogram
A regular echocardiogram (transthoracic echo/TTE) has a low sensitivity for identifying blood clots in the heart. If this is suspected (e.g., when planning urgent electrical cardioversion), a transesophageal echocardiogram/TEE (or TOE where British spelling is used) is preferred.[23]
The TEE has much better visualization of the
If a blood clot is seen on TEE, then cardioversion is contraindicated due to the risk of stroke, and anticoagulation is recommended.
Ambulatory Holter monitoring
A Holter monitor is a wearable ambulatory heart monitor that continuously monitors the heart rate and heart rhythm for a short duration, typically 24 hours. In individuals with symptoms of significant shortness of breath with exertion or palpitations regularly, a Holter monitor may be of benefit to determine whether rapid heart rates (or unusually slow heart rates) during atrial fibrillation are the cause of the symptoms.
Exercise stress testing
Some individuals with atrial fibrillation do well with normal activity but develop shortness of breath with exertion. It may be unclear whether the shortness of breath is due to a blunted heart rate response to exertion caused by excessive atrioventricular node-blocking agents, a very rapid heart rate during exertion, or other underlying conditions such as chronic lung disease or coronary ischemia. An exercise stress test will evaluate the individual's heart rate response to exertion and determine whether the AV node blocking agents are contributing to the symptoms.
Classification
| AF category | Defining characteristics |
|---|---|
| First detected | only one diagnosed episode |
| Paroxysmal | recurrent episodes that stop on their own in less than seven days |
| Persistent | recurrent episodes that last more than seven days |
| Longstanding Persistent | recurrent episodes that last more than twelve months |
| Permanent | AF that has been accepted, and for which a solely rate control strategy has been decided upon. |
The American College of Cardiology (ACC), American Heart Association (AHA), and the European Society of Cardiology (ESC) recommend in their guidelines the following classification system based on simplicity and clinical relevance.[21]
All people with AF are initially in the category called first detected AF. These people may or may not have had previous undetected episodes. If a first detected episode stops on its own in less than seven days and then another episode begins, later on, the category changes to paroxysmal AF. Although people in this category have episodes lasting up to seven days, in most cases of paroxysmal AF, the episodes will stop in less than 24 hours. If the episode lasts for more than seven days, it is unlikely to stop on its own and is then known as persistent AF. In this case, cardioversion can be attempted to restore a normal rhythm. If an episode continues for a year or more, the rhythm is then known as longstanding persistent AF. If a decision is made by the person and their medical team to accept persistent AF and not attempt restoration of a normal sinus rhythm but instead manage the AF by simply controlling the person's ventricular rate then the rhythm is referred to as permanent AF. As a further subtype, AF that is detected only by an implanted or wearable cardiac monitor is known as subclinical AF.[21]
Episodes that last less than 30 seconds are not considered in this classification system. Also, this system does not apply to cases where the AF is a secondary condition that occurs in the setting of a primary condition that may be the cause of the AF.
About half of people with AF have permanent AF, while a quarter have paroxysmal AF, and a quarter have persistent AF.[4]
In addition to the above AF categories, which are mainly defined by episode timing and termination, the ACC/AHA/ESC guidelines describe additional AF categories in terms of other characteristics of the person.
Prevention
Prevention of atrial fibrillation focuses primarily on preventing or controlling its risk factors. Many of its risk factors, such as
Lifestyle modification
Several healthy lifestyle behaviors are associated with a lower likelihood of developing atrial fibrillation. Accordingly, consensus guidelines recommend abstaining from alcohol and recreational drugs, stopping tobacco use, maintaining a healthy weight, and regularly participating in moderate-intensity physical activities.[63] Consistent moderate-intensity aerobic exercise, defined as achieving 3.0–5.9 METs of intensity, for at least 150 minutes per week may reduce the risk of developing new-onset atrial fibrillation.[17] Few studies have examined the role of specific dietary changes and how it relates to the prevention of atrial fibrillation.[63]
Management
The main goals of treatment are to prevent
This holistic or integrated care approach is summed up as the ABC (Atrial fibrillation Better Care) pathway,[96] as follows:
- A: Avoid stroke with Anticoagulation, where the default is stroke prevention unless the patient is at low risk. Stroke prevention means use of oral anticoagulation (OAC), whether with well managed vitamin K antagonists (VKA), with time in therapeutic range >70%, or more commonly, label-adherent dosed direct oral anticoagulant (DOAC).
