User:I enjoy sandwiches/h
Hormone replacement therapy (HRT), also known as menopausal hormone therapy (MHT) or postmenopausal hormone therapy (PHT, PMHT), is a form of
The main
The long-term effects of HRT on most organ systems vary by age and time since last physiologic exposure to hormones, and there can be large differences in individual regimens, factors which have made analyzing effect difficult.[7] There have been several large trials on hormone replacement in women, with the Women's Health Initiative (WHI) of the National Institutes of Health being the largest prospective study to date, and in particular having a significant impact since its inception. The WHI was a massive study of over 27,000 women conducted beginning in 1991 and taking place over 15 years, with multiple subsequent publications since that time analyzing its data.
The results of the WHI have been complex, and suggest both potential risks and benefits across different organ systems. Long term follow up of the WHI participants, however, has found no difference in
The current indications for use from the
Indications
Women receiving this treatment are usually
Potential menopausal symptoms include:[1][2]
- Hot flashes - vasomotor symptoms
- dryness
- Dyspareunia - painful sexual intercourse due to vaginal atrophy and lack of lubrication
- bone mineral density, which can eventually lead to osteopenia, osteoporosis, and associated fractures
- Decreased sexual desire
- Sleep disturbances and joint pain
The most common of these are are
HRT may impact diseases like breast cancer, colorectal cancer, endometrial cancer, cardiovascular disease and dementia, though there is much debate in the medical community as to magnitude of effect and whether positive or negative.
HRT is often given as a short-term relief from menopausal symptoms during
Long term health effects
The effects of HRT on most organ systems vary by age and time since last physiologic exposure to hormones, and there can be large differences in individual regimens, factors which have made analyzing effect difficult.[7] Demographically, the vast majority of data available is in postmenopausal American women with concurrent pre-existing conditions, and with a mean age of over 60 years.[15]
The Women's Health Initiative (WHI) of the National Institutes of Health (NIH) is a massive study of over 27,000 women beginning in 1991 and has been the largest prospective analysis of HRT effects in menopause to date. Successive analyses have found sometimes contradictory results, with the most recent publication in 2017 finding no difference for all cause mortality with HRT.[7]
Potential benefits
Bone density
Cardiovascular disease
A
HRT also improves
Endometrial cancer

In postmenopausal women, continuous combined estrogen plus progestin decreases endometrial cancer incidence.[23] The duration of progestogen therapy should be at least 14 days per cycle to prevent endometrial disease.[24]
Endometrial cancer has been grouped into two forms in the context of hormone replacement. Type 1 is the most common, can be associated with estrogen therapy, and is usually low grade. Type 2 is not related to estrogen stimulation and usually higher grade and poorer prognosis.[25] The endometrial hyperplasia that leads to endometrial cancer with estrogen therapy can be prevented by concomitant administration of progestogen.[25] The extensive use of high-dose estrogens for birth control in the 1970s is thought to have resulted in a significant increase in the incidence of type 1 endometrial cancer.[26]
Paradoxically, progestogens do promote the growth of
Muscle mass
Hormone replacement therapy in the form of estrogen and androgen can be effective at reversing the effects of aging on muscle.[27]
Neurodegenerative disorders
HRT may increase risk of dementia if initiated after 65 years of age, but have a neutral outcome or be neuroprotective for those between 50-55 years.[16] HRT can also improve executive and attention processes outside of the context of dementia in postmenopausal women.[28]
Sexual function
It is commonly misunderstood that as women complete their reproductive years, sexual activity stops altogether. Epidemiological surveys suggest that this is not true for most, with a recent study amongst women aged 40–69 revealing that 75% of women remain sexually active.[5] With increasing life spans, women today are living one third or more of their lives in a postmenopausal state, a period during which healthy sexuality can be integral to their quality of life.[29]
A major complaint among postmenopausal women is decreased libido and sexual function, and many may seek medical consultation.
