Linezolid
 | |
 | |
| Clinical data | |
|---|---|
| Pronunciation | /lɪˈnɛzəlɪd, -ˈneɪz-/ |
| Trade names | Zyvox, Zyvoxam, others |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a602004 |
| License data | |
| Pregnancy category |
|
Oxazolidinone antibiotic | |
| ATC code | |
| Legal status | |
| Legal status | |
| Pharmacokinetic data | |
| Bioavailability | ~100% (oral) |
| Protein binding | Low (31%) |
| Metabolism | Liver (50–70%, CYP not involved) |
| Elimination half-life | 3–7 hours;[9] longer half-life in CSF than plasma[9] |
| Excretion | non-kidney, kidney, and fecal[10] |
| Identifiers | |
| |
JSmol) | |
| |
| |
| (verify) | |
Linezolid is an
When given for short periods, linezolid is a relatively safe antibiotic.
As a
Linezolid was discovered in the mid-1990s, and was approved for commercial use in 2000.
Medical uses
The main use of linezolid is the treatment of severe infections caused by
In the United States, the indications for linezolid use approved by the U.S.
Linezolid appears to be as safe and effective for use in children and newborns as it is in adults.[23]
Skin and soft tissue infections
A large
In the treatment of diabetic foot infections, linezolid appears to be cheaper and more effective than vancomycin.
Some authors have recommended that combinations of cheaper or more cost-effective drugs (such as
Pneumonia
No significant difference appears in treatment success rates between linezolid, glycopeptides, or appropriate beta-lactam antibiotics in the treatment of pneumonia.[24] Clinical guidelines for the treatment of community-acquired pneumonia developed by the American Thoracic Society and the Infectious Diseases Society of America recommend that linezolid be reserved for cases in which MRSA has been confirmed as the causative organism, or when MRSA infection is suspected based on the clinical presentation.[31] The guidelines of the British Thoracic Society do not recommend it as first-line treatment, but rather as an alternative to vancomycin.[32] Linezolid is also an acceptable second-line treatment for community-acquired pneumococcal pneumonia when penicillin resistance is present.[31]
U.S. guidelines recommend either linezolid or vancomycin as the first-line treatment for hospital-acquired (nosocomial) MRSA pneumonia.
Other
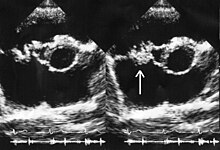
It is traditionally believed that so-called "deep" infections—such as osteomyelitis or infective endocarditis—should be treated with bactericidal antibiotics, not bacteriostatic ones. Nevertheless, preclinical studies were conducted to assess the efficacy of linezolid for these infections,[35] and the drug has been used successfully to treat them in clinical practice. Linezolid appears to be a reasonable therapeutic option for infective endocarditis caused by multi-resistant Gram-positive bacteria, despite a lack of high-quality evidence to support this use.[36][37] Results in the treatment of enterococcal endocarditis have varied, with some cases treated successfully and others not responding to therapy.[38][39][40][41][42][43] Low- to medium-quality evidence is also mounting for its use in bone and joint infections, including chronic osteomyelitis, although adverse effects are a significant concern when long-term use is necessary.[44][45][46][47][48][49]
In combination with other drugs, linezolid has been used to
Linezolid has been studied as an alternative to vancomycin in the treatment of
Infections of the central nervous system
In animal studies of meningitis caused by Streptococcus pneumoniae, linezolid was found to penetrate well into cerebrospinal fluid, but its effectiveness was inferior to that of other antibiotics.[54][55] There does not appear to be enough high-quality evidence to support the routine use of linezolid to treat bacterial meningitis. Nonetheless, it has been used successfully in many cases of central nervous system infection—including meningitis—caused by susceptible bacteria, and has also been suggested as a reasonable choice for this indication when treatment options are limited or when other antibiotics have failed.[56][57] The guidelines of the Infectious Diseases Society of America recommend linezolid as the first-line drug of choice for VRE meningitis, and as an alternative to vancomycin for MRSA meningitis.[58] Linezolid appears superior to vancomycin in treating community-acquired MRSA infections of the central nervous system, although very few cases of such infections have been published (as of 2009[update]).[59]