- B: Better symptom and atrial fibrillation management with patient-centred, symptom directed decisions on rate control or rhythm control. In some selected patients, use early rhythm control may be beneficial.
- C: Cardiovascular risk factor and comorbidity management, including attention to lifestyle factors and psychological morbidity.
Lifestyle modification
Regular aerobic exercise improves atrial fibrillation symptoms and AF-related quality of life.[17] The effect of high-intensity interval training on reducing atrial fibrillation burden is unclear.[17] Weight loss of at least 10% is associated with reduced atrial fibrillation burden in people who are overweight or obese.[17]
Comorbidity treatment
For people who have both atrial fibrillation and obstructive sleep apnea, observational studies suggest that continuous positive airway pressure (CPAP) treatment appears to lower the risk of atrial fibrillation recurrence after undergoing ablation.[17] Randomized controlled trials examining the role of obstructive sleep apnea treatment on atrial fibrillation incidence and burden are lacking.[17] Guideline-recommended lifestyle and medical interventions are recommended for people with atrial fibrillation and coexisting conditions such as hyperlipidemia, diabetes mellitus, or hypertension without specific blood sugar or blood pressure targets for people with atrial fibrillation.[17]
Anticoagulants
Anticoagulation can be used to reduce the risk of stroke from AF. Anticoagulation is recommended in most people other than those at low risk of stroke[12][102] or those at high risk of bleeding. The risk of falls and consequent bleeding in frail elderly people should not be considered a barrier to initiating or continuing anticoagulation since the risk of fall-related brain bleeding is low and the benefit of stroke prevention often outweighs the risk of bleeding.[103][104] Similarly, the presence or absence of AF symptoms does not determine whether a person warrants anticoagulation and is not an indicator of stroke risk.[38] Oral anticoagulation is underused in atrial fibrillation, while aspirin is overused in many who should be treated with a direct oral anticoagulant (DOAC) or warfarin.[105][106][107] In 2019, DOACs were often recommended over warfarin by the American Heart Association.[108]
The risk of stroke from non-valvular AF can be estimated using the CHA2DS2-VASc score. In the 2019 AHA/ACC/HRS guidelines anticoagulation is recommended in non-valvular AF if there is a score of two or more in men and three or more in women and may be considered if there is a score of one in men or two in women; not using anticoagulation is reasonable if there is a score of zero in men or one in women.[108] Guidelines from the American College of Chest Physicians, Asia-Pacific Heart Rhythm Society, Canadian Cardiovascular Society, European Society of Cardiology, Japanese Circulation Society, Korean Heart Rhythm Society, and the National Institute for Health and Care Excellence recommend the use of novel oral anticoagulants or warfarin with a CHA2DS2-VASc score of one over aspirin and some directly recommend against aspirin.[107][109][110][111][112][113][114][115] Experts generally advocate for most people with atrial fibrillation with CHA2DS2-VASc scores of one or more receiving anticoagulation though aspirin is sometimes used for people with a score of one (moderate risk for stroke).[105] There is little evidence to support the idea that the use of aspirin significantly reduces the risk of stroke in people with atrial fibrillation.[105] Furthermore, aspirin's major bleeding risk (including bleeding in the brain) is similar to that of warfarin and DOACs despite its inferior efficacy.[106][116]
Anticoagulation can be achieved through several means including
For those with non-valvular atrial fibrillation, DOACs are at least as effective as warfarin for preventing strokes and blood clots
Warfarin is the recommended anticoagulant choice for persons with valvular atrial fibrillation (atrial fibrillation in the presence of a mechanical heart valve and/or moderate-severe mitral valve stenosis).
Rate versus rhythm control
There are two ways to approach atrial fibrillation using medications: rate control and rhythm control. Both methods have similar outcomes.[129] Rate control lowers the heart rate closer to normal, usually 60 to 100 bpm, without trying to convert to a regular rhythm. Rhythm control tries to restore a normal heart rhythm in a process called cardioversion and maintains the normal rhythm with medications. Studies suggest that rhythm control is more important in the acute setting AF, whereas rate control is more important in the chronic phase.
