Salmonella
| Salmonella | |
|---|---|
| |
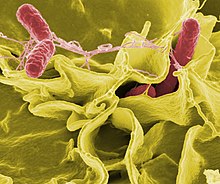
| Color-enhanced scanning electron micrograph showing Salmonella Typhimurium (red) invading cultured human cells
| |
| Scientific classification | |
| Domain: | Bacteria |
| Phylum: | Pseudomonadota |
| Class: | Gammaproteobacteria |
| Order: | Enterobacterales |
| Family: | Enterobacteriaceae |
| Genus: | Salmonella Lignières, 1900 |
| Species and subspecies[1] | |
| |
Salmonella is a
Salmonella species are non-
Salmonella species are
Nontyphoidal Salmonella serotypes are
Taxonomy
The genus Salmonella is part of the family of Enterobacteriaceae. Its taxonomy has been revised and has the potential to confuse. The genus comprises two species, S. bongori and S. enterica, the latter of which is divided into six subspecies: S. e. enterica, S. e. salamae, S. e. arizonae, S. e. diarizonae, S. e. houtenae, and S. e. indica.[8][9] The taxonomic group contains more than 2500 serotypes (also serovars) defined on the basis of the somatic O (lipopolysaccharide) and flagellar H antigens (the Kauffman–White classification). The full name of a serotype is given as, for example, Salmonella enterica subsp. enterica serotype Typhimurium, but can be abbreviated to Salmonella Typhimurium. Further differentiation of strains to assist clinical and epidemiological investigation may be achieved by antibiotic sensitivity testing and by other molecular biology techniques such as pulsed-field gel electrophoresis, multilocus sequence typing, and, increasingly, whole genome sequencing. Historically, salmonellae have been clinically categorized as invasive (typhoidal) or noninvasive (nontyphoidal salmonellae) based on host preference and disease manifestations in humans.[10]
History
Salmonella was first visualized in 1880 by Karl Eberth in the Peyer's patches and spleens of typhoid patients.[11] Four years later, Georg Theodor Gaffky was able to grow the pathogen in pure culture.[12] A year after that, medical research scientist Theobald Smith discovered what would be later known as Salmonella enterica (var. Choleraesuis). At the time, Smith was working as a research laboratory assistant in the Veterinary Division of the United States Department of Agriculture. The division was under the administration of Daniel Elmer Salmon, a veterinary pathologist.[13] Initially, Salmonella Choleraesuis was thought to be the causative agent of hog cholera, so Salmon and Smith named it "Hog-cholera bacillus". The name Salmonella was not used until 1900, when Joseph Leon Lignières proposed that the pathogen discovered by Salmon's group be called Salmonella in his honor.[14]: 16
In the late 1930s, Australian bacteriologist Nancy Atkinson established a salmonella typing laboratory – one of only three in the world at the time – at the Government of South Australia's Laboratory of Pathology and Bacteriology in Adelaide (later the Institute of Medical and Veterinary Science). It was here that Atkinson described multiple new strains of salmonella, including Salmonella Adelaide, which was isolated in 1943. Atkinson published her work on salmonellas in 1957.[15]
Serotyping
Serotyping is done by mixing cells with antibodies for a particular antigen. It can give some idea about risk. A 2014 study showed that S. Reading is very common among young turkey samples, but it is not a significant contributor to human salmonellosis.[16] Serotyping can assist in identifying the source of contamination by matching serotypes in people with serotypes in the suspected source of infection.[17] Appropriate prophylactic treatment can be identified from the known antibiotic resistance of the serotype.[18]
Newer methods of "serotyping" include xMAP and
Detection, culture, and growth conditions

Most subspecies of Salmonella produce
Salmonella can also be detected and subtyped using multiplex[24] or real-time polymerase chain reaction (qPCR)[25] from extracted Salmonella DNA.
