Iproniazid
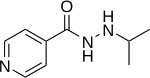 | |
| Clinical data | |
|---|---|
| Trade names | Marsilid, others |
| AHFS/Drugs.com | International Drug Names |
| ATC code | |
| Pharmacokinetic data | |
| Bioavailability | 1 |
| Identifiers | |
| |
JSmol) | |
| Density | 1.084 g/cm3 |
| Boiling point | 265.9 °C (510.6 °F) |
| |
| |
| (verify) | |
Iproniazid (Marsilid, Rivivol, Euphozid, Iprazid, Ipronid, Ipronin) is a non-selective,
History
Iproniazid was originally developed for the treatment of
Although iproniazid was one of the first
Structure and reactivity
The structure of iproniazid is chemically, in both structure and reactivity, similar to isoniazid. Iproniazid is a substituted hydrazine of which the isopropyl hydrazine moiety is essential for the inhibition of monoamine oxidase activity.[12]
Synthesis

There are multiple routes to synthesize iproniazid. The most common precursor is methyl isonicotinate which formes isonicotinohydrazide when it reacts with hydrazine.[13] Isonicotinohydrazide can be converted into iproniazid via different pathways.
One synthesis pathway involves AcMe which results in the formation of N'-(propan-2-ylidene)isonicotinohydrazide. Subsequently, the C=N linkage is selectively
In another pathway isonicotinohydrazide reacts with either 2-bromopropane or 2-chloropropane in an N-isopropyl addition reaction to the hydrazine moiety. This directly results in the formation of iproniazid.[16][17]
Reactions and mechanism of action
Iproniazid is a known
Inhibition of MAOs by iproniazid is competitive and sensitive to changes in pH and temperature, similar to oxidation of the monoamine substrate. Inhibition cannot be reversed by addition of the substrate.[18] Iproniazid is able to displace non-hydrazine inhibitors, but not other hydrazine inhibitors from the active site of the enzyme.[12]
To increase the inhibition of monoamine oxidase, cyanide can be used. The reaction however remains oxygen-dependent.[18] MAO inhibition can be decreased by addition of glutathione, suggesting non enzymatic conjugation of either iproniazid or isopropylhydrazine with glutathione.[18]
Metabolism and toxicity

Iproniazid is metabolized in the body. Iproniazid is converted to isopropyl hydrazine and isonicotinic acid in an initial hydrolysis reaction. Isopropyl hydrazine can either be released in the blood or it can be metabolically activated by microsomal CYP450 enzymes.[19] This oxidation of isopropyl hydrazine is a toxification reaction that eventually can lead to the formation of an alkylating agent: the isopropyl radical.[3] Hepatic necrosis was found in rats with doses as low as 10 mg/kg.[19]
Isopropyl radical
The presence of the isopropyl radical was indicated by another observed product of the metabolism of iproniazid: the gas propane.[3]
Alkylating agents have the capability to bind to chemical groups such as amino, phosphate hydroxyl, imidazole and sulfhydryl groups. The formed isopropyl radical is able to form S-isopropyl conjugates in vitro. This diminishes covalent binding to other proteins, however it was only observed in vitro. In vivo, hepatotoxic doses of isopropyl hydrazine, the precursor of the isopropyl radical, did not deplete sulfhydryl-group containing compounds.[3]
Liver necrosis
The isopropyl radical formed as a result of the metabolism of iproniazid, is able to covalently bind to proteins and other macromolecules in the liver. These interactions are the reason for the hepatotoxicity of iproniazid. Covalent binding results in liver necrosis by presumably changing protein function leading to organelle stress and acute toxicity.[20][21] However, the exact mechanism of how the binding of iproniazid derivatives to liver proteins would induce liver necrosis remains unclear.[3]
Cytochrome P450 enzymes are present at the highest concentrations in the liver, causing most alkylating agents to be produced in the liver. This explains why the liver is mostly damaged by covalent binding of alkylating agents such as the isopropyl radical.[19] Rat models and other animal models have shown that cytochrome P450 enzymes convert isopropyl hydrazine to alkylating compounds that induce liver necrosis. An inducer of a class of hepatic microsomal cytochrome P450 enzymes, phenobarbital, highly increased the chance of necrosis. In contrast, the compounds cobalt chloride, piperonyl butoxide and alpha-naphthylisothiocyanate inhibit microsomal enzymes which resulted in a decreased chance of necrosis due to isopropyl hydrazine.[19]
Metabolism to other forms
Iproniazid can also be metabolised by O-
Acetone can also be produced in alternative pathway as a metabolite of isopropyl hydrazine. It is eventually converted to CO2 and exhaled.[3]
Isonicotinic acid
Other toxic effects
Iproniazid can also interact with tyrosine-containing food products which may have toxic effects.[6][7]
Excretion
Excretion can occur via different routes: via the lungs, the urine, bile and sometimes via the skin or breast milk. Iproniazid has a molecular weight of 179.219 g/mol, which is far below 500 g/mol, and it is hydrophilic (because of e.g. the N-H groups in the molecule). These two properties together indicate that iproniazid is likely to be excreted in the urine via the kidneys.[24]
Iproniazid can also be metabolized and excreted afterwards in the form of one of its metabolites which can be found in the figure above. Isoniazid is hydrophilic[24] and has a molecular weight of 137.139 g/mol. Isoniazid is therefore expected to be excreted via the urine, if it is not further metabolized in the body. The same holds for isonicotinic acid and isonicotinoyl glycine. Carbon dioxide and propane are gaseous which are presumably transported out of the body by exhalation via the lungs.