The effectiveness of hormone replacement can decline in some women after long-term use.[13] A number of studies have also found that the combined effects of estrogen/androgen replacement therapy can increase libido and arousal over estrogen alone.[13] Findings on a relatively new form of HRT called tibolone, a synthetic steroid with estrogenic, androgenic, and progestogenic properties, suggest that it has the ability to improve mood, libido, and physical symptoms of surgically menopausal women to a greater degree than ERT. In various placebo-controlled studies, improvements in vasomotor symptoms, emotional response, sleep disturbances, physical symptoms, and sexual desire have been observed.[6] Tibolone has been used in Europe for almost two decades but is not available North America at this point.[6]
Skin
Estrogen replacement promotes
Potential risks
Breast cancer
There is a

The WHI also found a non-significant trend in the estrogen-alone clinical trial towards a reduced risk of breast cancer, though estrogen is usually only given alone in the setting of a hysterectomy due to the effect of unopposed estrogen on the uterus.[19][34]
HRT has been more strongly associated with risk of breast cancer in women with a lower range body mass indices (BMIs). No breast cancer association has been found with BMIs of over 25.[35] It has been suggested by some that the absence of significant effect in some of these studies could be due to selective prescription to overweight women who have higher baseline estrone, or to the very low progesterone serum levels after oral administration leading to a high tumor inactivation rate.[36]
For women who previously have had breast cancer, it is recommended to first consider other options for menopausal effects, such as
Colorectal cancer
In the WHI study, results were mixed. Women who took combined estrogen-progesterone therapy had a lower risk of getting
Ovarian cancer
A 2015 meta-analysis found that HRT was associated with an increased risk of
Pulmonary embolism and venous clotting
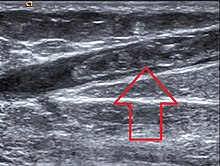
Comparisons between routes of administration suggest that when estrogens are taken orally the risk of a
Stroke
Multiple studies suggest that the possibility of HRT related stroke is absent if therapy is started within five years of menopause,
Available forms
There are five major human steroid hormones: estrogens, progestogens,
In women with intact uteruses, estrogens are almost always given in combination with progestogens, as long-term unopposed estrogen therapy is associated with a markedly increased risk of endometrial hyperplasia and endometrial cancer.[3] Conversely, in women who have undergone a hysterectomy or do not have a uterus, a progestogen is not required, and estrogen can be used alone. There are many combined formulations which include both estrogen and progestogen.
Specific types of hormone replacement include:[3]
- synthetic estrogens like ethinylestradiol
- progestins (synthetic progestogens) like medroxyprogesterone acetate (MPA), norethisterone, and dydrogesterone
- Androgens – bioidentical testosterone and dehydroepiandrosterone (DHEA), and synthetic anabolic steroids like methyltestosterone and nandrolone decanoate[43][44]
Tibolone is a synthetic derivative of Mexican yam whose metabolites have estrogenic, progestogenic, and androgenic effects.[3]
Vaginal estrogen can improve local atrophy and dryness, with fewer systemic effects than estrogens delivered by other routes.[45] Sometimes an androgen, generally testosterone, is added to treat diminished libido. It may also treat reduced energy and help reduce osteoporosis after menopause.
Continuous versus cyclic
Dosage is often varied cyclically to more closely mimic the ovarian hormone cycle, with estrogens taken daily and progestogens taken for about two weeks every month or every other month, a schedule referred to as 'cyclic' or 'sequentially combined'. Alternatively, 'continuous combined' HRT can be given with a constant daily hormonal dosage.