In March 2007, the FDA reported the results of a randomized, open-label, phase III clinical trial comparing linezolid to vancomycin in the treatment of catheter-related bloodstream infections. Patients treated with vancomycin could be switched to oxacillin or dicloxacillin if the bacteria that caused their infection was found to be susceptible, and patients in both groups (linezolid and vancomycin) could receive specific treatment against Gram-negative bacteria if necessary.[60] The study itself was published in January 2009.[61]
Linezolid was associated with significantly greater mortality than the comparator antibiotics. When data from all participants were pooled, the study found that 21.5% of those given linezolid died, compared to 16% of those not receiving it. The difference was found to be due to the inferiority of linezolid in the treatment of Gram-negative infections alone or mixed Gram-negative/Gram-positive infections. In participants whose infection was due to Gram-positive bacteria alone, linezolid was as safe and effective as vancomycin.[60][61] In light of these results, the FDA issued an alert reminding healthcare professionals that linezolid is not approved for the treatment of catheter-related infections or infections caused by Gram-negative organisms, and that more appropriate therapy should be instituted whenever a Gram-negative infection is confirmed or suspected.[60]
Specific populations
In adults and children over the age of 12, linezolid is usually given every 12 hours, whether orally or intravenously.[54][62] In younger children and infants, it is given every eight hours.[63] No dosage adjustments are required in the elderly, in people with mild-to-moderate liver failure, or in those with impaired kidney function.[64] In people requiring hemodialysis, care should be taken to give linezolid after a session, because dialysis removes 30–40% of a dose from the body; no dosage adjustments are needed in people undergoing continuous hemofiltration,[64] although more frequent administration may be warranted in some cases.[23] According to one study, linezolid may need to be given more frequently than normal in people with burns affecting more than 20% of body area, due to increased nonrenal clearance of the drug.[65]
Linezolid is in U.S. pregnancy category C, meaning there have been no adequate studies of its safety when used by pregnant women, and although animal studies have shown mild toxicity to the fetus, the benefits of using the drug may outweigh its risks.[8] It also passes into breast milk, although the clinical significance of this (if any) is unknown.[66]
Spectrum of activity
Linezolid is effective against all clinically important Gram-positive
Linezolid is considered bacteriostatic against most organisms—that is, it stops their growth and reproduction without actually killing them—but has some bactericidal (killing) activity against streptococci.[8][69] Some authors have noted that, despite its bacteriostatic effect in vitro, linezolid "behaves" as a bactericidal antibiotic in vivo because it inhibits the production of toxins by staphylococci and streptococci.[35] It also has a post-antibiotic effect lasting one to four hours for most bacteria, meaning that bacterial growth is temporarily suppressed even after the drug is discontinued.[23]
Gram-negative bacteria
Linezolid has no clinically significant effect on most Gram-negative bacteria. Pseudomonas and the Enterobacteriaceae, for instance, are not susceptible.[69] In vitro, it is active against Pasteurella multocida,[8][70] Fusobacterium, Moraxella catarrhalis, Legionella, Bordetella, and Elizabethkingia meningoseptica, and moderately active (having a minimum inhibitory concentration for 90% of strains of 8 mg/L) against Haemophilus influenzae.[66][69] It has also been used to great effect as a second-line treatment for Capnocytophaga infections.[56][71]
Comparable antibiotics
Linezolid's spectrum of activity against Gram-positive bacteria is similar to that of the glycopeptide antibiotic vancomycin, which has long been the standard for treatment of MRSA infections, and the two drugs are often compared.[12][23] Other comparable antibiotics include glycopeptide antibiotics such as teicoplanin (trade name Targocid), dalbavancin (Dalvance), oritavancin (Orbactiv), and telavancin (Vibativ); quinupristin/dalfopristin (Synercid, a combination of two streptogramins, not active against E. faecalis);[72] daptomycin (Cubicin, a lipopeptide); and ceftobiprole (Zevtera, a 5th-generation cephalosporin). Linezolid is the only one that can be taken by mouth for the treatment of systemic infections.[23]
Adverse effects
When used for short periods, linezolid is a relatively safe drug.