The risk of stroke appears to be lower with rate control versus attempted rhythm control, at least in those with heart failure.[130] AF is associated with a reduced quality of life, and, while some studies indicate that rhythm control leads to a higher quality of life, some did not find a difference.[131]
Neither rate nor rhythm control is superior in people with heart failure when they are compared in various clinical trials. However, rate control is recommended as the first-line treatment regimen for people with heart failure. On the other hand, rhythm control is only recommended when people experience persistent symptoms despite adequate rate control therapy.[132]
In those with a fast ventricular response, intravenous magnesium significantly increases the chances of achieving successful rate and rhythm control in the urgent setting without major side-effects.[133] A person with poor vital signs, mental status changes, preexcitation, or chest pain often will go to immediate treatment with synchronized DC cardioversion.[23] Otherwise, the decision of rate control versus rhythm control using medications is made. This is based on several criteria that include whether or not symptoms persist with rate control.
Rate control
Rate control to a
- Beta blockers (preferably the "cardioselective" beta blockers such as metoprolol, bisoprolol, or nebivolol)
- Non-dihydropyridine calcium channel blockers (e.g., diltiazem or verapamil)
Patients with chronic AF are recommended to take either beta blockers or calcium channel blockers.[134]
In addition to these agents, amiodarone has some AV node blocking effects (in particular when administered intravenously) and can be used in individuals when other agents are contraindicated or ineffective (particularly due to hypotension).
Cardioversion
Cardioversion is the attempt to switch an irregular heartbeat to a normal heartbeat using electrical or chemical means.[23]
- Electrical cardioversion involves the restoration of normal heart rhythm through the application of a DC electrical shock. The exact placement of the pads does not appear to be important.[137]
- Chemical cardioversion is performed with medications, such as amiodarone, dronedarone,[138] procainamide (especially in pre-excited atrial fibrillation), dofetilide, ibutilide, propafenone, or flecainide.
After successful cardioversion, the heart may be stunned, which means that there is a normal rhythm, but the restoration of normal atrial contraction has not yet occurred.[139]
Surgery
Ablation
Electrophysiologists generally use two forms of catheter ablation—
In general, CA is more successful at preventing AF recurrence if AF is paroxysmal as opposed to persistent .[144] As CA does not reduce the risk of stroke, many are advised to continue their anticoagulation.[141] Possible complications include common, minor complications such as the formation of a collection of blood at the site where the catheter goes into the vein (access site hematoma), but also more dangerous complications including bleeding around the heart (cardiac tamponade), stroke, damage to the esophagus (atrio-esophageal fistula), or even death.[141][145]
An alternative to catheter ablation is surgical ablation. The Maze procedure, first performed in 1987, is an effective invasive surgical treatment that is designed to create electrical blocks or barriers in the atria of the heart. The idea is to force abnormal electrical signals to move along one, uniform path to the lower chambers of the heart (ventricles), thus restoring the normal heart rhythm.[146] People with AF often undergo cardiac surgery for other underlying reasons and are frequently offered concomitant AF surgery to reduce the frequency of short- and long-term AF. Concomitant AF surgery is more likely to lead to the person being free from atrial fibrillation and off medications long-term after surgery and Cox-Maze IV procedure is the gold standard treatment. There is a slightly increased risk of needing a pacemaker following the procedure.[147][148][149]
AF often occurs after cardiac surgery and is usually self-limiting. It is strongly associated with age, preoperative hypertension, and the number of vessels grafted. Measures should be taken to control hypertension preoperatively to reduce the risk of AF. Also, people with a higher risk of AF, e.g., people with pre-operative hypertension, more than three vessels grafted, or greater than 70 years of age, should be considered for prophylactic treatment. Postoperative pericardial effusion is also suspected to be the cause of atrial fibrillation. Prophylaxis may include prophylactic postoperative rate and rhythm management. Some authors perform posterior pericardiotomy to reduce the incidence of postoperative AF.[150] When AF occurs, management should primarily be rate and rhythm control. However, cardioversion may be used if the patient is hemodynamically unstable, highly symptomatic, or AF persists for six weeks after discharge. In persistent cases, anticoagulation should be used.