Indication
Iproniazid was originally produced as anti-tuberculosis medicine, but found to be more effective as antidepressant. When it was discovered that iproniazid is hepatotoxic, it was replaced by medicinal xenobiotics that are less harmful to the liver. Examples of antidepressant drugs that are nowadays used instead of iproniazid are isocarboxazid, phenelzine, and tranylcypromine.[3]
Drugs more effective for treatment of tuberculosis are isoniazid, pyrazinamide, ethambutol and rifampicin.[25]
Efficacy and side effects
Efficacy
Iproniazid was designed to treat
Adverse effects
The most significant adverse effects of using iproniazid is the
Effects on animals
Rat animal models have been used to investigate the hepatotoxic (bio)chemical mechanism of iproniazid. A metabolite of iproniazid, isopropyl hydrazine, was found to be a potent hepatotoxin in rats.[3][19] Hepatic necrosis was found in rats with doses as low as 10 mg/kg.[19] It was predicted with admetSAR[28] that iproniazid had a LD50 of 2.6600 mol/kg in rats.[7]
Lethality
See the table for experimentally determined LD50, TDLo and LDLo values of various organisms.[29]
| Organism | Test Type | Route | Reported Dose (mg/kg) | Reference |
|---|---|---|---|---|
| Dog | LD50 | oral | 95 | Annals of the New York Academy of Sciences. Vol. 80, Pg. 626, 1959. |
| Human | TDLo | oral | 2.143 /D | Acta Neurologia et Psychiatrica Belgica. Vol. 59, Pg. 977, 1959. |
| Human | LDLo | oral | 14 /2W-I | Canadian Medical Association Journal. Vol. 78, Pg. 131, 1958. |
| Monkey | LD50 | oral | 640 | Annals of the New York Academy of Sciences. Vol. 80, Pg. 626, 1959. |
| Mouse | LD50 | Intramuscular | 615 | American Review of Tuberculosis. Vol. 65, Pg. 376, 1952. |
| Mouse | LD50 | intraperitoneal | 475 | Japanese Journal of Pharmacology. Vol. 13, Pg. 186, 1963. |
| Mouse | LD50 | intravenous | 719 | American Review of Tuberculosis. Vol. 65, Pg. 376, 1952. |
| Mouse | LD50 | oral | 440 | Pharmaceutical Chemistry Journal Vol. 30, Pg. 750, 1996. |
| Mouse | LD50 | subcateneous | 730 | American Review of Tuberculosis. Vol. 65, Pg. 376, 1952. |
| Rabbit | LD50 | intravenous | 117 | American Review of Tuberculosis. Vol. 65, Pg. 376, 1952. |
| Rabbit | LD50 | oral | 125 | American Review of Tuberculosis. Vol. 65, Pg. 376, 1952. |
| Rabbit | LDLo | skin | 2000 | Huntingdon Research Center Reports. Vol. -, Pg. -, 1972. |
| Rat | LD50 | subcutaneous | 538 | Japanese Journal of Pharmacology. Vol. 13, Pg. 186, 1963. |
| Rat | LD50 | unreported | 350 | Nature. Vol. 185, Pg. 532, 1960. |
| Rat | LD50 | oral | 365 | Journal of Pharmacology and Experimental Therapeutics. Vol. 119, Pg. 444, 1957. |
| Rat | LD50 | intraperitoneal | 375 | Arzneimittel-Forschung. Drug Research. Vol. 20, Pg. 363, 1970. |
See also
References
- ^ ISBN 9780896031807.
- PMID 2870717.
- ^ ISBN 978-0-8493-7302-2.
- ^ ISBN 9783642595196.
- PMID 21772661.
- ^ ISBN 9781118819449.
- ^ a b c d "Iproniazid". www.drugbank.ca. Retrieved 2018-03-27.
- PMID 23539642.
- PMID 18492727.
- S2CID 1675621.
- ISSN 0009-2347.
- ^ PMID 14075108.
- .
- .
- PMID 9795482.
- ^ Journal of the American Pharmaceutical Association (1912-1977), 42: 457,463
- ISSN 0016-5603.
- ^ PMID 13471553.
- ^ PMID 702322.
- PMID 28486401.
- PMID 4746326.
- S2CID 9309017.
- PMID 22037847.
- ^ PMID 932974.
- PMID 28715978.
- PMID 13151011.
- ^ "Side Effects of Iproniazid". edudrugs.com. Retrieved 2018-03-27.
- S2CID 16356154.
- ^ lookchem.com/Iproniazid