Like nearly all antibiotics, linezolid has been associated with
Long-term use
Bone marrow suppression, characterized particularly by thrombocytopenia (low platelet count), may occur during linezolid treatment; it appears to be the only adverse effect that occurs significantly more frequently with linezolid than with glycopeptides or beta-lactams.[24] It is uncommon in patients who receive the drug for 14 days or fewer, but occurs much more frequently in patients who receive longer courses or who have renal failure.[73][77] A 2004 case report suggested that pyridoxine (a form of vitamin B6) could reverse the anemia and thrombocytopenia caused by linezolid,[78] but a later, larger study found no protective effect.[79]
Long-term use of linezolid has also been associated with
The adverse effects of long-term linezolid therapy were first identified during postmarketing surveillance. Bone marrow suppression was not identified during Phase III trials, in which treatment did not exceed 21 days. Although some participants of early trials did experience thrombocytopenia, it was found to be reversible and did not occur significantly more frequently than in controls (participants not taking linezolid).[54] There have also been postmarketing reports of seizures, and, as of 2009[update], a single case each of Bell's palsy (paralysis of the facial nerve) and kidney toxicity.[74] Evidence of protein synthesis inhibition in mammalian cells by linezolid has been published.[95]
Interactions
Linezolid is a weak, non-selective, reversible
Linezolid does not inhibit or induce the cytochrome P450 (CYP) system, which is responsible for the metabolism of many commonly used drugs, and therefore does not have any CYP-related interactions.[8]
Pharmacology
Pharmacodynamics

Linezolid, like other
In 2008, the
Pharmacokinetics

One of the advantages of linezolid is that it has an
Linezolid's
Linezolid is
Chemistry
At physiological pH (7.4), linezolid exists in an uncharged state. It is moderately water-soluble (approximately 3 mg/mL), with a logP of 0.55.[23]
![Skeletal formula of N-{[(5S)-3-[3-fluoro-4-(morpholin-4-yl)phenyl]-2-oxo-1,3-oxazolidin-5-yl]methyl}acetamide, highlighting the morpholino and fluoro groups in orange, with the rest in blue. The carbon atoms of the parent chain are numbered.](http://upload.wikimedia.org/wikipedia/commons/thumb/e/ea/Linezolid_showing_oxazolidinone_pharmacophore.svg/220px-Linezolid_showing_oxazolidinone_pharmacophore.svg.png)
The oxazolidinone
The anticoagulant rivaroxaban (Xarelto) bears a striking structural similarity to linezolid; both drugs share the oxazolidinone pharmacophore, differing in only three areas (an extra ketone and chlorothiophene, and missing the fluorine atom). However this similarity appears to carry no clinical significance.[109]
Synthesis
Linezolid is a completely
Later syntheses have included an "
Resistance
Acquired resistance to linezolid was reported as early as 1999, in two patients with severe, multidrug-resistant Enterococcus faecium infection who received the drug through a compassionate use program.[69] Linezolid-resistant Staphylococcus aureus was first isolated in 2001.[115]
In the United States, resistance to linezolid has been monitored and tracked since 2004 through a program named LEADER, which (as of 2007[update]) was conducted in 60 medical institutions throughout the country. Resistance has remained stable and extremely low—less than one-half of one percent of
Mechanism
The intrinsic resistance of most Gram-negative bacteria to linezolid is due to the activity of
Gram-positive bacteria usually develop resistance to linezolid as the result of a
History
The oxazolidinones have been known as monoamine oxidase inhibitors since the late 1950s. Their antimicrobial properties were discovered by researchers at E.I. duPont de Nemours in the 1970s.[108] In 1978, DuPont patented a series of oxazolidinone derivatives as being effective in the treatment of bacterial and fungal plant diseases, and in 1984, another patent described their usefulness in treating bacterial infections in mammals.[54][108] In 1987, DuPont scientists presented a detailed description of the oxazolidinones as a new class of antibiotics with a novel mechanism of action.[108][127] Early compounds were found to produce liver toxicity, however, and development was discontinued.[72]
As of 2009[update], linezolid was the only oxazolidinone antibiotic available.[135] Other members of this class have entered development, such as posizolid (AZD2563),[136] ranbezolid (RBx 7644),[137] and radezolid (RX-1741).[138] In 2014, the FDA approved tedizolid phosphate, a second-generation oxazolidinone derivative, for acute bacterial skin and skin structure infection.[139][140]
Society and culture
Economics
Linezolid was quite expensive in 2009; a course of treatment may cost one or two thousand U.S. dollars for the drug alone,[64] not to mention other costs (such as those associated with hospital stay). With the medication becoming generic the price has decreased. In India as of 2015 a month of linezolid, as would be used to treat tuberculosis cost about US$60.[11]
However, because intravenous linezolid may be switched to an oral formulation (tablets or oral solution) without jeopardizing efficacy, people may be discharged from hospital relatively early and continue treatment at home, whereas home treatment with injectable antibiotics may be impractical.[141] Reducing the length of hospital stay reduces the overall cost of treatment, even though linezolid may have a higher acquisition cost—that is, it may be more expensive—than comparable antibiotics.