Left atrial appendage occlusion
There is growing evidence that left atrial appendage occlusion therapy may reduce the risk of stroke in people with non-valvular AF as much as warfarin.[151][152]

After surgery
After catheter ablation, people are moved to a cardiac recovery unit, intensive care unit, or cardiovascular intensive care unit where they are not allowed to move for 4–6 hours. Minimizing movement helps prevent bleeding from the site of the catheter insertion. The length of time people stay in the hospital varies from hours to days. This depends on the problem, the length of the operation, and whether or not general anesthetic was used. Additionally, people should not engage in strenuous physical activity – to maintain a low heart rate and low blood pressure – for around six weeks.[153]
Prognosis
Atrial fibrillation can progress from infrequent occurrences to more frequent occurrences, ultimately becoming permanent.[154] But the majority of cases do not progress, especially among patients with a healthy lifestyle. [155]
Atrial fibrillation increases the risk of
Blood clots
Prediction of embolism
Among Danish men aged 50, with no risk factors, the 5-year risk of stroke was 1.1% and with AF alone 2.5%. For women the risks were slightly less, 0.7% and 2.1%. For men aged 70, the 5-year risk of stroke was 4.8% and with AF alone 6.8%. For women aged 70 the risk was again lower than for men, 3.4% with no added risk factor and 8.2% with AF.[159]
Determining the risk of an embolism causing a stroke is important for guiding the use of anticoagulants. The most accurate clinical prediction rules are:[12][160]
- CHADS2
- CHA2DS2-VASc score
Both the CHADS2 and the CHA2DS2-VASc score predict future stroke risk in people with A-fib with CHA2DS2-VASc score being more accurate. Some that had a CHADS2 score of zero had a CHA2DS2-VASc score of three, with a 3.2% annual risk of stroke. Thus, a CHA2DS2-VASc score of zero is considered very low risk.[161]
Mechanism of thrombus formation
In atrial fibrillation, the lack of an organized atrial contraction can result in some stagnant blood in the left atrium (LA) or
More than 90% of cases of thrombi associated with non-valvular atrial fibrillation evolve in the left atrial appendage.[87] However, the LAA lies in close relation to the free wall of the left ventricle, and thus the LAA's emptying and filling, which determines its degree of blood stagnation, may be helped by the motion of the wall of the left ventricle if there is good ventricular function.[162]
Dementia
Atrial fibrillation has been independently associated with a higher risk of developing
Epidemiology
Atrial fibrillation is the most common arrhythmia and affects more than 33 million people worldwide.[17][23] In Europe and North America, as of 2014[update], it affects about 2% to 3% of the population.[4] This is an increase from 0.4 to 1% of the population around 2005.[23] In the developing world, rates are about 0.6% for males and 0.4% for females.[4] The number of people diagnosed with AF has increased due to better detection of silent AF and increasing age and conditions that predispose to it.[166]
It also accounts for one-third of hospital admissions for cardiac rhythm disturbances,[23] and the rate of admissions for AF has risen in recent years.[167] AF is the cause for 20% to 30% of all ischemic strokes.[166] After a transient ischemic attack or stroke, about 11% are found to have a new diagnosis of atrial fibrillation.[168] 3% to 11% of patients with AF have structurally normal hearts.[169] Approximately 2.2 million individuals in the United States and 4.5 million in the European Union have AF.[23]
The number of new cases each year of AF increases with age. In people older than 80 years, it affects about 8%.
Gender
Atrial fibrillation is more common in men than in women when reviewed in European and North American populations.
Ethnicity
Rates of AF are lower in populations of African descent than in populations of European descent. African descent is associated with a protective effect for AF, due to the lower presence of
Young people
Atrial fibrillation is an uncommon condition in children but sometimes occurs in association with certain inherited and acquired conditions.
History
Because the diagnosis of atrial fibrillation requires measurement of the electrical activity of the heart, atrial fibrillation was not truly described until 1874, when
Other animals
Atrial fibrillation occurs in other animals, including cats, dogs, and horses.[182][183] Unlike humans, dogs rarely develop the complications that stem from blood clots breaking off from inside the heart and traveling through the arteries to distant sites (thromboembolic complications).[182] Cats rarely develop atrial fibrillation but appear to have a higher risk of thromboembolic complications than dogs.[182]
Cats and dogs with atrial fibrillation often have underlying structural heart disease that predisposes them to the condition.
References
- ^ "Atrial fibrillation or flutter: MedlinePlus Medical Encyclopedia". medlineplus.gov. Retrieved 28 May 2019.
- ^ ISBN 978-0-340-97425-4.
- ^ PMID 24474959.
- ^ PMID 24966695.
- ^ PMID 25443231.
- ^ PMID 23453870.
- ^ PMID 28450367.
- ^ PMID 24054541.
- ISBN 978-3-319-11821-5. Archivedfrom the original on 8 September 2017.
- PMID 37988383.
- ^ "Heart Disease Other Related Conditions". cdc.gov. 3 September 2014. Archived from the original on 14 February 2015. Retrieved 19 February 2015.
- ^ PMID 30480925.
Report No.: 18-EHC018-EFReport No.: 2018-SR-04
- ^ PMID 25838435.