Mathematical models of Salmonella growth kinetics have been developed for chicken, pork, tomatoes, and melons.[26][27][28][29][30] Salmonella reproduce asexually with a cell division interval of 40 minutes.[14][16][17][18]
Salmonella species lead predominantly host-associated lifestyles, but the bacteria were found to be able to persist in a bathroom setting for weeks following contamination, and are frequently isolated from water sources, which act as bacterial reservoirs and may help to facilitate transmission between hosts.[31] Salmonella is notorious for its ability to survive desiccation and can persist for years in dry environments and foods.[32]
The bacteria are not destroyed by freezing,
Salmonella species can be found in the digestive tracts of humans and animals, especially reptiles. Salmonella on the skin of reptiles or amphibians can be passed to people who handle the animals.[39] Food and water can also be contaminated with the bacteria if they come in contact with the feces of infected people or animals.[40]
Nomenclature
Initially, each Salmonella "species" was named according to clinical consideration, for example Salmonella typhi-murium (mouse-typhoid), S. cholerae-suis (pig-cholera). After host specificity was recognized not to exist for many species, new strains received species names according to the location at which the new strain was isolated.[41]
In 1987, Le Minor and Popoff used molecular findings to argue that Salmonella consisted of only one species,
The serotype or serovar is a classification of Salmonella based on antigens that the organism presents. The
In 2005, a third species, Salmonella subterranea, was proposed, but according to the
Pathogenicity
Salmonella species are facultative
Most infections are due to ingestion of food contaminated by animal feces, or by human feces, such as by a food-service worker at a commercial eatery. Salmonella serotypes can be divided into two main groups—typhoidal and nontyphoidal. Typhoidal serotypes include Salmonella Typhi and Salmonella Paratyphi A, which are adapted to humans and do not occur in other animals. Nontyphoidal serotypes are more common, and usually cause self-limiting
Salmonella pathogenicity and host interaction has been studied extensively since the 2010s. Most of the important virulent genes of Salmonella are encoded in five pathogenicity islands, the so-called Salmonella pathogenicity islands (SPIs). These are chromosomal encoded and have significant contribution to bacterial-host interaction. More traits like plasmids, flagella or biofilm-related proteins can contribute in the infection. SPIs are characterised to be regulated by complex and fine-tuned regulatory networks that allow the gene expression only in the presence of the right environmental stresses.[58]
Molecular modeling and active site analysis of SdiA homolog, a putative quorum sensor for Salmonella typhimurium pathogenicity reveals specific binding patterns of AHL transcriptional regulators.[59] It is also known that Salmonella plasmid virulence gene spvB enhances bacterial virulence by inhibiting autophagy.[60]
Typhoidal Salmonella
Typhoid fever is caused by Salmonella serotypes which are strictly adapted to humans or higher primates—these include
Nontyphoidal Salmonella
Non-invasive
Infection with nontyphoidal serotypes of Salmonella generally results in
The organisms enter through the digestive tract and must be ingested in large numbers to cause disease in healthy adults. An infection can only begin after living salmonellae (not merely Salmonella-produced toxins) reach the gastrointestinal tract. Some of the microorganisms are killed in the stomach, while the surviving ones enter the small intestine and multiply in tissues. Gastric acidity is responsible for the destruction of the majority of ingested bacteria, but Salmonella has evolved a degree of tolerance to acidic environments that allows a subset of ingested bacteria to survive.[61] Bacterial colonies may also become trapped in mucus produced in the esophagus. By the end of the incubation period, the nearby host cells are poisoned by endotoxins released from the dead salmonellae. The local response to the endotoxins is enteritis and gastrointestinal disorder.[citation needed]
About 2,000 serotypes of nontyphoidal Salmonella are known, which may be responsible for as many as 1.4 million illnesses in the United States each year. People who are at risk for severe illness include infants, elderly, organ-transplant recipients, and the immunocompromised.[40]
Invasive