| Route/form | Estrogen | Low | Standard | High | |||
|---|---|---|---|---|---|---|---|
| Oral | Estradiol | 0.5–1 mg/day | 1–2 mg/day | 2–4 mg/day | |||
| Estradiol valerate | 0.5–1 mg/day | 1–2 mg/day | 2–4 mg/day | ||||
| Estradiol acetate | 0.45–0.9 mg/day | 0.9–1.8 mg/day | 1.8–3.6 mg/day | ||||
| Conjugated estrogens | 0.3–0.45 mg/day | 0.625 mg/day | 0.9–1.25 mg/day | ||||
| Esterified estrogens | 0.3–0.45 mg/day | 0.625 mg/day | 0.9–1.25 mg/day | ||||
| Estropipate | 0.75 mg/day | 1.5 mg/day | 3 mg/day | ||||
| Estriol | 1–2 mg/day | 2–4 mg/day | 4–8 mg/day | ||||
| Ethinylestradiola | 2.5–10 μg/day | 5–20 μg/day | – | ||||
| Nasal spray | Estradiol | 150 μg/day | 300 μg/day | 600 μg/day | |||
| Transdermal patch | Estradiol | 25 μg/dayb | 50 μg/dayb | 100 μg/dayb | |||
Transdermal gel |
Estradiol | 0.5 mg/day | 1–1.5 mg/day | 2–3 mg/day | |||
Vaginal |
Estradiol | 25 μg/day | – | – | |||
| Estriol | 30 μg/day | 0.5 mg 2x/week | 0.5 mg/day | ||||
SC injection |
Estradiol valerate | – | – | 4 mg 1x/4 weeks | |||
| Estradiol cypionate | 1 mg 1x/3–4 weeks | 3 mg 1x/3–4 weeks | 5 mg 1x/3–4 weeks | ||||
| Estradiol benzoate | 0.5 mg 1x/week | 1 mg 1x/week | 1.5 mg 1x/week | ||||
| SC implant | Estradiol | 25 mg 1x/6 months | 50 mg 1x/6 months | 100 mg 1x/6 months | |||
| Footnotes: a = No longer used or recommended, due to health concerns. b = As a single patch applied once or twice per week (worn for 3–4 days or 7 days), depending on the formulation. Note: Dosages are not necessarily equivalent. Sources: See template. | |||||||
Route of administration
- Oral administration – tablets, capsules
- gels, creams
- Vaginal administration – tablets, creams, suppositories, rings
- Subcutaneous implant – surgically-inserted pellets placed into fat tissue
- Less commonly intranasal, and rectal administration, as well as intrauterine devices
More recently developed forms of drug delivery are alleged to have increased local effect lower dosing, fewer side effects, and constant rather than cyclical serum hormone levels.
Bioidentical hormone therapy
Bioidentical hormones can be used in either pharmaceutical or compounded preparations, with the latter generally not recommended by regulatory bodies due to their lack of standardization and regulatory oversight.[48] Most classifications of bioidentical hormones do not take into account manufacturing, source, or delivery method of the products, and so describe both non-FDA approved compounded products and FDA approved pharmaceuticals as 'bioidentical'.[9]
Bioidentical hormones in pharmaceuticals may have health benefits over their animal derived counterparts, including a potentially decreased risk of
Compounding
Compounding for HRT is generally discouraged by the FDA and medical industry in the United States due to a lack of regulation and standardized dosing.
In the United Kingdom, on the other hand, compounding is a regulated activity. The Medicines and Healthcare products Regulatory Agency regulates compounding performed under a Manufacturing Specials license and the General Pharmaceutical Council regulates compounding performed within a pharmacy. All testosterone prescribed in the United Kingdom is bioidentical, with its use supported by the National Health Service. There is also marketing authorisation for male testosterone products. National Institute for Health and Care Excellence guideline 1.4.8 states: "consider testosterone supplementation for menopausal women with low sexual desire if HRT alone is not effective". The footnote adds: "at the time of publication (November 2015), testosterone did not have a United Kingdom marketing authorisation for this indication in women. Bio-identical progesterone is used in IVF treatment and for pregnant women who are at risk of premature labour."