- ISBN 978-1-107-68130-9. Archivedfrom the original on 8 September 2017.
- ^ PMID 23514988.
- PMID 36874560.
- ^ PMID 32148086.
- PMID 23369365.
- PMID 24182224.
- ^ S2CID 5578741.
- ^ PMID 32860505.
- PMID 24733535.
- ^ PMID 16908781.
- PMID 27733281.
- PMID 25530442.
- ^ from the original on 24 December 2013.
- ^ PMID 27185022.
- ^ S2CID 53213100.
- PMID 25498795.
- PMID 25951122.
- S2CID 25479450.
- S2CID 11129249.
- PMID 17276180.
- PMID 23877062.
- S2CID 2311111.
- PMID 24680173.
- ^ PMID 27931615.
- ^ PMID 25827359.
- PMID 28408027.
- S2CID 22065631.
- S2CID 2475456.
- ^ "Night shift work is linked to increased risk of heart problems". Escardio. Retrieved 16 August 2021.
- PMID 15199036.
- PMID 24932358.
- PMID 26229966.
- PMID 16790707.
- ^ "OMIM Online Mendelian Inheritance of Man". The National Center for Biotechnology Information. Archived from the original on 16 June 2013. Retrieved 24 August 2010.
- PMID 23631189.
- ^ PMID 28450367.
- PMID 16790700.
- PMID 25684755.
- ^ PMID 29892015.
- PMID 30333491.
- PMID 31691645.
- ^ Wren GH, Baker E, Underwood JFG, Humby T, Thompson AR, Kirov G, Escott-Price V, Davies W. (2022) Characterising heart rhythm abnormalities associated with Xp22.31 deletion Journal of Medical Genetics doi:10.1136/jmg-2022-108862 PMID 36379544 URL:https://jmg.bmj.com/content/early/2022/11/15/jmg-2022-108862
- PMID 21767729.
- ^ S2CID 206025944.
- PMID 19633305.
- PMID 20569734.
- ^ PMID 23537808.
- S2CID 24080017.
- ^ PMID 28175283.
- PMID 31768479.
- PMID 26835073.
- PMID 25880508.
- ISBN 978-0-7817-5030-1.
- PMID 36856589.
- PMID 32860505.
- PMID 30077228.
- PMID 26481149.
- PMID 29048522.
- ^ S2CID 207655707.
- PMID 22441062.
- PMID 25701017.
- ^ "Reports and Publications | HIQA". www.hiqa.ie.
- PMID 31553733.
- PMID 30088016.
- S2CID 132597318.
- PMID 26851813.
- PMID 30590964.
- PMID 27892421.
- PMID 24791776.
- PMID 32865129.
- ISBN 978-1-4160-5998-1. Archivedfrom the original on 8 September 2017.
- ^ S2CID 29114242.
- ^ PMID 8572814.
- PMID 26306127.
- ^ PMID 30703530.
- S2CID 205070036.
- PMID 31483500.
- PMID 34020488.
- S2CID 52114134.
- PMID 32370588.
- S2CID 54623946.
- S2CID 36013527.
- S2CID 207646320.
- S2CID 33841631.
- PMID 33206945.
- PMID 34333599.
- PMID 31893513.
- PMID 25988464.
- S2CID 34366717.
- ^ S2CID 3832073.
- ^ PMID 27825618.
- ^ S2CID 5578741.
- ^ PMID 28754397.
- ^ PMID 30686041.
- PMID 24965079.
- PMID 25653698.
- PMID 22315271.
- PMID 28765771.
- PMID 32860505.
- PMID 27609430.
- ^ "Atrial fibrillation: management". National Institute of Health Care and Excellence. 18 June 2014.
- PMID 27567408.
- PMID 23014814. Archived from the originalon 5 March 2016.
- ^ "FDA approves Xarelto to prevent stroke in people with common type of abnormal heart rhythm". FDA. Archived from the original on 5 November 2011. Retrieved 4 November 2011.
- ^ "FDA approves anti-clotting drug Savaysa". FDA. 8 January 2015. Archived from the original on 19 June 2016. Retrieved 23 June 2016.
- ^ "FDA approves Eliquis to reduce the risk of stroke, blood clots in patients with non-valvular atrial fibrillation". FDA. Archived from the original on 31 December 2012. Retrieved 30 December 2012.
- PMID 30383133.
- PMID 15383480.
- PMID 30413255.
- PMID 29747837.
- ^ PMID 25995317.
- ^ PMID 24455237.