While in developed countries, nontyphoidal serotypes present mostly as gastrointestinal disease, in sub-Saharan Africa, these serotypes can create a major problem in bloodstream infections, and are the most commonly isolated bacteria from the blood of those presenting with fever. Bloodstream infections caused by nontyphoidal salmonellae in Africa were reported in 2012 to have a case fatality rate of 20–25%. Most cases of invasive nontyphoidal Salmonella infection (iNTS) are caused by Salmonella enterica Typhimurium or Salmonella enterica Enteritidis. A new form of Salmonella Typhimurium (ST313) emerged in the southeast of the African continent 75 years ago, followed by a second wave which came out of central Africa 18 years later. This second wave of iNTS possibly originated in the Congo Basin, and early in the event picked up a gene that made it resistant to the antibiotic chloramphenicol. This created the need to use expensive antimicrobial drugs in areas of Africa that were very poor, making treatment difficult. The increased prevalence of iNTS in sub-Saharan Africa compared to other regions is thought to be due to the large proportion of the African population with some degree of immune suppression or impairment due to the burden of HIV, malaria, and malnutrition, especially in children. The genetic makeup of iNTS is evolving into a more typhoid-like bacterium, able to efficiently spread around the human body. Symptoms are reported to be diverse, including fever, hepatosplenomegaly, and respiratory symptoms, often with an absence of gastrointestinal symptoms.[62]
Epidemiology
Due to being considered sporadic, between 60% and 80% of salmonella infections cases go undiagnosed.[63] In March 2010, data analysis was completed to estimate an incidence rate of 1140 per 100,000 person-years. In the same analysis, 93.8 million cases of gastroenteritis were due to salmonella infections. At the 5th percentile the estimated amount was 61.8 million cases and at the 95th percentile the estimated amount was 131.6 million cases. The estimated number of deaths due to salmonella was approximately 155,000 deaths.[64] In 2014, in countries such as Bulgaria and Portugal, children under 4 were 32 and 82 times more likely, respectively, to have a salmonella infection.[65] Those who are most susceptible to infection are: children, pregnant women, elderly people, and those with deficient immune systems.[66]
Risk factors for Salmonella infections include a variety of foods. Meats such as chicken and pork have the possibility to be contaminated. A variety of vegetables and sprouts may also have salmonella. Lastly, a variety of processed foods such as chicken nuggets and pot pies may also contain this bacteria.[67]
Successful forms of prevention come from existing entities such as the
A recent Salmonella Typhimurium outbreak has been linked to chocolate.[71]
Global monitoring
In Germany, food-borne infections must be reported.[72] From 1990 to 2016, the number of officially recorded cases decreased from about 200,000 to about 13,000 cases.[73] In the United States, about 1,200,000 cases of Salmonella infection are estimated to occur each year.[74] A World Health Organization study estimated that 21,650,974 cases of typhoid fever occurred in 2000, 216,510 of which resulted in death, along with 5,412,744 cases of paratyphoid fever.[75]
Molecular mechanisms of infection
The mechanisms of infection differ between typhoidal and nontyphoidal serotypes, owing to their different targets in the body and the different symptoms that they cause. Both groups must enter by crossing the barrier created by the intestinal cell wall, but once they have passed this barrier, they use different strategies to cause infection.[citation needed]
Switch to virulence
While travelling to their target tissue in the gastrointestinal tract, Salmonella is exposed to stomach acid, to the detergent-like activity of bile in the intestine, to decreasing oxygen supply, to the competing normal gut flora, and finally to antimicrobial peptides present on the surface of the cells lining the intestinal wall. All of these form stresses that Salmonella can sense and reacts against, and they form virulence factors and as such regulate the switch from their normal growth in the intestine into virulence.[76]
The switch to virulence gives access to a replication
- Approach, in which they travel towards a host cell via intestinal peristalsis and through active swimming via the flagella, penetrate the mucus barrier, and locate themselves close to the epithelium lining the intestine,
- Adhesion, in which they adhere to a host cell using bacterial adhesins and a type III secretion system,
- Invasion, in which Salmonella enter the host cell (see variant mechanisms below),
- Replication, in which the bacterium may reproduce inside the host cell,
- Spread, in which the bacterium can spread to other organs via cells in the blood (if it succeeded in avoiding the immune defence). Alternatively, bacteria can go back towards the intestine, re-seeding the intestinal population.
- Re-invasion (a secondary infection, if now at a systemic site) and further replication.