Studies have been conducted in several countries with different
In 2009, Pfizer paid $2.3 billion and entered a corporate integrity agreement to settle charges that it had misbranded and illegally promoted four drugs, and caused false claims to be submitted to government healthcare programs for uses that had not been approved by the United States Food and Drug Administration.[142] $1.3 billion was paid to settle criminal charges of illegally marketing the anti-inflammatory valdecoxib, while $1 billion was paid in civil fines regarding illegal marketing of three other drugs, including Zyvox.[143]
Brand names
| A | Amizole 500 (Kenya), Anozilad (Poland), Antizolid (Greece), Arlid (India), Arlin (Bangladesh), Averozolid & Debacozoline (Egypt) |
| B | |
| C | |
| D | Dilizolen (Poland, Slovakia, Netherlands, Bulgaria) |
| E | Entavar (India) |
| F | |
| G | Grampolid (Netherlands), Grampolyve (Netherlands), Gramposimide (Poland, Netherlands), Grampoxid (Netherlands) |
| H | |
| I | |
| J | |
| K | |
| L | Linzolid (Bangladesh), Lidobact (Netherlands), Linez (Bangladesh, Egypt), Linezolid Accord (Netherlands), Linezolid Amneal (Netherlands), Linezolid Betapharm (Netherlands), Linezolid Farmaprojects (Netherlands), Linezolid Fresenius Kabi (Netherlands), Linezolid GNP (Egypt), Linezolid Hetero (Netherlands), Linezolid Kabi (Croatia, Poland), Linezolid Mylan (Netherlands), Linezolid Pfizer (Netherlands), Linezolid Pliva (Croatia), Linezolid Polpharma (Netherlands, Poland), Linezolid Richet (Argentina), Linezolid Sandoz (Belgium, Switzerland, Netherlands, Slovakia, Estonia, Croatia, Poland), Linezolid Teva (Netherlands, Romania), Linezolid Zentiva (Poland), Linezolida Teva (Portugal), Linezone (Turkey), Linid (India), Linosept (India), Linozid (Bangladesh), Linxyd (Netherlands), Linzowin (India), Litrecan (Argentina), Livegramide (Netherlands), Lizbid (India), Lizemox (India), Lizolid (India, Vietnam), Lizoliden (Netherlands), Lizomac (India), Lizomed (India), Lizorex (India), Lizox (Netherlands), Lorezogram (Netherlands), Lynvox (Netherlands), Lynz (Croatia) |
| M | |
| N | Natlinez (Netherlands) |
| O | |
| P | Pneumolid (Croatia, Netherlands, Poland, Romania, Bulgaria) |
| Q | |
| R | Ralinz (India), Respenzo (Egypt) |
| S | Synzolid (Netherlands) |
| T | |
| U | |
| V | Voxazoldin (Egypt) |
| W | |
| X | |
| Y | |
| Z | Zenix (Bosnia and Herzegovina, Serbia), Zizolid (Turkey), Zodlin (India), Zolinid (Bulgaria), Zyvox (Georgia, Chile, Argentina, Australia, China, Ecuador, Egypt, United Kingdom, Hong Kong, Indonesia, Ireland, South Korea, Malta, Malaysia, New Zealand, Philippines, Singapore, Thailand, Taiwan, Japan, United States), Zyvoxam (Canada), Zyvoxid (Israel, Austria, Belgium, Bulgaria, Switzerland, Czech Republic, Denmark, Estonia, Spain, Finland, France, Greece, Germany, Croatia, Iceland, Lithuania, Latvia, Netherlands, Norway, Portugal, Romania, Sweden, Slovakia, Tunisia, Turkey, South Africa, Poland, Italy, Bosnia and Herzegovina) |
| Generic Combination | Brand Name |
|---|---|
| linezolid and cefixime | Zifi-Turbo (India) |
References
- ^ "Linezolid (Zyvox) Use During Pregnancy". Drugs.com. 16 April 2018. Archived from the original on 17 March 2020. Retrieved 17 March 2020.