Side effects
Some common and uncommon side effects include:[52]
Common
- Headache
- stomach cramps or bloating
- Diarrhea
- Appetite and weight changes
- Changes in sex drive or performance
- Nervousness
- Brown or black patches on the skin
- Acne
- Swelling of hands, feet, or lower legs due to fluid retention
- Changes in menstrual flow
- Breast tenderness, enlargement, or discharge
- Sudden difficulty wearing contact lenses
Uncommon
- Double vision
- Severe abdominal pain
- Yellowing of skin or eyes
- Severe depression
- Unusual bleeding
- Loss of appetite
- Skin rash
- Lassitude
- Fever
- Dark-colored urine
- Light colored stool
- Chorea[53]
Contraindications
The following are absolute and relative contraindications to HRT:[54]
Absolute contraindications
- Undiagnosed vaginal bleeding
- Severe liver disease
- Pregnancy
- Severe coronary artery disease
- Aggressive breast, uterine or ovarian cancer
Relative contraindications
- Migraine headaches
- History of breast cancer
- History of ovarian cancer
- Venous thrombosis
- History of uterine fibroids
- Atypical ductal hyperplasia of the breast
- Active cholangitis, cholecystitis)
- Well-differentiated and early endometrial cancer - once treatment for the malignancy is complete, is no longer an absolute contraindication.
Medical and regulatory body statements
Current indications for HRT from the FDA include short-term treatment of menopausal symptoms such as hot flashes and vaginal atrophy, and prevention of osteoporosis.[10]
The
The
The American Association of Clinical Endocrinologists (AACE) has also released multiple position statements approving of HRT in appropriate clinical scenarios.[59]
History and research
The extraction of CEEs from the urine of pregnant
Women's Health Initiative and other trials
The WHI results were both positive and negative, suggesting that during the time of hormone therapy itself, there are increases in invasive
The actual trials were intended to be conducted between 1991 and 2006.
Initial data from the WHI in 2002 suggested mortality to be lower when HRT was begun earlier, between age 50 to 59, but higher when begun after age 60. In older patients, there was an apparent increased incidence of
In 2002 when the first WHI follow up study was published, with HRT in post menopausal women, both older and younger age groups had a slightly higher incidence of
The data published by the WHI suggested supplemental estrogen increased risk of venous thromboembolism and breast cancer but was protective against osteoporosis and colorectal cancer, while the impact on cardiovascular disease was mixed.[66] These results were later supported in trials from the United Kingdom, but not in more recent studies from France and China. Genetic polymorphism appears to be associated with inter-individual variability in metabolic response to HRT in postmenopausal women.[67][68]
Neither the WHI nor the MWS differentiated the results for different types of progestogens used. MPA – the type most commonly used in the United States – was the only one examined by the WHI, which in its analysis and conclusions extrapolated the benefits versus risks of MPA to all progestins. This conclusion has since been challenged by several researchers as unjustified and misleading, resulting in unreasonable, unnecessary avoidance by many women of HRT. In addition, subsequent findings released by the WHI showed that all cause mortality was not dramatically different between the groups receiving CEEs, those receiving estrogen and a progestogen, and those not on therapy.[69] In addition, the WHI trial was limited by low adherence, high attrition, inadequate power to detect risks for some outcomes, and evaluation of few regimens.[65] The double blinding limited validity of study results due to its effects on patient exclusion criteria. Patients who were experiencing symptoms of the menopausal transition were excluded from the study, meaning that younger women who had only recently experienced menopause were not significantly represented. As a result, while the average age of menopause is age 51, study participants were on average 62 years of age. Demographically, the vast majority were Caucasian, and tended to be slightly overweight and former smokers.