Mechanisms of entry
Nontyphoidal serotypes preferentially enter
Salmonellae are also able to breach the intestinal barrier via
Much of the success of Salmonella in causing infection is attributed to two
The AvrA toxin injected by the SPI1 type III secretion system of S. Typhimurium works to inhibit the
Clinical symptoms
Salmonellosis is known to be able to cause back pain or spondylosis. It can manifest as five clinical patterns: gastrointestinal tract infection, enteric fever, bacteremia, local infection, and the chronic reservoir state. The initial symptoms are nonspecific fever, weakness, and myalgia among others. In the bacteremia state, it can spread to any parts of the body and this induces localized infection or it forms abscesses. The forms of localized Salmonella infections are arthritis, urinary tract infection, infection of the central nervous system, bone infection, soft tissue infection, etc.[80] Infection may remain as the latent form for a long time, and when the function of reticular endothelial cells is deteriorated, it may become activated and consequently, it may secondarily induce spreading infection in the bone several months or several years after acute salmonellosis.[80]
A 2018
Resistance to oxidative burst
A hallmark of Salmonella pathogenesis is the ability of the bacterium to survive and proliferate within phagocytes. Phagocytes produce DNA-damaging agents such as nitric oxide and oxygen radicals as a defense against pathogens. Thus, Salmonella species must face attack by molecules that challenge genome integrity. Buchmeier et al.[83] showed that mutants of S. enterica lacking RecA or RecBC protein function are highly sensitive to oxidative compounds synthesized by macrophages, and furthermore these findings indicate that successful systemic infection by S. enterica requires RecA- and RecBC-mediated recombinational repair of DNA damage.[83][84]
Host adaptation
S. enterica, through some of its serotypes such as Typhimurium and Enteritidis, shows signs of the ability to infect several different mammalian host species, while other serotypes such as Typhi seem to be restricted to only a few hosts.[85] Some of the ways that Salmonella serotypes have adapted to their hosts include loss of genetic material and mutation. In more complex mammalian species, immune systems, which include pathogen specific immune responses, target serovars of Salmonella through binding of antibodies to structures such as flagella. Through the loss of the genetic material that codes for a flagellum to form, Salmonella can evade a host's immune system.[86] mgtC leader RNA from bacteria virulence gene (mgtCBR operon) decreases flagellin production during infection by directly base pairing with mRNAs of the fljB gene encoding flagellin and promotes degradation.[87] In the study by Kisela et al., more pathogenic serovars of S. enterica were found to have certain adhesins in common that have developed out of convergent evolution.[88] This means that, as these strains of Salmonella have been exposed to similar conditions such as immune systems, similar structures evolved separately to negate these similar, more advanced defenses in hosts. Still, many questions remain about the way that Salmonella has evolved into so many different types, but Salmonella may have evolved through several phases. As Baumler et al. have suggested, Salmonella most likely evolved through horizontal gene transfer, formation of new serovars due to additional pathogenicity islands and through an approximation of its ancestry.[89] So, Salmonella could have evolved into its many different serotypes through gaining genetic information from different pathogenic bacteria. The presence of several pathogenicity islands in the genome of different serotypes has lent credence to this theory.[89]
Salmonella sv. Newport has signs of adaptation to a plant colonization lifestyle, which may play a role in its disproportionate association with foodborne illness linked to produce. A variety of functions selected for during sv. Newport persistence in tomatoes have been reported to be similar to those selected for in sv. Typhimurium from animal hosts.[90] The papA gene, which is unique to sv. Newport, contributes to the strain's fitness in tomatoes, and has homologs in genomes of other Enterobacteriaceae that are able to colonize plant and animal hosts.[90]
Research
In addition to their importance as pathogens, nontyphoidal Salmonella species such as S. enterica serovar Typhimurium are commonly used as homologues of typhoid species. Many findings are transferable and it attenuates the danger for the researcher in case of contamination, but is also limited. For example, it is not possible to study specific typhoidal toxins using this model.[91] However, strong research tools such as the commonly-used mouse intestine gastroenteritis model build upon the use of Salmonella Typhimurium.[92]
For genetics, S. Typhimurium has been instrumental in the development of genetic tools that led to an understanding of fundamental bacterial physiology. These developments were enabled by the discovery of the first generalized transducing phage P22[93] in S. Typhimurium, that allowed quick and easy genetic editing. In turn, this made fine structure genetic analysis possible. The large number of mutants led to a revision of genetic nomenclature for bacteria.[94] Many of the uses of transposons as genetic tools, including transposon delivery, mutagenesis, and construction of chromosome rearrangements, were also developed in S. Typhimurium. These genetic tools also led to a simple test for carcinogens, the Ames test.[95]
As a natural alternative to traditional antimicrobials, phages are being recognised as highly effective control agents for Salmonella and other foodborne bacteria.[96]
Ancient DNA
S. enterica genomes have been reconstructed from up to 6,500 year old human remains across Western Eurasia, which provides evidence for geographic widespread infections with systemic S. enterica during prehistory, and a possible role of the Neolithization process in the evolution of host adaptation.