- ^ "Linezolid, injection, 600 mg per 300 mL, tablet, 600 mg and powder for oral suspension, 20 mg per mL, Zyvox®". Australian Government Department of Health and Aged Care. 24 September 2001. Archived from the original on 18 November 2022. Retrieved 30 March 2024.
- ^ "Public Summary" (PDF). Retrieved 30 March 2024.
- ^ "Prescription medicines: registration of new generic medicines and biosimilar medicines, 2017". Therapeutic Goods Administration (TGA). 21 June 2022. Archived from the original on 6 July 2023. Retrieved 30 March 2024.
- ^ "Product information". health-products.canada.ca. 31 July 2020. Archived from the original on 29 March 2024. Retrieved 29 March 2024.
- ^ "Product information". health-products.canada.ca. 7 February 2006. Archived from the original on 29 March 2024. Retrieved 29 March 2024.
- ^ a b c "Zyvox 600 mg Film-Coated Tablets, 100 mg/5 ml Granules for Oral Suspension, 2 mg/ml Solution for Infusion – Summary of Product Characteristics (SPC)". electronic Medicines Compendium. 24 June 2009. Archived from the original on 6 August 2012. Retrieved 3 July 2009.
- ^ a b c d e f g h i j k l "Zyvox- linezolid injection, solution Zyvox- linezolid tablet, film coated Zyvox- linezolid suspension". DailyMed. 21 February 2020. Archived from the original on 26 April 2021. Retrieved 17 March 2020.
- ^ S2CID 4961324.
- ^ a b c d e f g h i j "Linezolid". The American Society of Health-System Pharmacists. Archived from the original on 20 December 2016. Retrieved 8 December 2016.
- ^ ISSN 0512-3054. WHO technical report series;994.
- ^ ISBN 978-0-7817-4802-5.
- ^ a b "Linezolid Side Effects in Detail". drugs.com. Archived from the original on 20 December 2016. Retrieved 11 December 2016.
- ^ PMID 9835522.
- PMID 24880801.
Emergence of resistance has been limited ... It is still uncertain whether the occurrences of such isolates are becoming more prevalent.
- ISBN 978-1-118-35446-9. Archivedfrom the original on 10 September 2017.
- ISBN 978-0-19-103962-1. Archivedfrom the original on 8 September 2017.
- hdl:10665/371090. WHO/MHP/HPS/EML/2023.02.
- ISBN 9789241515528.
- ^ Wroe D (28 February 2002). "An antibiotic to fight immune bugs". The Age. Archived from the original on 27 January 2010. Retrieved 16 May 2009.
- PMID 16735420.
- PMID 15013035.
- ^ S2CID 8791647.
- ^ PMID 18156089. Structured abstract with quality assessment available at DARE Archived 4 October 2011 at the Wayback Machine.
- S2CID 19381342.
- S2CID 30903985.
- S2CID 20586344.
- ^ PMID 19406516. Archived from the original(PDF) on 23 July 2011.
- PMID 18291550.
- .
- ^ PMID 17278083.