- ISBN 978-1-4511-5396-5.
- S2CID 24988387.
- PMID 24887617.
- PMID 23418244.
- PMID 16651058.
- PMID 25125304.
Multiple studies have compared pharmacological rate and rhythm strategies but have failed to identify a superior therapy, a finding that extends to patients with HF. ... Antiarrhythmic drug therapy is indicated as first-line therapy for AF that remains symptomatic despite adequate rate control.
- PMID 17560883.
- ^ PMID 23558044.
- PMID 24507168.
- ^ "Atrial fibrillation: national clinical guideline for management in primary and secondary care" (PDF). National Collaborating Centre for Chronic Conditions. London: Royal College of Physicians. 2006. Archived from the original (PDF) on 22 May 2013. Retrieved 9 May 2009.
- S2CID 36859521.
- S2CID 9264507.
- S2CID 35178625.
- PMID 9725923.
- ^ S2CID 201099189.
- PMID 20858861.
- PMID 30588315.
- PMID 25528745.
- S2CID 20081569.
- ^ Northwestern Surgery for Atrial Fibrillation. Atrial Fibrillation Surgery Archived 19 April 2012 at the Wayback Machine
- PMID 27551927.
- S2CID 56176611.
- S2CID 251932594.
- PMID 22235005.
- PMID 26492310.
- S2CID 201717267.
- PMID 24682347.
- Executive summary: January CT, Wann LS, Alpert JS, Calkins H, Cigarroa JE, Cleveland JC, et al. (December 2014). "2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines and the Heart Rhythm Society". Circulation. 130 (23): 2071–2104. PMID 24682348.
- Executive summary: January CT, Wann LS, Alpert JS, Calkins H, Cigarroa JE, Cleveland JC, et al. (December 2014). "2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines and the Heart Rhythm Society". Circulation. 130 (23): 2071–2104.
- S2CID 201631227.
- PMID 31590581.
- S2CID 7881115.
- PMID 26786546.
- ^ PMID 29173598.
- ^ Atrial fibrillation and risk of stroke: a nationwide cohort study. Christine Benn Christiansen, Thomas A. Gerds, Jonas Bjerring Olesen, Søren Lund Kristensen, Morten Lamberts, Gregory Y.H. Lip, Gunnar H. Gislason, Lars Køber, Christian Torp-Pedersen. EP Europace, Volume 18, Issue 11, November 2016, Pages 1689–1697, https://doi.org/10.1093/europace/euv401 https://academic.oup.com/europace/article/18/11/1689/2437498 accessed 12 Oct 2020
- ^ Lopes RD, Crowley MJ, Shah BR, et al. Stroke Prevention in Atrial Fibrillation. Comparative Effectiveness Review No. 123. AHRQ Publication No. 13-EHC113-EF. Rockville, MD: Agency for Healthcare Research and Quality; August 2013. www.effectivehealthcare.ahrq.gov/ reports/final.cfm.
- S2CID 10318035.
- PMID 10525506.
- PMID 35861814.
- ^ PMID 30732716.
- S2CID 52901769.
- ^ PMID 27567408.
- S2CID 19079630.
- PMID 24385275.
- PMID 2144217.
- ^ S2CID 49305621.
- PMID 11343485.
- PMID 25960110.
- PMID 24103419.
- ^ Vulpian A (1874). "Note sur les effets de la faradisation directe des ventricules du coeur chez le chien". Archives de Physiologie Normale et Pathologique. 6: 975.
- PMID 7049202.
- ^ Nothnagel H (1876). "Ueber arythmische Herzthatigkeit". Deutsches Archiv für Klinische Medizin. 17: 190–220.
- PMID 20761393.
- ^ Einthoven W (1906). "Le telecardiogramme". Archives Internationales de Physiologie. 4: 132–64.
- ^ Rothberger CJ, Winterberg H (1909). "Vorhofflimmern und Arhythmia perpetua". Wiener Klinische Wochenschrift. 22: 839–44.
- PMID 20764769.
- S2CID 10629315.
- ^ PMID 28645513.
- ^ S2CID 78092141.
Further reading
- January CT, Wann LS, Calkins H, Chen LY, Cigarroa JE, Cleveland JC, et al. (July 2019). "2019 AHA/ACC/HRS Focused Update of the 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society". Journal of the American College of Cardiology. 74 (1): 104–132. PMID 30703431.
External links
- "Atrial Fibrillation". CVD Roadmaps. World Heart Federation.