| Clinical outcome | Hypothesized effect on risk |
Estrogen and progestogen (CEs 0.625 mg/day p.o. + MPA 2.5 mg/day p.o.) (n = 16,608, with uterus, 5.2–5.6 years follow up) |
Estrogen alone (CEs 0.625 mg/day p.o.) (n = 10,739, no uterus, 6.8–7.1 years follow up) | ||||
|---|---|---|---|---|---|---|---|
| HR | 95% CI | AR
|
HR | 95% CI | AR
| ||
Coronary heart disease
|
Decreased | 1.24 | 1.00–1.54 | +6 / 10,000 PYs | 0.95 | 0.79–1.15 | −3 / 10,000 PYs |
| Stroke | Decreased | 1.31 | 1.02–1.68 | +8 / 10,000 PYs | 1.37 | 1.09–1.73 | +12 / 10,000 PYs |
| Pulmonary embolism | Increased | 2.13 | 1.45–3.11 | +10 / 10,000 PYs | 1.37 | 0.90–2.07 | +4 / 10,000 PYs |
Venous thromboembolism
|
Increased | 2.06 | 1.57–2.70 | +18 / 10,000 PYs | 1.32 | 0.99–1.75 | +8 / 10,000 PYs |
| Breast cancer | Increased | 1.24 | 1.02–1.50 | +8 / 10,000 PYs | 0.80 | 0.62–1.04 | −6 / 10,000 PYs |
| Colorectal cancer | Decreased | 0.56 | 0.38–0.81 | −7 / 10,000 PYs | 1.08 | 0.75–1.55 | +1 / 10,000 PYs |
| Endometrial cancer | – | 0.81 | 0.48–1.36 | −1 / 10,000 PYs | – | – | – |
| Hip fractures | Decreased | 0.67 | 0.47–0.96 | −5 / 10,000 PYs | 0.65 | 0.45–0.94 | −7 / 10,000 PYs |
| Total fractures | Decreased | 0.76 | 0.69–0.83 | −47 / 10,000 PYs | 0.71 | 0.64–0.80 | −53 / 10,000 PYs |
| Total mortality | Decreased | 0.98 | 0.82–1.18 | −1 / 10,000 PYs | 1.04 | 0.91–1.12 | +3 / 10,000 PYs |
| Global index | – | 1.15 | 1.03–1.28 | +19 / 10,000 PYs | 1.01 | 1.09–1.12 | +2 / 10,000 PYs |
| Diabetes | – | 0.79 | 0.67–0.93 | 0.88 | 0.77–1.01 | ||
| Gallbladder disease | Increased | 1.59 | 1.28–1.97 | 1.67 | 1.35–2.06 | ||
| Stress incontinence | – | 1.87 | 1.61–2.18 | 2.15 | 1.77–2.82 | ||
Urge incontinence
|
– | 1.15 | 0.99–1.34 | 1.32 | 1.10–1.58 | ||
| Peripheral artery disease | – | 0.89 | 0.63–1.25 | 1.32 | 0.99–1.77 | ||
| Probable dementia | Decreased | 2.05 | 1.21–3.48 | 1.49 | 0.83–2.66 | ||
| Abbreviations: CEs = coronary heart disease, stroke, pulmonary embolism, breast cancer, colorectal cancer, endometrial cancer (estrogen plus progestogen group only), hip fractures, and death from other causes. Sources: See template.
| |||||||
The WHI reported
After the increased clotting found in the first WHI results was reported in 2002, the number of Prempro prescriptions filled reduced by almost half. Following the WHI results, a large percentage of HRT users opted out of them, which was quickly followed by a sharp drop in breast cancer rates. The decrease in breast cancer rates has continued in subsequent years.[71] An unknown number of women started taking alternatives to Prempro, such as compounded bioidentical hormones, though researchers have asserted that compounded hormones are not significantly different from conventional hormone therapy.[72]
The other portion of the parallel studies featured women who were post hysterectomy and so received either placebo progestogen or CEEs alone. This group did not show the risks demonstrated in the combination hormone study, and the estrogen-only study was not halted in 2002. However, in February 2004 it, too, was halted. While there was a 23% decreased incidence of breast cancer in the estrogen-only study participants, risks of stroke and pulmonary embolism were increased slightly, predominantly in patients who began HRT over the age of 60.[73]
Several other large studies and meta-analyses have reported reduced mortality for HRT in women younger than age 60 or within 10 years of menopause, and a debatable or absent effect on mortality in women over 60.[74][75][76][77][58][78]
Though research thus far has been substantial, further investigation is needed to fully understand differences in effect for different types of HRT and lengths of time since menopause.[79][80][18]
Society and public perception
Wyeth controversy
These favorable publications emphasized the benefits and downplayed the risks of its HRT products, especially the "misconception" of the association of its products with breast cancer.