- ^ BTS Pneumonia Guidelines Committee (30 April 2004). "BTS guidelines for the management of community acquired pneumonia in adults – 2004 update" (PDF). British Thoracic Society. Archived from the original (PDF) on 7 April 2009. Retrieved 30 June 2009.
- ^ S2CID 14907563.
- PMID 15610562.
- ^ PMID 12746812.
- PMID 14999632.
- PMID 16735427.
- PMID 11303275.
- PMID 14688576.
- S2CID 40817941.
- PMID 12884185.
- PMID 17182759.
- S2CID 12651659.
- PMID 17204407. Review.
- PMID 15705640.
- S2CID 46391229.
- PMID 16982292.
- PMID 17574788.
- S2CID 12400080.
- PMID 15907341.
- PMID 16857689.
- PMID 15911549.
- doi:10.1086/504437.
- ^ (PDF) from the original on 14 March 2020. Retrieved 25 September 2019.
- PMID 11102418.
- ^ PMID 16220032. Archived from the originalon 22 July 2011.
- S2CID 33514115. Structured abstract with quality assessment available at DARE Archived 2 September 2011 at the Wayback Machine.
- PMID 15494903.
- PMID 19528145.
- ^ U.S. Food and Drug Administration (FDA). Archivedfrom the original on 19 October 2010. Retrieved 15 September 2010.
- ^ PMID 19072714.
- ^ from the original on 24 July 2008.
- ^ Buck ML (June 2003). "Linezolid use for resistant Gram-positive infections in children" (PDF). Pediatric Pharmacotherapy. 9 (6). Archived from the original (PDF) on 5 June 2011. Retrieved 8 June 2009.
- ^ a b c d e f g Lexi-Comp (August 2008). "Linezolid". The Merck Manual Professional. Archived from the original on 26 April 2009. Retrieved on 14 May 2009.
- PMID 19153078.
- ^ ISBN 978-0-7817-3371-7. Retrieved 20 June 2009.
- PMID 17210770.
- S2CID 33975237.
- ^ .
- ^ [No authors listed] (5 August 2008). "Animal Bites and Pasteurella multocida: Information for Healthcare Staff". Health Protection Agency. Archived from the original on 26 January 2010. Retrieved on 15 May 2009.
- S2CID 34825943.
- ^ PMID 10980159.
- ^ PMID 12730142. Review. Includes extensive discussion of the hematological adverse effects of linezolid.
- ^ S2CID 5691388.
- S2CID 37705529.
- PMID 11959617.
- PMID 16935472.
- PMID 15317746.
- PMID 17029128.
- ^ a b del Pino BM (23 February 2010). "Chemotherapy-induced Peripheral Neuropathy". NCI Cancer Bulletin. 7 (4): 6. Archived from the original on 11 December 2011.
- ISBN 9781498704304.
- PMID 22609781.
- ISBN 9783527326693.
- ^ Grisold W, Oberndorfer S, Windebank AJ (2012). "Chemotherapy and polyneuropathies" (PDF). European Association of Neurooncology Magazine. 12 (1). Archived (PDF) from the original on 6 October 2014.
- ^ "Review: could Herceptin cause Peripheral sensory neuropathy". Archived from the original on 17 March 2016. Retrieved 4 May 2016.
- S2CID 40772687.
- PMID 15288827.
- S2CID 28881160.
- S2CID 33138699.
- PMID 15953450.
- ^ PMID 16306535.
- PMID 17179125.
- PMID 16723564.
- PMID 16569895.
- PMID 2814477.
- PMID 16652315.
- S2CID 24150415.
- ^ Waknine Y (5 September 2008). "FDA Safety Changes: Mirena, Zyvox, Orencia". Medscape. Archived from the original on 2 December 2008. Retrieved 6 September 2008. Freely available with registration.
- S2CID 37436341.
- S2CID 23670767.
- ^ S2CID 3334681.
- PMID 18494460.
- PMID 18757750.
- S2CID 6289226.
- ^ from the original on 28 August 2021. Retrieved 3 April 2011.
- S2CID 38863420.
- ^ PMID 27999068.
- ^ structure-activity relationships.