See also
- 1984 Rajneeshee bioterror attack
- The Great Hormel Disaster of '98
- 2008 United States salmonellosis outbreak
- American Public Health Association v. Butz
- Bismuth sulfite agar
- Food testing strips
- Host–pathogen interaction
- List of foodborne illness outbreaks
- 2008–2009 peanut-borne salmonellosis
- Wright County Egg
- XLD agar
References
- ^ "Salmonella". NCBI taxonomy. Bethesda, MD: National Center for Biotechnology Information. Retrieved 27 January 2019.
- PMID 17760271.
- ^ PMID 28540296.
- PMID 25136336.
- ^ PMID 23554419.
- ^ S2CID 19344119.
- ISBN 978-0-8385-8529-0.
- PMID 10878026.
- ISBN 978-0-470-01796-8.
- PMID 23023330.
- S2CID 6979333.
- PMID 11623930.
- ^ "FDA/CFSAN—Food Safety A to Z Reference Guide—Salmonella". FDA–Center for Food Safety and Applied Nutrition. 2008-07-03. Archived from the original on 2009-03-02. Retrieved 2009-02-14.
- ^ ISBN 978-0-7910-8500-4. Retrieved 31 July 2015.
- ISSN 1833-7538. Retrieved 2022-10-27.
- ^ a b "Serotypes Profile of Salmonella Isolates from Meat and Poultry Products, January 1998 through December 2014" (PDF).
- ^ a b "Steps in a Foodborne Outbreak Investigation". 2018-11-09.
- ^ PMID 28781944.
- PMID 33014887.
- PMID 31167843.
- PMID 3108233.
- ^ "UK Standards for Microbiology Investigations: Changing the Phase of Salmonella" (PDF). UK Standards for Microbiology Investigations: 8–10. 8 January 2015. Archived (PDF) from the original on 2022-10-09. Retrieved 2 August 2015.
- ISBN 978-0-8493-3795-6.
- PMID 15071035.
- PMID 10970396.
- PMID 19244895.
- PMID 20951457.
- PMID 20819361.
- PMID 23726189.
- ^ Li D. "Development and validation of a mathematical model for growth of salmonella in cantaloupe". Archived from the original on November 20, 2013.
- PMID 12839733.
- PMID 28943871.
- PMID 5461164.
Mortality differences between wholly uninjured and predominantly injured populations were small and consistent (5% level) with a hypothesis of no difference.
- PMID 1098573.
Little decrease in viable population of the three species was noted on inoculated pecan halves stored at -18, -7, and 5°C for 32 weeks.
- PMID 30795117.
- PMID 19722389.
- ^ Partnership for Food Safety Education (PFSE) Fight BAC! Basic Brochure Archived 2013-08-31 at the Wayback Machine.
- USDA Internal Cooking Temperatures Chart Archived 2012-05-03 at the Wayback Machine. The USDA has other resources available at their Safe Food Handling Archived 2013-06-05 at the Wayback Machine fact-sheet page. See also the National Center for Home Food Preservation.