Following the publication of the WHI data in 2002, the stock prices for the pharmaceutical industry plummeted, and huge numbers of women stopped using HRT.[84] The stocks of Wyeth, which supplied the Premarin and Prempro that were used in the WHI trials, decreased by more than 50%, and never fully recovered.[84] Some of their articles in response promoted themes such as the following: "the WHI was flawed; the WHI was a controversial trial; the population studied in the WHI was inappropriate or was not representative of the general population of menopausal women; results of clinical trials should not guide treatment for individuals; observational studies are as good as or better than randomized clinical trials; animal studies can guide clinical decision-making; the risks associated with hormone therapy have been exaggerated; the benefits of hormone therapy have been or will be proven, and the recent studies are an aberration."[60] Similar findings were observed in a 2010 analysis of 114 editorials, reviews, guidelines, and letters by five industry-paid authors.[60] These publications promoted positive themes and challenged and criticized unfavorable trials such as the WHI and MWS.[60] In 2009, Wyeth was acquired by Pfizer in a deal valued at US$68 billion.[85][86] Pfizer, a company that produces Provera and Depo-Provera (MPA) and has also engaged in medical ghostwriting, continues to market Premarin and Prempro, which remain best-selling medications.[60][83]
According to Fugh-Berman (2010), "Today, despite definitive scientific data to the contrary, many gynecologists still believe that the benefits of [HRT] outweigh the risks in asymptomatic women. This non-evidence–based perception may be the result of decades of carefully orchestrated corporate influence on medical literature."[82] As many as 50% of physicians have expressed skepticism about large trials like the WHI and HERS.[87] The positive perceptions of many physicians of HRT in spite of large trials showing risks that potentially outweigh any benefits may be due to the efforts of pharmaceutical companies like Wyeth.[83][60]
Popularity
The 1990s showed a dramatic decline in prescription rates, though more recently they have begun to rise again.[88][89]
See also
- Androgen replacement therapy
- Hormonal contraception
- Menopause
- Pharmacodynamics of progesterone
- Pharmacodynamics of estradiol
- Transgender hormone therapy (male-to-female)
References
- ^ S2CID 29118146.
- ^ PMID 20566620.
- ^ S2CID 24616324.
- PMID 19733988.
- ^
- ^
- ^ S2CID 3427944.
- ^ S2CID 207579406.
- ^ PMID 21531972.
- ^ a b "USPTF Consensus Statement". 2012.
- S2CID 20392538.
- PMID 22533363.
- ^ a b c d e f g Sarrel, P.M. (2000). Effects of hormone replacement therapy on sexual psychophysiology and behavior in postmenopause. Journal of Women’s Health and Gender-Based Medicine, 9, 25-32
- ^ "Menopause treatments". NHS. Retrieved 2018-02-23.
- PMID 28093732.
- ^ PMID 24084921.
- S2CID 26110755.
- ^ S2CID 33414205.
- ^ S2CID 38249709.
- PMID 12904517.
- PMID 25754617.
- S2CID 203464.
- PMID 26668177.
- S2CID 38526018.
- ^ PMID 23303565.
- ISBN 1-55009-163-8.
- PMID 25610174.
- S2CID 22921797.
- S2CID 43031351.
- ^ a b "Menopausal Hormone Therapy and Cancer Risk". www.cancer.org. Retrieved 4 March 2019.
- PMID 17333341.
- PMID 23062839.
- S2CID 3956784.
- ISSN 0027-8874.
- In turn citing: Hou, N.; Hong, S.; Wang, W.; Olopade, O. I.; Dignam, J. J.; Huo, D. (2013). "Hormone Replacement Therapy and Breast Cancer: Heterogeneous Risks by Race, Weight, and Breast Density". JNCI Journal of the National Cancer Institute. 105 (18): 1365–1372. PMID 24003037.