- ^ European Medicines Agency (2011). "CHP Assessment Report for Xarelto (EMA/CHMP/301607/2011)" (PDF). Archived (PDF) from the original on 30 January 2012. Retrieved 15 March 2012.
- ^ a b c Xu GY, Zhou Y, Xu MC (2006). "A convenient synthesis of antibacterial linezolid from (S)-glyceraldehyde acetonide" (PDF). Chinese Chemical Letters. 17 (3): 302–4. Archived from the original (PDF) on 7 July 2011.
- ^ a b Kaiser CR, Cunico W, Pinheiro AC, de Oliveira AG, Peralta MA, de Souza MV (2007). "Oxazolidinonas: uma nova classe de compostos no combate à tuberculose" [Oxazolidinones: a new class of compounds against tuberculosis] (PDF). Revista Brasileira de Farmácia (in Portuguese). 88 (2): 83–8. Archived from the original (PDF) on 15 May 2012.
- ^ US patent 5837870, Pearlman BA, Perrault WR, Barbachyn MR, et al., "Process to prepare oxazolidinones", issued 1997-03-28 Retrieved on 13 June 2009.
- .
- ^ Perrault WR, Keeler JB, Snyder WC, et al. (25 June 2008). "Convergent green synthesis of linezolid (Zyvox)" Archived 28 July 2011 at the Wayback Machine, in 12th Annual Green Chemistry and Engineering Conference, 24–26 June 2008, New York, NY. Retrieved on 8 June 2009.
- S2CID 27426801.
- PMID 19022153.
- PMID 19500528.
- PMID 18819981.
- S2CID 2468640.
- ^ PMID 18391028.
- PMID 16971414.
- S2CID 1085422.
- PMID 18212098.
- PMID 19351617.
- PMID 19376688.
- PMID 19429927.
- (PDF) from the original on 11 June 2011.
- PMID 12455414.
- ^ "Drug Approval Package: Zyvox". FDA Center for Drug Evaluation and Research. 20 November 2001. Archived from the original on 10 January 2008. Retrieved 17 January 2009. Comprehensive review of the FDA approval process. Includes detailed reviews of the chemistry and pharmacology of linezolid, correspondence between the FDA and Pharmacia & Upjohn, and administrative documents.
- National Health Surveillance Agency. Archived from the originalon 19 July 2011. Retrieved 19 May 2009.
- PMID 12425150.
- ^ a b "Canada Approves Marketing Of Zyvoxam (Linezolid) For Gram Positive Infections" (Press release). 8 May 2001. Archived from the original on 28 August 2008. Retrieved 18 May 2009.
- (PDF) from the original on 29 September 2011.
- ^ "Pharmacia Corporation Reports 17% Increase In Second-Quarter Earnings-Per-Share Driven By 61% Increase In Pharmaceutical Earnings" (Press release). Pharmacia Corporation. 25 July 2001. Archived from the original on 9 May 2012. Retrieved 19 May 2009.
- PMID 19164418.
- (PDF) from the original on 29 September 2011.
- PMID 19075051.
- ^ "Rx 1741". Rib-X Pharmaceuticals. 2009. Archived from the original on 26 February 2009. Retrieved 17 May 2009.
- ^ "Drug Approval Package: Sivextro (tedizolid phosphate) tablets NDA #205435". U.S. Food and Drug Administration (FDA). 16 July 2014. Archived from the original on 6 July 2020. Retrieved 29 March 2024.
- ^ "Drug Approval Package: Sivextro (tedizolid phosphate) injection NDA #205436". U.S. Food and Drug Administration (FDA). 10 October 2014. Archived from the original on 6 July 2020. Retrieved 29 March 2024.
- ^ S2CID 3005291.
- ^ "Pfizer agrees record fraud fine". BBC News. 2 September 2009. Archived from the original on 8 September 2009. Retrieved 12 September 2009.
- ^ Harris G (2 September 2009). "Pfizer pays $2.3 billion to settle marketing case". The New York Times. Archived from the original on 22 August 2011. Retrieved 12 September 2009.
- ^ a b "Linezolid". Drugs.com. Archived from the original on 29 December 2018. Retrieved 29 December 2018.