- ^ "Reptiles, Amphibians, and Salmonella". Centers for Disease Control and Prevention. U.S. Department of Health & Human Services. 25 November 2013. Retrieved 3 August 2013.
- ^ PMID 12635640.
- ^ F. Kauffmann: Die Bakteriologie der Salmonella-Gruppe. Munksgaard, Kopenhagen, 1941
- .
- PMID 2915026.
- ^ Janda JM, Abbott SL (2006). "The Enterobacteria", ASM Press.
- PMID 15653929.
- PMID 15653930.
- ISBN 978-1-904455-73-8.
- PMID 22737074.

- ^ Grimont PA, Xavier Weill F (2007). Antigenic Formulae of the Salmonella Serovars (PDF) (9th ed.). Institut Pasteur, Paris, France: WHO Collaborating Centre for Reference and Research on Salmonella. p. 7. Archived (PDF) from the original on 2022-10-09. Retrieved 26 August 2015.
- S2CID 32594451.
- ^ "Species: Atlantibacter subterranea". lpsn.dsmz.de.
- ^ "GTDB - Tree at g__Atlantibacter". gtdb.ecogenomic.org.
- ^ "Taxonomy browser (Atlantibacter)". www.ncbi.nlm.nih.gov.
- ^ "GTDB - Tree at g__Salmonella". gtdb.ecogenomic.org.
- PMID 25749450.
- PMID 22722237.
- ^ "What is the difference between nontyphoidal salmonellae and S typhi or S paratyphi?". www.medscape.com. Retrieved 2021-09-28.
- PMID 23554419.
- S2CID 25177221.
- PMID 26723267.
- PMID 8406841.
- PMID 22587967.
- ^ "Salmonella (non-typhoidal)". www.who.int. Retrieved 2019-12-05.
- PMID 20158401.
- ^ "Salmonellosis - Annual Epidemiological Report 2016 [2014 data]". European Centre for Disease Prevention and Control. 2016-01-31. Retrieved 2019-12-05.
- ^ "Get the Facts about Salmonella!". Center for Veterinary Medicine, FDA. 2019-06-06.
- ^ "Prevention | General Information | Salmonella | CDC". www.cdc.gov. 2019-03-06. Retrieved 2019-12-05.
- ^ "Salmonella". fsis.usda.gov.
- ^ "Salmonella". European Food Safety Authority. Retrieved 2019-12-05.
- ^ "Content not found". 3 March 2022.
- S2CID 249136373.
- ^ § 6 and § 7 of the German law on infectious disease prevention, Infektionsschutzgesetz
- ^ "Anzahl der jährlich registrierten Salmonellose-Erkrankungen in Deutschland bis 2016". Statista.
- ^ Salmonella. Centers for Disease Control and Prevention
- PMID 15298225.
- PMID 16023758.
- ^ S2CID 2365666.
- PMID 20300065.
- PMID 20430892.
- ^ PMID 21286449.
- ^ "Bacterial protein mimics DNA to sabotage cells' defenses: Study reveals details of Salmonella infections". Sciencedaily.
- S2CID 235256840.
- ^ S2CID 25127127.
- PMID 11751841.
- PMID 18583645.
- PMID 21859443.
- PMID 28874555.
- PMID 22685400.
- ^ PMID 9746553.
- ^ PMID 29867794.
- S2CID 51705854.
- PMID 16140013.
- PMID 12999698.
- PMID 5961488.
- PMID 768755.
- S2CID 248195843.
- PMID 32094538.
- PMID 30033331.
- S2CID 3358440.
External links
- Background on Salmonella from the Food Safety and Inspection Service of the United States Department of Agriculture
- Salmonella genomes and related information at PATRIC, a Bioinformatics Resource Center funded by NIAID
- Questions and Answers about commercial and institutional sanitizing methods Archived 2017-06-29 at the Wayback Machine
- Salmonella as an emerging pathogen from IFAS
- Notes on Salmonella nomenclature
- Salmonella motility video
- Avian Salmonella Archived 2011-12-09 at the Wayback Machine
- Overview of Salmonellosis — The Merck Veterinary Manual