- In turn citing: Hou, N.; Hong, S.; Wang, W.; Olopade, O. I.; Dignam, J. J.; Huo, D. (2013). "Hormone Replacement Therapy and Breast Cancer: Heterogeneous Risks by Race, Weight, and Breast Density". JNCI Journal of the National Cancer Institute. 105 (18): 1365–1372.
- S2CID 20808536.
- ^ Management of the menopause after breast cancer Archived 2016-04-07 at archive.today, from The Royal Australian and New Zealand College of Obstetricians and Gynaecologists. College Statement C-Gyn 15. 1st Endorsed: February 2003. Current: November 2011. Review: November 2014
- .
- ^ S2CID 32195397.
- ^ S2CID 4229701.
- S2CID 205827003.
- ^ PMID 29149179.)
{{cite journal}}: CS1 maint: unflagged free DOI (link - PMID 12730248.
- PMID 18488873.)
{{cite journal}}: CS1 maint: unflagged free DOI (link - ^ Estrogen (Vaginal Route) from Mayo Clinic / Thomson Healthcare Inc. Portions of this document last updated: Nov. 1, 2011
- S2CID 29446836.
- S2CID 205452835.
- ^ PMID 21464264.
- ^ FDA. 2008-01-09. Retrieved 2009-02-17.
- S2CID 30292136.
- S2CID 30612542.
- PMID 28346192.
- S2CID 11410333.
- S2CID 25426141.
- ^ Lewis, Ricki. "ACOG Revises Guidelines on Treating Menopause Symptoms". login.medscape.com. Medscape. Retrieved 4 March 2019.
- ^ "Hormone Therapy and Heart Disease - ACOG". www.acog.org. Committee on Gynecologic Practice. Retrieved 4 March 2019.
- ^ "Medscape". www.medscape.com.
- ^ . Retrieved Jan 16, 2015.
- PMID 28703650. Retrieved 1 March 2019.
- ^ ISSN 2329-3691.
- ISBN 978-92-832-1291-1.
- ^ S2CID 20149703.
- PMID 19196674.
- PMID 23396275.
- ^ S2CID 25829459.
- ISBN 0-7817-4996-4.
- PMID 21117950.
- PMID 25922653.
- S2CID 16529377.
- ^ Mazzucco AE, Santoro E, DeSoto M, Lee JH (December 2010). "Hormone Therapy and Menopause". National Research Center for Women and Families.
- ^ Gina Kolata (2007-04-19). "Sharp Drop in Rates of Breast Cancer Holds". New York Times.
- ^ Roni Caryn Rabin (2007-08-28). "For a Low-Dose Hormone, Take Your Pick". New York Times.
Many women seeking natural remedies have turned to compounding pharmacies, which use bioidentical hormones that are chemically synthesized but with the same molecular structure as hormones produced by a woman's body.
- ^ John Gever (2011-04-05). "New WHI Estrogen Analysis Shows Lower Breast Ca Risk". MedPageToday.
- PMID 19854329.
- PMID 16815651.
- PMID 9718051.
- PMID 15209595.
- PMID 9187066.
- PMID 21252179.
- S2CID 37219662.
- ^ a b c d Singer, Natasha (4 August 2009). "Medical Papers by Ghostwriters Pushed Therapy". The New York Times. Retrieved 13 July 2018.
- ^ PMID 20838656.)
{{cite journal}}: CS1 maint: unflagged free DOI (link - ^ ISBN 978-1-4129-8309-9.
- ^ S2CID 207650230.
- ^ https://www.nytimes.com/2009/01/26/business/26drug.html
- ^ https://www.cnbc.com/id/33384753
- PMID 21949743.
- S2CID 205452835.
- ^ "Hormone therapy for brain performance: No effect, whether started early or late". www.sciencedaily.com.
External links
Category:Endocrine procedures Category:Life sciences industry Category:Menopause
